|
|
| [Code of Federal Regulations] |
| [Title 21, Volume 8] |
| [CITE: 21CFR866] |
TITLE 21--FOOD AND DRUGS CHAPTER I--FOOD AND DRUG ADMINISTRATION DEPARTMENT OF HEALTH AND HUMAN SERVICES
SUBCHAPTER H - MEDICAL DEVICES
| |
| PART 866 | IMMUNOLOGY AND MICROBIOLOGY DEVICES |
|
|
|
|
Subpart A - General Provisions
|
|
(a) This part sets forth the classification of immunology and microbiology devices intended for human use that are in commercial distribution.
(b) The indentification of a device in a regulation in this part is not a precise description of every device that is, or will be, subject to the regulation. A manufacturer who submits a premarket notification submission for a device under part 807 may not show merely that the device is accurately described by the section title and identification provisions of a regulation in this part, but shall state why the device is substantially equivalent to other devices, as required by § 807.87.
(c) To avoid duplicative listings, an immunology and microbiology device that has two or more types of uses (e.g., used both as a diagnostic device and as a microbiology device) is listed only in one subpart.
(d) References in this part to regulatory sections of the Code of Federal Regulations are to chapter I of title 21, unless otherwise noted.
(e) Guidance documents referenced in this part are available on the Internet at http://www.fda.gov/MedicalDevices/DeviceRegulationandGuidance/GuidanceDocuments/default.htm.
[52 FR 17733, May 11, 1987, as amended at 68 FR 5827, Feb. 5, 2003; 79 FR 50552, Aug. 25, 2014]
|
|
|
Sec. 866.3 Effective dates of requirement for premarket approval.
|
|
A device included in this part that is classified into class III (Premarket approval) shall not be commercially distributed after the date shown in the regulation classifying the device unless the manufacturer has an approval under section 515 of the act (unless an exemption has been granted under section 520(g)(2) of the act). An approval under section 515 of the act consists of FDA's issuance of an order approving an application for premarket approval (PMA) for the device or declaring completed a product development protocol (PDP) for the device.
(a) Before FDA requires that a device commercially distributed before the enactment date of the amendments, or a device that has been found substantially equivalent to such a device, has an approval under section 515 of the act FDA must promulgate a regulation under section 515(b) of the act requiring such approval, except as provided in paragraphs (b) and (c) of this section. Such a regulation under section 515(b) of the act shall not be effective during the grace period ending on the 90th day after its promulgation or on the last day of the 30th full calendar month after the regulation that classifies the device into class III is effective, whichever is later. See section 501(f)(2)(B) of the act. Accordingly, unless an effective date of the requirement for premarket approval is shown in the regulation for a device classified into class III in this part, the device may be commercially distributed without FDA's issuance of an order approving a PMA or declaring completed a PDP for the device. If FDA promulgates a regulation under section 515(b) of the act requiring premarket approval for a device, section 501(f)(1)(A) of the act applies to the device.
(b) Any new, not substantially equivalent, device introduced into commercial distribution on or after May 28, 1976, including a device formerly marketed that has been substantially altered, is classified by statute (section 513(f) of the act) into class III without any grace period and FDA must have issued an order approving a PMA or declaring completed a PDP for the device before the device is commercially distributed unless it is reclassified. If FDA knows that a device being commercially distributed may be a "new" device as defined in this section because of any new intended use or other reasons, FDA may codify the statutory classification of the device into class III for such new use. Accordingly, the regulation for such a class III device states that as of the enactment date of the amendments, May 28, 1976, the device must have an approval under section 515 of the act before commercial distribution.
(c) A device identified in a regulation in this part that is classified into class III and that is subject to the transitional provisions of section 520(l) of the act is automatically classified by statute into class III and must have an approval under section 515 of the act before being commercially distributed. Accordingly, the regulation for such a class III transitional device states that as of the enactment date of the amendments, May 28, 1976, the device must have an approval under section 515 of the act before commercial distribution.
[52 FR 17733, May 11, 1987; 52 FR 22577, June 12, 1987]
|
|
|
Sec. 866.9 Limitations of exemptions from section 510(k) of the Federal Food, Drug, and Cosmetic Act (the act).
|
|
The exemption from the requirement of premarket notification (section 510(k) of the act) for a generic type of class I or II device is only to the extent that the device has existing or reasonably foreseeable characteristics of commercially distributed devices within that generic type or, in the case of in vitro diagnostic devices, only to the extent that misdiagnosis as a result of using the device would not be associated with high morbidity or mortality. Accordingly, manufacturers of any commercially distributed class I or II device for which FDA has granted an exemption from the requirement of premarket notification must still submit a premarket notification to FDA before introducing or delivering for introduction into interstate commerce for commercial distribution the device when:
(a) The device is intended for a use different from the intended use of a legally marketed device in that generic type of device; e.g., the device is intended for a different medical purpose, or the device is intended for lay use where the former intended use was by health care professionals only;
(b) The modified device operates using a different fundamental scientific technology than a legally marketed device in that generic type of device; e.g., a surgical instrument cuts tissue with a laser beam rather than with a sharpened metal blade, or an in vitro diagnostic device detects or identifies infectious agents by using deoxyribonucleic acid (DNA) probe or nucleic acid hybridization technology rather than culture or immunoassay technology; or
(c) The device is an in vitro device that is intended:
(1) For use in the diagnosis, monitoring, or screening of neoplastic diseases with the exception of immunohistochemical devices;
(2) For use in screening or diagnosis of familial or acquired genetic disorders, including inborn errors of metabolism;
(3) For measuring an analyte that serves as a surrogate marker for screening, diagnosis, or monitoring life-threatening diseases such as acquired immune deficiency syndrome (AIDS), chronic or active hepatitis, tuberculosis, or myocardial infarction or to monitor therapy;
(4) For assessing the risk of cardiovascular diseases;
(5) For use in diabetes management;
(6) For identifying or inferring the identity of a microorganism directly from clinical material;
(7) For detection of antibodies to microorganisms other than immunoglobulin G (IgG) or IgG assays when the results are not qualitative, or are used to determine immunity, or the assay is intended for use in matrices other than serum or plasma;
(8) For noninvasive testing as defined in § 812.3(k) of this chapter; and
(9) For near patient testing (point of care).
[65 FR 2311, Jan. 14, 2000]
|
|
|
Subpart B - Diagnostic Devices
|
|
Sec. 866.1620 Antimicrobial susceptibility test disc.
|
|
(a) Identification. An antimicrobial susceptibility test disc is a device that consists of antimicrobic-impregnated paper discs used to measure by a disc-agar diffusion technique or a disc-broth elution technique the in vitro susceptibility of most clinically important bacterial pathogens to antimicrobial agents. In the disc-agar diffusion technique, bacterial susceptibility is ascertained by directly measuring the magnitude of a zone of bacterial inhibition around the disc on an agar surface. The disc-broth elution technique is associated with an automated rapid susceptibility test system and employs a fluid medium in which susceptibility is ascertained by photometrically measuring changes in bacterial growth resulting when antimicrobial material is eluted from the disc into the fluid medium. Test results are used to determine the antimicrobial agent of choice in the treatment of bacterial diseases.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.1640 Antimicrobial susceptibility test powder.
|
|
(a) Identification. An antimicrobial susceptibility test powder is a device that consists of an antimicrobial drug powder packaged in vials in specified amounts and intended for use in clinical laboratories for determining in vitro susceptibility of bacterial pathogens to these therapeutic agents. Test results are used to determine the antimicrobial agent of choice in the treatment of bacterial diseases.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.1645 Fully automated short-term incubation cycle antimicrobial susceptibility system.
|
|
(a) Identification. A fully automated short-term incubation cycle antimicrobial susceptibility system is a device that incorporates concentrations of antimicrobial agents into a system for the purpose of determining in vitro susceptibility of bacterial pathogens isolated from clinical specimens. Test results obtained from short-term (less than 16 hours) incubation are used to determine the antimicrobial agent of choice to treat bacterial diseases.
(b) Classification. Class II (special controls). The special control for this device is FDA's guidance document entitled "Class II Special Controls Guidance Document: Antimicrobial Susceptibility Test (AST) Systems; Guidance for Industry and FDA."
[68 FR 5827, Feb. 5, 2003]
|
|
|
Sec. 866.1655 System for detection of microorganisms and antimicrobial resistance using reporter expression.
|
|
(a) Identification. A system for detection of microorganisms and antimicrobial resistance using reporter expression is an in vitro diagnostic device intended for the detection and identification of live microorganisms and the detection of associated antimicrobial drug susceptibility or resistance in specimens from patients at risk of colonization or suspected of infection.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The intended use for the device in the labeling required under § 809.10 of this chapter must include a detailed description of the targets the device detects, the type of results provided to the user, the clinical indications appropriate for test use, and the specific population(s) for which the device is intended.
(2) Any device used for specimen collection and transport must be FDA-cleared, approved, or -classified as 510(k) exempt (standalone or as part of a test system) for the collection of the specimen types claimed by this device and for the maintenance of viability of the targeted microorganisms; alternatively, the specimen collection device must be cleared in a premarket submission as a part of this device.
(3) The labeling required under § 809.10(b) of this chapter must include:
(i) A detailed description of the device, including reagents, instruments, ancillary materials, applicable specimen collection and transport device(s) and control elements, and a detailed explanation of the methodology, including all pre-analytical methods for handling and processing of specimens and controls to maintain organism viability;
(ii) Detailed descriptions of the test procedure, including the preparation and maintenance of quality controls and the interpretation of test results;
(iii) Detailed discussion of the performance characteristics of the device for all claimed organisms and specimen types based on analytical studies, including evaluation of analytical sensitivity, inclusivity, cross-reactivity, potentially interfering substances and microorganisms, contamination, specimen stability, precision, and reproducibility;
(iv) Detailed discussion of the performance characteristics of the device observed in a clinical study performed on a population that is consistent with the intended use population in comparison to the results obtained by a reference or comparator method determined to be acceptable by FDA, for microbial detection, identification, and antimicrobial susceptibility testing; and
(v) A limiting statement indicating that a negative test result does not preclude colonization or infection with organisms that do not express detectable levels of the reporter that is identified by the device.
(4) Design verification and validation must include:
(i) A detailed description of the device, including an explanation of the technology, hardware, software, and consumables, as well as an explanation of the result algorithms and method(s) of data processing from signal acquisition to result assignment;
(ii) A detailed description of the impact of any software, including software applications and hardware-based devices that incorporate software, on the device's functions;
(iii) Detailed documentation of the analytical and clinical studies required in paragraphs (b)(3)(iii) and (iv) of this section, including the study protocols containing descriptions of the test methods, prescribed methods of data analysis and acceptance criteria, final study reports, and data line listings;
(iv) Detailed documentation of quality control procedures, including an explanation of how quality control materials were selected, the recommended frequency of testing, methods of control preparation, acceptance criteria for performance and the results from quality control testing performed during the analytical and clinical studies required under paragraphs (b)(3)(iii) and (iv) of this section;
(v) Detailed documentation of studies performed to establish onboard and in-use reagent stability, including the test method(s), data analysis plans, acceptance criteria, final study reports, and data line listings;
(vi) Detailed documentation of studies to establish reagent shelf-life for the assay kit and each applicable specimen collection and transport device, including study protocols containing descriptions of the test method(s), data analysis plans, and acceptance criteria; and
(vii) Documentation of an appropriate end user device training program that will be offered as part of efforts to assure appropriate conduct of the assay and to mitigate the risk associated with false results, including failure to use the device correctly or correctly interpret results.
[87 FR 6417, Feb. 4, 2022]
|
|
|
Sec. 866.1700 Culture medium for antimicrobial susceptibility tests.
|
|
(a) Identification. A culture medium for antimicrobial susceptibility tests is a device intended for medical purposes that consists of any medium capable of supporting the growth of many of the bacterial pathogens that are subject to antimicrobial susceptibility tests. The medium should be free of components known to be antagonistic to the common agents for which susceptibility tests are performed in the treatment of disease.
(b) Classification. Class II (performance standards).
|
|
|
Subpart C - Microbiology Devices
|
|
Sec. 866.2050 Staphylococcal typing bacteriophage.
|
|
(a) Identification. A staphylococcal typing bacteriophage is a device consisting of a bacterial virus intended for medical purposes to identify pathogenic staphylococcal bacteria through use of the bacteria's susceptibility to destruction by the virus. Test results are used principally for the collection of epidemiological information.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25045, June 12, 1989; 66 FR 38790, July 25, 2001]
|
|
|
Sec. 866.2120 Anaerobic chamber.
|
|
(a) Identification. An anaerobic chamber is a device intended for medical purposes to maintain an anaerobic (oxygen free) environment. It is used to isolate and cultivate anaerobic microorganisms.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9. The device is also exempt from the good manufacturing practice requirements of the quality system regulation in part 820 of this chapter, with the exception of § 820.180, with respect to general requirements concerning records, and § 820.198, with respect to complaint files.
[47 FR 50823, Nov. 9, 1982, as amended at 66 FR 38790, July 25, 2001]
|
|
|
Sec. 866.2160 Coagulase plasma.
|
|
(a) Identification. Coagulase plasma is a device that consists of freeze-dried animal or human plasma that is intended for medical purposes to perform coagulase tests primarily on staphylococcal bacteria. When reconstituted, the fluid plasma is clotted by the action of the enzyme coagulase which is produced by pathogenic staphylococci. Test results are used primarily as an aid in the diagnosis of disease caused by pathogenic bacteria belonging to the genus Staphylococcus and provide epidemiological information on disease caused by these microorganisms.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 61 FR 1119, Jan. 16, 1996; 66 FR 38790, July 25, 2001]
|
|
|
Sec. 866.2170 Automated colony counter.
|
|
(a) Identification. An automated colony counter is a mechanical device intended for medical purposes to determine the number of bacterial colonies present on a bacteriological culture medium contained in a petri plate. The number of colonies counted is used in the diagnosis of disease as a measure of the degree of bacterial infection.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25045, June 12, 1989; 66 FR 38790, July 25, 2001]
|
|
|
Sec. 866.2180 Manual colony counter.
|
|
(a) Identification. A manual colony counter is a device intended for medical purposes that consists of a printed grid system superimposed on an illuminated screen. Petri plates containing bacterial colonies to be counted are placed on the screen for better viewing and ease of counting. The number of colonies counted is used in the diagnosis of disease as a measure of the degree of bacterial infection.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9. The device is also exempt from the good manufacturing practice requirements of the quality system regulation in part 820 of this chapter, with the exception of § 820.180, with respect to general requirements concerning records, and § 820.198, with respect to complaint files.
[47 FR 50823, Nov. 9, 1982, as amended at 66 FR 38790, July 25, 2001]
|
|
|
Sec. 866.2190 Automated image assessment system for microbial colonies on solid culture media.
|
|
(a) Identification. An automated image assessment system for microbial colonies on solid culture media is a system that is intended to assess the presence or absence of microbial colonies on solid microbiological culture medium, and to interpret their number, and phenotypic and morphologic characteristics through analysis of two dimensional digital images as an aid in diagnosis of infectious disease.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include a detailed description of the device, including the technology employed, components and software modules, as well as a detailed explanation of the result algorithms and any expert rules that are used to assess colony characteristics and enumerate colonies from image capture through end result.
(2) Premarket notification submissions must include detailed documentation of the analytical studies performed to characterize device performance to support the intended use, as appropriate.
(3) Premarket notification submissions must include detailed documentation from clinical studies performed on a population that is consistent with the intended use population.
(i) The clinical studies must establish the device performance based on comparison to results obtained by an acceptable reference method, as appropriate.
(ii) The clinical study documentation must include the study protocol with a predefined statistical analysis plan and the final report documenting support for the Indications for Use and the results of the statistical analysis, as appropriate.
(4) Premarket notification submissions must include detailed documentation for device software, including but not limited to software applications and hardware based components that incorporate software, and any decision-making thresholds used to generate results for the device. If a part of a Total Laboratory Automation System, the premarket notification submission must include detailed documentation addressing the instrument and software system integration.
(5) Premarket notification submissions must include detailed documentation of appropriate instructions for use regarding the intended user's device quality control procedures for the instrument system and components, as appropriate.
(6) The 21 CFR 809.10 compliant device labeling must include:
(i) Detailed user instructions to mitigate the risk of failure to operate the instrument correctly.
(ii) A detailed explanation of the interpretation of results and limitations regarding the need for review of culture plates by a qualified microbiologist, as appropriate.
(iii) A summary of performance data obtained from the analytical studies used to support device performance, as appropriate.
(iv) A summary of performance data obtained from clinical studies performed on a population that is consistent with the intended use population, as appropriate.
(7) Under 21 CFR 820.30 compliant design control, device manufacturers must, as appropriate:
(i) Conduct human factors/usability validation testing with the final version of the labeling and related materials to adequately mitigate the risk of failure to operate the instrument correctly.
(ii) Document a device training program that will be offered to the end user to adequately mitigate the risk of failure to operate the instrument correctly.
[82 FR 47969, Oct. 16, 2017]
|
|
|
Sec. 866.2300 Multipurpose culture medium.
|
|
(a) Identification. A multipurpose culture medium is a device that consists primarily of liquid or solid biological materials intended for medical purposes for the cultivation and identification of several types of pathogenic microorganisms without the need of additional nutritional supplements. Test results aid in the diagnosis of disease and also provide epidemiological information on diseases caused by these microorganisms.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38790, July 25, 2001]
|
|
|
Sec. 866.2320 Differential culture medium.
|
|
(a) Identification. A differential culture medium is a device that consists primarily of liquid biological materials intended for medical purposes to cultivate and identify different types of pathogenic microorganisms. The identification of these microorganisms is accomplished by the addition of a specific biochemical component(s) to the medium. Microorganisms are identified by a visible change (e.g., a color change) in a specific biochemical component(s) which indicates that specific metabolic reactions have occurred. Test results aid in the diagnosis of disease and also provide epidemiological information on diseases caused by these microorganisms.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38790, July 25, 2001]
|
|
|
Sec. 866.2330 Enriched culture medium.
|
|
(a) Identification. An enriched culture medium is a device that consists primarily of liquid or solid biological materials intended for medical purposes to cultivate and identify fastidious microorganisms (those having complex nutritional requirements). The device consists of a relatively simple basal medium enriched by the addition of such nutritional components as blood, blood serum, vitamins, and extracts of plant or animal tissues. The device is used in the diagnosis of disease caused by pathogenic microorganisms and also provides epidemiological information on these diseases.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2350 Microbiological assay culture medium.
|
|
(a) Identification. A microbiological assay culture medium is a device that consists primarily of liquid or solid biological materials intended for medical purposes to cultivate selected test microorganisms in order to measure by microbiological procedures the concentration in a patient's serum of certain substances, such as amino acids, antimicrobial agents, and vitamins. The concentration of these substances is measured by their ability to promote or inhibit the growth of the test organism in the innoculated medium. Test results aid in the diagnosis of disease resulting from either deficient or excessive amounts of these substances in a patient's serum. Tests results may also be used to monitor the effects of the administration of certain antimicrobial drugs.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2360 Selective culture medium.
|
|
(a) Identification. A selective culture medium is a device that consists primarily of liquid or solid biological materials intended for medical purposes to cultivate and identify certain pathogenic microorganisms. The device contains one or more components that suppress the growth of certain microorganisms while either promoting or not affecting the growth of other microorganisms. The device aids in the diagnosis of disease caused by pathogenic microorganisms and also provides epidemiological information on these diseases.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2390 Transport culture medium.
|
|
(a) Identification. A transport culture medium is a device that consists of a semisolid, usually non-nutrient, medium that maintains the viability of suspected pathogens contained in patient specimens while in transit from the specimen collection area to the laboratory. The device aids in the diagnosis of disease caused by pathogenic microorganisms and also provides epidemiological information on these diseases.
(b) Classification. Class I (general controls).
|
|
|
Sec. 866.2410 Culture medium for pathogenic Neisseria spp.
|
|
(a) Identification. A culture medium for pathogenic Neisseria spp. is a device that consists primarily of liquid or solid biological materials used to cultivate and identify pathogenic Neisseria spp. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Neisseria, such as epidemic cerebrospinal meningitis, other meningococcal disease, and gonorrhea, and also provides epidemiological information on these microorganisms.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.2420 Oxidase screening test for gonorrhea.
|
|
(a) Identification. An oxidase screening test for gonorrhea is an in vitro device that consists of the articles intended to identify by chemical reaction, cytochrome oxidase, an oxidizing enzyme that is associated with certain bacteria including Neisseria gonorrhoeae. A sample of a male's urethral discharge is obtained on a swab which is placed into a wetting agent containing an ingredient that will react with cytochrome oxidase. When cytochrome oxidase is present, the swab turns a dark purple color within 3 minutes. Because it is unlikely that cytochrome oxidase-positive organisms other than Neisseria gonorrhoeae are present in the urethral discharge of males, the identification of cytochrome oxidase with this device indicates presumptive infection of the patient with the causative agent of gonorrhea.
(b) Classification. Class III (premarket approval) (transitional device).
(c) Date PMA or notice of completion of a PDP is required. As of May 28, 1976, an approval under section 515 of the act is required before this device may be commercially distributed. See § 866.3.
[47 FR 50823, Nov. 9, 1982, as amended at 52 FR 17734, May 11, 1987]
|
|
|
Sec. 866.2440 Automated medium dispensing and stacking device.
|
|
(a) Identification. An automated medium dispensing and stacking device is a device intended for medical purposes to dispense a microbiological culture medium into petri dishes and then mechanically stack the petri dishes.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9. The device is also exempt from the good manufacturing practice requirements of the quality system regulation in part 820 of this chapter, with the exception of § 820.180, with respect to general requirements concerning records, and § 820.198, with respect to complaint files.
[47 FR 50823, Nov. 9, 1982, as amended at 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2450 Supplement for culture media.
|
|
(a) Identification. A supplement for culture media is a device, such as a vitamin or sugar mixture, that is added to a solid or liquid basal culture medium to produce a desired formulation and that is intended for medical purposes to enhance the growth of fastidious microorganisms (those having complex nutritional requirements). This device aids in the diagnosis of diseases caused by pathogenic microorganisms.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2480 Quality control kit for culture media.
|
|
(a) Identification. A quality control kit for culture media is a device that consists of paper discs (or other suitable materials), each impregnated with a specified, freeze-dried, viable microorganism, intended for medical purposes to determine if a given culture medium is able to support the growth of that microorganism. The device aids in the diagnosis of disease caused by pathogenic microorganisms and also provides epidemiological information on these diseases.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2500 Microtiter diluting and dispensing device.
|
|
(a) Identification. A microtiter diluting and dispensing device is a mechanical device intended for medical purposes to dispense or serially dilute very small quantities of biological or chemical reagents for use in various diagnostic procedures.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2540 Microbiological incubator.
|
|
(a) Identification. A microbiological incubator is a device with various chambers or water-filled compartments in which controlled environmental conditions, particularly temperature, are maintained. It is intended for medical purposes to cultivate microorganisms and aid in the diagnosis of disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9. The device is also exempt from the good manufacturing practice requirements of the quality system regulation in part 820 of this chapter, with the exception of § 820.180, with respect to general requirements concerning records, and § 820.198, with respect to complaint files.
[47 FR 50823, Nov. 9, 1982, as amended at 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2560 Microbial growth monitor.
|
|
(a) Identification. A microbial growth monitor is a device intended for medical purposes that measures the concentration of bacteria suspended in a liquid medium by measuring changes in light scattering properties, optical density, electrical impedance, or by making direct bacterial counts. The device aids in the diagnosis of disease caused by pathogenic microorganisms.
(b) Classification. Class I. With the exception of automated blood culturing system devices that are used in testing for bacteria, fungi, and other microorganisms in blood and other normally sterile body fluids, this device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter.
[47 FR 50823, Nov. 9, 1982, as amended at 60 FR 38482, July 27, 1995]
|
|
|
Sec. 866.2580 Gas-generating device.
|
|
(a) Identification. A gas-generating device is a device intended for medical purposes that produces predetermined amounts of selected gases to be used in a closed chamber in order to establish suitable atmospheric conditions for cultivation of microorganisms with special atmospheric requirements. The device aids in the diagnosis of disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2600 Wood's fluorescent lamp.
|
|
(a) Identification. A Wood's fluorescent lamp is a device intended for medical purposes to detect fluorescent materials (e.g., fluorescein pigment produced by certain microorganisms) as an aid in the identification of these microorganisms. The device aids in the diagnosis of disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9. The device is also exempt from the good manufacturing practice requirements of the quality system regulation in part 820 of this chapter, with the exception of § 820.180, with respect to general requirements concerning records, and § 820.198, with respect to complaint files.
[47 FR 50823, Nov. 9, 1982, as amended at 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.2660 Microorganism differentiation and identification device.
|
|
(a) Identification. A microorganism differentiation and identification device is a device intended for medical purposes that consists of one or more components, such as differential culture media, biochemical reagents, and paper discs or paper strips impregnated with test reagents, that are usually contained in individual compartments and used to differentiate and identify selected microorganisms. The device aids in the diagnosis of disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.2680 Streptococcus spp. nucleic acid-based assay.
|
|
(a) Identification. A Streptococcus spp. nucleic acid-based assay is a qualitative in vitro diagnostic device intended to simultaneously detect and identify various Streptococcus spp. nucleic acids extracted directly from clinical specimens. The device detects specific nucleic acid sequences for organism identification. The identification aids in the diagnosis of diseases caused by bacteria belonging to the genus Streptococcus and provides epidemiological information on these diseases. Pathogenic streptococci are associated with infections, such as sore throat, impetigo (an infection characterized by small pustules on the skin), urinary tract infections, rheumatic fever, and kidney disease.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include detailed device description documentation, including the device components, ancillary reagents required but not provided, and a detailed explanation of the methodology including primer/probe sequence, design, and rationale for sequence selection.
(2) Premarket notification submissions must include detailed documentation from the following analytical and clinical performance studies: Analytical sensitivity (Limit of Detection), reactivity, inclusivity, precision, reproducibility, interference, cross reactivity, carry-over, and cross contamination.
(3) Premarket notification submissions must include detailed documentation from a clinical study. The study, performed on a study population consistent with the intended use population, must compare the device performance to results obtained from well-accepted reference methods.
(4) Premarket notification submissions must include detailed documentation for device software, including, but not limited to, software applications and hardware-based devices that incorporate software.
(5) Premarket notification submissions must include database implementation methodology, construction parameters, and quality assurance protocols, as appropriate.
(6) The device labeling must include limitations regarding the need for culture confirmation of negative specimens, as appropriate.
(7) A detailed explanation of the interpretation of results and acceptance criteria must be included in the device's 21 CFR 809.10(b)(9) compliant labeling.
(8) Premarket notification submissions must include details on an end user device training program that will be offered while marketing the device, as appropriate.
[82 FR 50074, Oct. 30, 2017]
|
|
|
Sec. 866.2850 Automated zone reader.
|
|
(a) Identification. An automated zone reader is a mechanical device intended for medical purposes to measure zone diameters of microbial growth inhibition (or exhibition), such as those observed on the surface of certain culture media used in disc-agar diffusion antimicrobial susceptibility tests. The device aids in decisionmaking respecting the treatment of disease.
(b) Classification. Class I (general controls).
|
|
|
Sec. 866.2900 Microbiological specimen collection and transport device.
|
|
(a) Identification. A microbiological specimen collection and transport device is a specimen collecting chamber intended for medical purposes to preserve the viability or integrity of microorganisms in specimens during storage of specimens after their collection and during their transport from the collecting area to the laboratory. The device may be labeled or otherwise represented as sterile. The device aids in the diagnosis of disease caused by pathogenic microorganisms.
(b) Classification. Class I (general controls). The device, when solely intended for use in the collection of concentrated parasites from specimens and transport, is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 84 FR 71800, Dec. 30, 2019; 85 FR 18445, Apr. 2, 2020]
|
|
|
Subpart D - Serological Reagents
|
|
Sec. 866.3010 Acinetobacter calcoaceticus serological reagents.
|
|
(a) Identification. Acinetobacter calcoaceticus serological reagents are devices that consist of Acinetobacter calcoaceticus antigens and antisera used to identify this bacterium from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of disease caused by the bacterium Acinetobacter calcoaceticus and provides epidemiological information on disease caused by this microorganism. This organism becomes pathogenic in patients with burns or with immunologic deficiency, and infection can result in sepsis (blood poisoning).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3020 Adenovirus serological reagents.
|
|
(a) Identification. Adenovirus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to adenovirus in serum. Additionally, some of these reagents consist of adenovirus antisera conjugated with a fluorescent dye and are used to identify adenoviruses directly from clinical specimens. The identification aids in the diagnosis of disease caused by adenoviruses and provides epidemiological information on these diseases. Adenovirus infections may cause pharyngitis (inflammation of the throat), acute respiratory diseases, and certain external diseases of the eye (e.g., conjunctivitis).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3035 Arizona spp. serological reagents.
|
|
(a) Identification. Arizona spp. serological reagents are devices that consist of antisera and antigens used to identify Arizona spp. in cultured isolates derived from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Arizona and provides epidemiological information on diseases caused by these microorganisms. Arizona spp. can cause gastroenteritis (food poisoning) and sepsis (blood poisoning).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3040 Aspergillus spp. serological reagents.
|
|
(a) Identification. Aspergillus spp. serological reagents are devices that consist of antigens and antisera used in various serological tests to identify antibodies to Aspergillus spp. in serum. The identification aids in the diagnosis of aspergillosis caused by fungi belonging to the genus Aspergillus. Aspergillosis is a disease marked by inflammatory granulomatous (tumor-like) lessions in the skin, ear, eyeball cavity, nasal sinuses, lungs, and occasionally the bones.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3045 In vitro diagnostic device for Bacillus spp. detection.
|
|
(a) Identification. An in vitro diagnostic device for Bacillus species (spp.) detection is a prescription device used to detect and differentiate among Bacillus spp. and presumptively identify B. anthracis and other Bacillus spp. from cultured isolates or clinical specimens as an aid in the diagnosis of anthrax and other diseases caused by Bacillus spp. This device may consist of Bacillus spp. antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to presumptively identify bacillus-like organisms in clinical specimens; bacteriophage used for differentiating B. anthracis from other Bacillus spp. based on susceptibility to lysis by the phage; or antigens used to identify antibodies to B. anthracis (anti-toxin and anti-capsular) in serum. Bacillus infections include anthrax (cutaneous, inhalational, or gastrointestinal) caused by B. anthracis, and gastrointestinal disease and non-gastrointestinal infections caused by B. cereus.
(b) Classification. Class II (special controls). The special controls are set forth in FDA's special controls guideline document entitled "In Vitro Diagnostic Devices for Bacillus spp. Detection; Class II Special Controls Guideline for Industry and Food and Drug Administration Staff." For availability of the guideline document, see § 866.1(e).
(c) Restriction on Distribution. The distribution of these devices is limited to laboratories that follow public health guidelines that address appropriate biosafety conditions, interpretation of test results, and coordination of findings with public health authorities.
(d) Restriction on Use. The use of this device is restricted to prescription use and must comply with the following:
(1) The device must be in the possession of:
(i)(A) A person, or his agents or employees, regularly and lawfully engaged in the manufacture, transportation, storage, or wholesale or retail distribution of such device; or
(B) A practitioner, such as a physician, licensed by law to use or order the use of such device; and
(ii) The device must be sold only to or on the prescription or other order of such practitioner for use in the course of his professional practice.
(2) The label of the device shall bear the statement "Caution: Federal law restricts this device to sale by or on the order of a ____", the blank to be filled with the word "physician" or with the descriptive designation of any other practitioner licensed by the law of the State in which he practices to use or order the use of the device.
(3) Any labeling, as defined in section 201(m) of the Federal Food, Drug, and Cosmetic Act, whether or not it is on or within a package from which the device is to be dispensed, distributed by, or on behalf of the manufacturer, packer, or distributor of the device, that furnishes or purports to furnish information for use of the device contains adequate information for such use, including indications, effects, routes, methods, and frequency and duration of administration and any relevant hazards, contraindications, side effects, and precautions, under which practitioners licensed by law to employ the device can use the device safely and for the purposes for which it is intended, including all purposes for which it is advertised or represented. This information will not be required on so-called reminder-piece labeling which calls attention to the name of the device but does not include indications or other use information.
(4) All labeling, except labels and cartons, bearing information for use of the device also bears the date of the issuance or the date of the latest revision of such labeling.
[84 FR 12088, Apr. 1, 2019]
|
|
|
Sec. 866.3050 Beta-glucan serological assays.
|
|
(a) Identification. Beta-glucan serological assays are devices that consist of antigens or proteases used in serological assays. The device is intended for use for the presumptive diagnosis of fungal infection. The assay is indicated for use in patients with symptoms of, or medical conditions predisposing the patient to invasive fungal infection. The device can be used as an aid in the diagnosis of deep seated mycoses and fungemias.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: Serological Assays for the Detection of Beta-Glucan." See § 866.1(e) for the availability of this guidance document.
[69 FR 56936, Sept. 23, 2004]
|
|
|
Sec. 866.3060 Blastomyces dermatitidis serological reagents.
|
|
(a) Identification. Blastomyces dermatitidis serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Blastomyces determatitidis in serum. The identification aids in the diagnosis of blastomycosis caused by the fungus Blastomyces dermatitidis. Blastomycosis is a chronic granulomatous (tumor-like) disease, which may be limited to the skin or lung or may be widely disseminated in the body resulting in lesions of the bones, liver, spleen, and kidneys.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59226, Nov. 3, 1998]
|
|
|
Sec. 866.3065 Bordetella spp. serological reagents.
|
|
(a) Identification. Bordetella spp. serological reagents are devices that consist of antigens and antisera, including antisera conjugated with a fluorescent dye, used in serological tests to identify Bordetella spp. from cultured isolates or directly from clinical specimens. The identification aids in the diagnosis of diseases caused by bacteria belonging to the genus Bordetella and provides epidemiological information on these diseases. Bordetella spp. cause whooping cough (Bordetella pertussis ) and other similiarly contagious and acute respiratory infections characterized by pneumonitis (inflammation of the lungs).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3085 Brucella spp. serological reagents.
|
|
(a) Identification. Brucella spp. serological reagents are devices that consist of antigens and antisera used for serological identification of Brucella spp. from cultured isolates derived from clinical specimens or to identify antibodies to Brucella spp. in serum. Additionally, some of these reagents consist of antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Brucella spp. directly from clinical specimens or cultured isolates derived from clinical specimens. The identification aids in the diagnosis of brucellosis (e.g., undulant fever, Malta fever) caused by bacteria belonging to the genus Brucella and provides epidemiological information on diseases caused by these microorganisms.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59226, Nov. 3, 1998]
|
|
|
Sec. 866.3110 Campylobacter fetus serological reagents.
|
|
(a) Identification. Campylobacter fetus serological reagents are devices that consist of antisera conjugated with a fluorescent dye used to identify Campylobacter fetus from clinical specimens or cultured isolates derived from clinical specimens. The identification aids in the diagnosis of diseases caused by this bacterium and provides epidemiological information on these diseases. Campylobacter fetus is a frequent cause of abortion in sheep and cattle and is sometimes responsible for endocarditis (inflammation of certain membranes of the heart) and enteritis (inflammation of the intestines) in humans.
(b) Classification. Class I (general controls).
|
|
|
Sec. 866.3120 Chlamydia serological reagents.
|
|
(a) Identification. Chlamydia serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to chlamydia in serum. Additionally, some of these reagents consist of chlamydia antisera conjugated with a fluorescent dye used to identify chlamydia directly from clinical specimens or cultured isolates derived from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Chlamydia and provides epidemiological information on these diseases. Chlamydia are the causative agents of psittacosis (a form of pneumonia), lymphogranuloma venereum (a venereal disease), and trachoma (a chronic disease of the eye and eyelid).
(b) Classification. Class I (general controls).
|
|
|
Sec. 866.3125 Citrobacter spp. serological reagents.
|
|
(a) Identification. Citrobacter spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify Citrobacter spp. from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Citrobacter and provides epidemiological information on diseases caused by these microorganisms. Citrobacter spp. have occasionally been associated with urinary tract infections.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3130 Clostridium difficile toxin gene amplification assay.
|
|
(a) Identification. A Clostridium difficile toxin gene amplification assay is a device that consists of reagents for the amplification and detection of target sequences in Clostridium difficile toxin genes in fecal specimens from patients suspected of having Clostridium difficile infection (CDI). The detection of clostridial toxin genes, in conjunction with other laboratory tests, aids in the clinical laboratory diagnosis of CDI caused by Clostridium difficile.
(b) Classification. Class II (special controls). The special controls are set forth in FDA's guideline document entitled: "Class II Special Controls Guideline: Toxin Gene Amplification Assays for the Detection of Clostridium difficile; Guideline for Industry and Food and Drug Administration Staff." See § 866.1(e) for information on obtaining this document.
[80 FR 51939, Aug. 27, 2015]
|
|
|
Sec. 866.3135 Coccidioides immitis serological reagents.
|
|
(a) Identification. Coccidioides immitis serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Coccidioides immitis in serum. The identification aids in the diagnosis of coccidioidomycosis caused by a fungus belonging to the genus Coccidioides and provides epidemiological information on diseases caused by this microorganism. An infection with Coccidioides immitis produces symptoms varying in severity from those accompanying the common cold to those of influenza.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59226, Nov. 3, 1998]
|
|
|
Sec. 866.3140 Corynebacterium spp. serological reagents.
|
|
(a) Identification. Corynebacterium spp. serological reagents are devices that consist of antisera conjugated with a fluorescent dye used to identify Corynebacterium spp. from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Corynebacterium and provides epidemiological information on diseases caused by these microorganisms. The principal human pathogen of this genus, Corynebacterium diphtheriae, causes diphtheria. However, many other types of corynebacteria form part of the normal flora of the human respiratory tract, other mucus membranes, and skin, and are either nonpathogenic or have an uncertain role.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3145 Coxsackievirus serological reagents.
|
|
(a) Identification. Coxsackievirus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to coxsackievirus in serum. Additionally, some of these reagents consist of coxsackievirus antisera conjugated with a fluorescent dye that are used to identify coxsackievirus from clinical specimens or from tissue culture isolates derived from clinical specimens. The identification aids in the diagnosis of coxsackievirus infections and provides epidemiological information on diseases caused by these viruses. Coxsackieviruses produce a variety of infections, including common colds, meningitis (inflammation of brain and spinal cord membranes), herpangina (brief fever accompanied by ulcerated lesions of the throat), and myopericarditis (inflammation of heart tissue).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3165 Cryptococcus neoformans serological reagents.
|
|
(a) Identification. Cryptococcus neoformans serological reagents are devices that consist of antigens used in serological tests to identify antibodies to Cryptococcus neoformans in serum. Additionally, some of these reagents consist of antisera conjugated with a fluorescent dye (immunofluorescent reagents) and are used to identify Cryptococcus neoformans directly from clinical specimens or from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of cryptococcosis and provides epidemiological information on this type of disease. Cryptococcosis infections are found most often as chronic meningitis (inflammation of brain membranes) and, if not treated, are usually fatal.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59226, Nov. 3, 1998]
|
|
|
Sec. 866.3169 Hepatitis C virus antibody tests.
|
|
(a) Identification. A hepatitis C virus (HCV) antibody test is identified as an in vitro diagnostic device intended for use with human serum, plasma, or other matrices as a prescription device that aids in the diagnosis of HCV infection in persons with signs and symptoms of hepatitis and in persons at risk for hepatitis C infection. The test is not intended for screening blood, plasma, cell, or tissue donors.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The labeling required under § 809.10(b) of this chapter must include:
(i) A prominent statement that the test is not intended for the screening of blood, plasma, and cell or tissue donors.
(ii) Limitations, which must be updated to reflect current clinical practice and disease presentation and management. The limitations must include, but are not limited to, statements that indicate:
(A) When appropriate, the performance characteristics of the test have not been established in populations of immunocompromised or immunosuppressed patients or, other special populations where test performance may be affected.
(B) The detection of HCV antibodies indicates a present or past infection with hepatitis C virus, but does not differentiate between acute, chronic, or resolved infection.
(C) The specimen types for which the device has been cleared, and that use of the test with specimen types other than those specifically cleared for this device may result in inaccurate test results.
(D) Test results are to be interpreted by qualified licensed healthcare professionals in conjunction with the individual's clinical presentation, history, and other laboratory results.
(E) A non-reactive test result may occur early during acute infection, prior to development of a host antibody response to infection, or when analyte levels are below the limit of detection of the test.
(iii) A detailed explanation of the principles of operation and procedures for performing the test.
(2) Design verification and validation must include the following:
(i) A detailed device description, including all parts that make up the device, ancillary reagents required but not provided, an explanation of the device methodology, and design of the antigen(s) and capture antibody(ies) sequences, rationale for the selected epitope(s), degree of amino acid sequence conservation of the target, and the design and nature of all primary, secondary, and subsequent standards used for calibration.
(ii) Documentation and characterization (e.g., supplier, determination of identity, and stability) of all critical reagents (including description of the antigen(s) and capture antibody(ies)), and protocols for maintaining product integrity throughout its labeled shelf life.
(iii) Risk analysis and management strategies, such as Failure Modes Effects Analysis and/or Hazard Analysis and Critical Control Points summaries and their impact on test performance.
(iv) Final release criteria to be used for manufactured test lots with appropriate evidence that lots released at the extremes of the specifications will meet the claimed analytical and clinical performance characteristics as well as the stability claims.
(v) Stability studies for reagents must include documentation of an assessment of real-time stability for multiple reagent lots using the indicated specimen types and must use acceptance criteria that ensure that analytical and clinical performance characteristics are met when stability is assigned based on the extremes of the acceptance range.
(vi) All stability protocols, including acceptance criteria.
(vii) Final release test results for each lot used in clinical studies.
(viii) Multisite reproducibility study that includes the testing of three independent production lots.
(ix) Analytical performance studies and results for determining the limit of blank (LoB), limit of detection (LoD), cutoff, precision (reproducibility) including lot-to-lot and/or instrument-to-instrument precision, interference, cross reactivity, carryover, hook effect, seroconversion panel testing, matrix equivalency, specimen stability, reagent stability, and cross-genotype antibody detection sensitivity, when appropriate.
(x) Analytical sensitivity of the test is the same or better than that of other cleared or approved tests.
(xi) Detailed documentation of clinical performance testing from a multisite clinical study. Performance must be analyzed relative to an FDA cleared or approved HCV antibody test, or a comparator that FDA has determined is appropriate. This study must be conducted using appropriate patient samples, with an acceptable number of HCV positive and negative samples in applicable risk categories. Additional relevant patient groups must be validated as appropriate. The samples may be a combination of fresh and repository samples, sourced from geographically diverse areas. The study designs, including number of samples tested, must be sufficient to meet the following criteria:
(A) Clinical sensitivity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 95 percent.
(B) Clinical specificity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 96 percent.
(3) For any HCV antibody test intended for Point of Care (PoC) use, the following special controls, in addition to those listed in paragraphs (b)(1) and (2) of this section, apply:
(i) Clinical studies must be conducted at PoC sites.
(ii) Additional labeling must include a brief summary of the instructions for use that are appropriate for use in a PoC environment.
[86 FR 66176, Nov. 22, 2021]
|
|
|
Sec. 866.3170 Nucleic acid-based hepatitis C virus ribonucleic acid tests.
|
|
(a) Identification. A nucleic acid-based hepatitis C virus (HCV) ribonucleic acid (RNA) test is identified as an in vitro diagnostic device intended for prescription use as an aid in the diagnosis of HCV infection in specified populations, and/or as an aid in the management of HCV-infected patients including guiding the selection of genotype-specific treatment in individuals with chronic HCV infection. The test is intended for use with human serum or plasma. The test is not intended for use as a donor screening test for the presence of HCV antibodies in blood, blood products, or tissue donors.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) For all nucleic acid-based HCV RNA tests, the labeling required under § 809.10(b) of this chapter must include:
(i) A prominent statement that the test is not intended for use as a donor screening test for the presence of HCV RNA from human cells, tissues, and cellular and tissue-based products.
(ii) A detailed explanation of the principles of operation and procedures for performing the assay.
(iii) A detailed explanation of the interpretation of results.
(iv) Limitations, which must be updated to reflect current clinical practice and disease presentation and management. These limitations must include, but are not limited to, statements that indicate:
(A) The specimen types for which the device has been cleared and that use of this test kit with specimen types other than those specifically cleared for this device may result in inaccurate test results.
(B) When applicable, that assay performance characteristics have not been established in populations of immunocompromised or immunosuppressed patients or, other populations where test performance may be affected.
(C) Test results are to be interpreted by qualified licensed healthcare professionals in conjunction with the individual's clinical presentation, history, and other laboratory results.
(2) For all nucleic acid-based HCV RNA tests, the design verification and validation must include:
(i) Detailed device description, including the device components, ancillary reagents required but not provided, and an explanation of the device methodology. Additional information appropriate to the technology must be included such as design of primers and probes, rationale for the selected gene targets, specifications for amplicon size, and degree of nucleic acid sequence conservation.
(ii) For devices with assay calibrators, the design and nature of all primary, secondary, and subsequent quantitation standards used for calibration as well as their traceability to a standardized reference material that FDA has determined is appropriate (e.g., a recognized consensus standard). In addition, analytical testing must be performed following the release of a new lot of the standard material that was used for device clearance or approval, or when there is a transition to a new calibration standard.
(iii) Documentation and characterization (e.g., determination of the identity, supplier, purity, and stability) of all critical reagents (including nucleic acid sequences for primers and probes) and protocols for maintaining product integrity.
(iv) Detailed documentation of analytical performance studies conducted as appropriate to the technology, specimen types tested, and intended use of the device, including, but not limited to, limit of detection (LoD), upper and lower limits of quantitation (ULoQ and LLoQ, respectively), linearity, precision, endogenous and exogenous interferences, cross reactivity, carryover, matrix equivalency, and sample and reagent stability. Samples selected for use in analytical studies or used to prepare samples for use in analytical studies must be from subjects with clinically relevant circulating genotypes in the United States. Cross-reactivity studies must include samples from HCV RNA negative subjects with other causes of liver disease, including autoimmune hepatitis, alcoholic liver disease, chronic hepatitis B virus, primary biliary cirrhosis, and nonalcoholic steatohepatitis, when applicable. The effect of each claimed nucleic-acid isolation and purification procedure on detection must be evaluated.
(v) Risk analysis and management strategies, such as Failure Modes Effects Analysis and/or Hazard Analysis and Critical Control Points summaries and their impact on test performance.
(vi) Final release criteria to be used for manufactured test lots with appropriate evidence that lots released at the extremes of the specifications will meet the claimed analytical and clinical performance characteristics as well as the stability claims.
(vii) Multisite reproducibility study that includes the testing of three independent production lots.
(viii) All stability protocols, including acceptance criteria.
(ix) Final release test results for each lot used in clinical studies.
(x) Analytical sensitivity and specificity of the test must be the same or better than that of other cleared or approved tests.
(xi) Lot-to-lot precision studies, as appropriate.
(3) For devices intended for the qualitative detection of HCV RNA, in addition to the special controls listed in paragraphs (b)(1) and (2) of this section, the design verification and validation must include detailed documentation of performance from a multisite clinical study. Performance must be analyzed relative to an FDA cleared or approved qualitative HCV RNA test, or a comparator that FDA has determined is appropriate. This study must be conducted using appropriate patient samples, with appropriate numbers of HCV positive and negative samples in applicable risk categories. Additional genotypes must be validated using appropriate numbers and types of samples. The samples may be a combination of fresh and repository samples, sourced from within and outside the United States, as appropriate. The study designs, including number of samples tested, must be sufficient to meet the following criteria:
(i) Clinical sensitivity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 95 percent.
(ii) Clinical specificity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 96 percent.
(4) For devices intended for the quantitative detection of HCV RNA, the following special controls, in addition to those listed in paragraphs (b)(1) and (2) of this section, apply:
(i) Labeling required under § 809.10(b) of this chapter must include a prominent statement that the test is not intended as a diagnostic test to confirm the presence of active HCV infection, when applicable.
(ii) Design verification and validation must include the following:
(A) Detailed documentation of the following analytical performance studies conducted as appropriate to the technology, specimen types tested, and intended use of the device, including but not limited to: LoD, ULoQ and LLoQ. LoD, LLoQ, and linearity studies must demonstrate acceptable device performance with all HCV genotypes detected by the device.
(B) Detailed documentation of clinical performance testing from either:
(1 ) A multisite clinical study with an appropriate number of clinical samples from chronically HCV infected patients in which the results are compared to an FDA-cleared or approved quantitative HCV RNA test, or a comparator that FDA has determined is appropriate. This study must include a sufficient number of HCV positive samples containing an analyte concentration near the LLoQ to describe performance at this level. Clinical samples must cover the full range of the device output and must be consistent with the distribution of these genotypes in the U.S. population. Clinical samples may be supplemented with diluted clinical samples for those viral load concentrations that are not sufficiently covered by natural clinical specimens, or
(2 ) A clinical study with prospectively collected samples demonstrating clinical validity of the device.
(C) Detailed documentation of a qualitative analysis near the lower end of the measuring range demonstrating acceptable performance when used as an aid in diagnosis.
(5) For devices intended for HCV RNA genotyping, in addition to the special controls listed in paragraphs (b)(1) and (2) of this section, design verification and validation must include the following:
(i) Detailed documentation of an analytical performance study demonstrating the LoD for all HCV genotypes detected by the device.
(ii) Detailed documentation, including results, of a multisite clinical study that assesses genotyping accuracy (i.e., the proportion of interpretable results that match with the reference method result) and the genotyping rate (i.e., the proportion of results that were interpretable).
(6) For any nucleic acid-based HCV RNA test intended for Point of Care (PoC) use, the following special controls, in addition to those listed in paragraphs (b)(1) and (2) of this section, apply:
(i) Clinical studies must be conducted at PoC sites.
(ii) Additional labeling must include a brief summary of the instructions for use that are appropriate for use in a PoC environment.
[86 FR 66172, Nov. 22, 2021]
|
|
|
Sec. 866.3175 Cytomegalovirus serological reagents.
|
|
(a) Identification. Cytomegalovirus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to cytomegalovirus in serum. The identification aids in the diagnosis of diseases caused by cytomegaloviruses (principally cytomegalic inclusion disease) and provides epidemiological information on these diseases. Cytomegalic inclusion disease is a generalized infection of infants and is caused by intrauterine or early postnatal infection with the virus. The disease may cause severe congenital abnormalities, such as microcephaly (abnormal smallness of the head), motor disability, and mental retardation. Cytomegalovirus infection has also been associated with acquired hemolytic anemia, acute and chronic hepatitis, and an infectious mononucleosis-like syndrome.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.3200 Echinococcus spp. serological reagents.
|
|
(a) Identification. Echinococcus spp. serological reagents are devices that consist of Echinococcus spp. antigens and antisera used in serological tests to identify antibodies to Echinococcus spp. in serum. The identification aids in the diagnosis of echinococcosis, caused by parasitic tapeworms belonging to the genus Echinococcus and provides epidemiological information on this disease. Echinococcosis is characterized by the development of cysts in the liver, lung, kidneys, and other organs formed by the larva of the infecting organisms.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3205 Echovirus serological reagents.
|
|
(a) Identification. Echovirus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to echovirus in serum. Additionally, some of these reagents consist of echovirus antisera conjugated with a fluorescent dye used to identify echoviruses from clinical specimens or from tissue culture isolates derived from clinical specimens. The identification aids in the diagnosis of echovirus infections and provides epidemiological information on diseases caused by these viruses. Echoviruses cause illnesses such as meningitis (inflammation of the brain and spinal cord membranes), febrile illnesses (accompanied by fever) with or without rash, and the common cold.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3210 Endotoxin assay.
|
|
(a) Identification. An endotoxin assay is a device that uses serological techniques in whole blood. The device is intended for use in conjunction with other laboratory findings and clinical assessment of the patient to aid in the risk assessment of critically ill patients for progression to severe sepsis.
(b) Classification. Class II (special controls). The special control for this device is the FDA guidance entitled "Class II Special Controls Guidance Document: Endotoxin Assay." See § 866.1(e) for the availability of this guidance document.
[68 FR 62008, Oct. 31, 2003. Redesignated at 70 FR 53069, Sept. 7, 2005]
|
|
|
Sec. 866.3215 Device to detect and measure non-microbial analyte(s) in human clinical specimens to aid in assessment of patients with suspected sepsis.
|
|
(a) Identification. A device to detect and measure non-microbial analyte(s) in human clinical specimens to aid in assessment of patients with suspected sepsis is identified as an in vitro device intended for the detection and qualitative and/or quantitative measurement of one or more non-microbial analytes in human clinical specimens to aid in the assessment of patients with suspected sepsis when used in conjunction with clinical signs and symptoms and other clinical and laboratory findings.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include the device's detailed Indications for Use statement describing what the device detects and measures, the results provided to the user, whether the measure is qualitative and/or quantitative, the clinical indications for which the test is to be used, and the specific population(s) for which the device use is intended.
(2) Premarket notification submissions must include detailed documentation of the device description, including (as applicable), all device components, software, ancillary reagents required but not provided, explanation of the device principle and methodology, and for molecular devices include detailed documentation of the primer/probe sequence, design, and rationale for sequence selection.
(3) Premarket notification submissions must include detailed documentation of applicable analytical studies, such as, analytical sensitivity (Limit of Detection, Limit of Blank, and Limit of Quantitation), precision, reproducibility, analytical measuring range, interference, cross-reactivity, and specimen stability.
(4) Premarket notification submissions must include detailed documentation of a prospective clinical study or, if appropriate, results from an equivalent sample set. This detailed documentation must include the following information:
(i) Results must demonstrate adequate device performance relative to a well-accepted comparator.
(ii) Clinical sample results must demonstrate consistency of device output throughout the device measuring range likely to be encountered in the Intended Use population.
(iii) Clinical study documentation must include the original study protocol (including predefined statistical analysis plan), study report documenting support for the Indications for Use(s), and results of all statistical analyses.
(5) Premarket notification submissions must include evaluation of the level of the non-microbial analyte in asymptomatic patients with demographic characteristics (e.g., age, racial, ethnic, and gender distribution) similar to the Intended Use population.
(6) As part of the risk management activities performed under 21 CFR 820.30 design controls, you must document an appropriate end user device training program that will be offered as part of your efforts to mitigate the risk of failure to correctly operate the instrument.
(7) A detailed explanation of the interpretation of results and acceptance criteria must be included in the device's 21 CFR 809.10(b)(9) compliant labeling, and a detailed explanation of the interpretation of the limitations of the samples (e.g., collected on day of diagnosis) must be included in the device's 21 CFR 809.10(b)(10) compliant labeling.
[82 FR 49099, Oct. 24, 2017]
|
|
|
Sec. 866.3220 Entamoeba histolytica serological reagents.
|
|
(a) Identification. Entamoeba histolytica serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Entamoeba histolytica in serum. Additionally, some of these reagents consist of antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Entamoeba histolytica directly from clinical specimens. The identification aids in the diagnosis of amebiasis caused by the microscopic protozoan parasite Entamoeba histolytica and provides epidemiological information on diseases caused by this parasite. The parasite may invade the skin, liver, intestines, lungs, and diaphragm, causing disease conditions such as indolent ulcers, an amebic hepatitis, amebic dysentery, and pulmonary lesions.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982; 47 FR 56846, Dec. 21, 1982, as amended at 63 FR 59226, Nov. 3, 1998]
|
|
|
Sec. 866.3225 Enterovirus nucleic acid assay.
|
|
(a) Identification. An enterovirus nucleic acid assay is a device that consists of primers, probes, enzymes, and controls for the amplification and detection of enterovirus ribonucleic acid (RNA) in cerebrospinal fluid (CSF) from individuals who have signs and symptoms consistent with meningitis or meningoencephalitis. The detection of enterovirus RNA, in conjunction with other laboratory tests, aids in the clinical laboratory diagnosis of viral meningitis caused by enterovirus.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: Nucleic Acid Amplification Assay for the Detection of Enterovirus RNA." See § 866.1(e) for the availability of this guidance document.
[74 FR 8, Jan. 2, 2009]
|
|
|
Sec. 866.3235 Epstein-Barr virus serological reagents.
|
|
(a) Identification. Epstein-Barr virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Epstein-Barr virus in serum. The identification aids in the diagnosis of Epstein-Barr virus infections and provides epidemiological information on diseases caused by these viruses. Epstein-Barr viruses are thought to cause infectious mononucleosis and have been associated with Burkitt's lymphoma (a tumor of the jaw in African children and young adults) and postnasal carcinoma (cancer).
(b) Classification. Class I (general controls).
|
|
|
Sec. 866.3240 Equine encephalomyelitis virus serological reagents.
|
|
(a) Identification. Equine encephalomyelitis virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antobodies to equine encephalomyelitis virus in serum. The identification aids in the diagnosis of diseases caused by equine encephalomyelitis viruses and provides epidemiological information on these viruses. Equine encephalomyelitis viruses are transmitted to humans by the bite of insects, such as mosquitos and ticks, and may cause encephalitis (inflammation of the brain), rash, acute arthritis, or hepatitis.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3250 Erysipelothrix rhusiopathiae serological reagents.
|
|
(a) Identification. Erysipelothrix rhusiopathiae serological reagents are devices that consist of antigens and antisera used in serological tests to identify Erysipelothrix rhusiopathiae from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of disease caused by this bacterium belonging to the genus Erysipelothrix. This organism is responsible for a variety of inflammations of the skin following skin abrasions from contact with fish, shellfish, or poultry.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3255 Escherichia coli serological reagents.
|
|
(a) Identification. Escherichia coli serological reagents are devices that consist of antigens and antisera used in serological tests to identify Escherichia coli from cultured isolates derived from clinical specimens. Additionally, some of these reagents consist of Escherichia coli antisera conjugated with a fluorescent dye used to identify Escherichia coli directly from clinical specimens or cultured isolates derived from clinical specimens. The identification aids in the diagnosis of diseases caused by this bacterium belonging to the genus Escherichia, and provides epidemiological information on diseases caused by this microorganism. Although Escherichia coli constitutes the greater part of the microorganisms found in the intestinal tract in humans and is usually nonpathogenic, those strains which are pathogenic may cause urinary tract infections or epidemic diarrheal disease, especially in children.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38791, July 25, 2001]
|
|
|
Sec. 866.3270 Flavobacterium spp. serological reagents.
|
|
(a) Identification. Flavobacterium spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify Flavobacteriuim spp. from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Flavobacterium and provides epidemiological information on diseases caused by these microorganisms. Most members of this genus are found in soil and water and, under certain conditions, may become pathogenic to humans. Flavobacterium meningosepticum is highly virulent for the newborn, in whom it may cause epidemics of septicemia (blood poisoning) and meningitis (inflammation of the membranes of the brain) and is usually attributable to contaminated hospital equipment.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25046, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3280 Francisella tularensis serological reagents.
|
|
(a) Identification. Francisella tularensis serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Francisella tularensis in serum or to identify Francisella tularensis in cultured isolates derived from clinical specimens. Additionally, some of these reagents consist of antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Francisella tularensis directly from clinical specimens. The identification aids in the diagnosis of tularemia caused by Francisella tularensis and provides epidemiological information on this disease. Tularemia is a desease principally of rodents, but may be transmitted to humans through handling of infected animals, animal products, or by the bites of fleas and ticks. The disease takes on several forms depending upon the site of infection, such as skin lesions, lymph node enlargements, or pulmonary infection.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59226, Nov. 3, 1998]
|
|
|
Sec. 866.3290 Gonococcal antibody test (GAT).
|
|
(a) Identification. A gonococcal antibody test (GAT) is an in vitro device that consists of the reagents intended to identify by immunochemical techniques, such as latex agglutination, indirect fluorescent antibody, or radioimmunoassay, antibodies to Neisseria gonorrhoeae in sera of asymptomatic females at low risk of infection. Identification of antibodies with this device may indicate past or present infection of the patient with Neisseria gonorrhoeae.
(b) Classification. Class III (premarket approval) (transitional device).
(c) Date PMA or notice of completion of a PDP is required. As of May 28, 1976, an approval under section 515 of the act is required before this device may be commercially distributed. See § 866.3.
[47 FR 50823, Nov. 9, 1982, as amended at 52 FR 17734, May 11, 1987]
|
|
|
Sec. 866.3300 Haemophilus spp. serological reagents.
|
|
(a) Identification. Haemophilus spp. serological reagents are devices that consist of antigens and antisera, including antisera conjugated with a fluorescent dye, that are used in serological tests to identify Haemophilus spp. directly from clinical specimens or tissue culture isolates derived from clinical specimens. The identification aids in the diagnosis of diseases caused by bacteria belonging to the genus Haemophilus and provides epidemiological information on diseases cause by these microorganisms. Diseases most often caused by Haemophilus spp. include pneumonia, pharyngitis, sinusitis, vaginitis, chancroid venereal disease, and a contagious form of conjunctivitis (inflammation of eyelid membranes).
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59226, Nov. 3, 1998]
|
|
|
Sec. 866.3305 Herpes simplex virus serological assays.
|
|
(a) Identification. Herpes simplex virus serological assays are devices that consist of antigens and antisera used in various serological tests to identify antibodies to herpes simplex virus in serum. Additionally, some of the assays consist of herpes simplex virus antisera conjugated with a fluorescent dye (immunofluorescent assays) used to identify herpes simplex virus directly from clinical specimens or tissue culture isolates derived from clinical specimens. The identification aids in the diagnosis of diseases caused by herpes simplex viruses and provides epidemiological information on these diseases. Herpes simplex viral infections range from common and mild lesions of the skin and mucous membranes to a severe form of encephalitis (inflammation of the brain). Neonatal herpes virus infections range from a mild infection to a severe generalized disease with a fatal outcome.
(b) Classification. Class II (special controls). The device is classified as class II (special controls). The special control for the device is FDA's revised guidance document entitled "Class II Special Controls Guidance Document: Herpes Simplex Virus Types 1 and 2 Serological Assays." For availability of the guidance revised document, see § 866.1(e).
[72 FR 15830, Apr. 3, 2007, as amended at 74 FR 42775, Aug. 25, 2009; 76 FR 48717, Aug. 9, 2011]
|
|
|
Sec. 866.3309 Herpes virus nucleic acid-based cutaneous and mucocutaneous lesion panel.
|
|
(a) Identification. A herpes virus nucleic acid-based cutaneous and mucocutaneous lesion panel is a qualitative in vitro diagnostic device intended for the simultaneous detection and differentiation of different herpes viruses in cutaneous and mucocutaneous lesion samples from symptomatic patients suspected of Herpetic infections. Negative results do not preclude infection and should not be used as the sole basis for treatment or other patient management decisions. The assay is not intended for use in cerebrospinal fluid samples.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include detailed documentation for the device description, including the device components, ancillary reagents required but not provided, and a detailed explanation of the methodology including primer design and selection.
(2) Premarket notification submissions must include detailed documentation from the following analytical and clinical performance studies: Analytical sensitivity (Limit of Detection), reactivity, inclusivity, precision, reproducibility, interference, cross reactivity, carry-over, and cross contamination.
(3) Premarket notification submissions must include detailed documentation of a clinical study using lesion samples in which Herpes Simplex Virus 1, Herpes Simplex Virus 2, or Varicella Zoster Virus DNA detection was requested. The study must compare the device performance to an appropriate well established reference method.
(4) A detailed explanation of the interpretation of results and acceptance criteria must be included in the device's 21 CFR 809.10(b)(9) compliant labeling.
(5) The device labeling must include a limitation statement that reads: "The device is not intended for use with cerebrospinal fluid or to aid in the diagnosis of HSV or VZV infections of the central nervous system (CNS)."
(6) Premarket notification submissions must include quality assurance protocols and a detailed documentation for device software, including, but not limited to, standalone software applications and hardware-based devices that incorporate software.
(7) The risk management activities performed as part of the manufacturer's 21 CFR 820.30 design controls must document an appropriate end user device training program that will be offered as part of efforts to mitigate the risk of failure to correctly operate the instrument.
[83 FR 52314, Oct. 17, 2018]
|
|
|
Sec. 866.3310 Hepatitis A virus (HAV) serological assays.
|
|
(a) Identification. HAV serological assays are devices that consist of antigens and antisera for the detection of hepatitis A virus-specific IgM, IgG, or total antibodies (IgM and IgG), in human serum or plasma. These devices are used for testing specimens from individuals who have signs and symptoms consistent with acute hepatitis to determine if an individual has been previously infected with HAV, or as an aid to identify HAV-susceptible individuals. The detection of these antibodies aids in the clinical laboratory diagnosis of an acute or past infection by HAV in conjunction with other clinical laboratory findings. These devices are not intended for screening blood or solid or soft tissue donors.
(b) Classification. Class II (special controls). The special control is "Guidance for Industry and FDA Staff: Class II Special Controls Guidance Document: Hepatitis A Virus Serological Assays." See § 866.1(e) for the availability of this guidance document.
[71 FR 6679, Feb. 9, 2006]
|
|
|
Sec. 866.3320 Histoplasma capsulatum serological reagents.
|
|
(a) Identification. Histoplasma capsulatum serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Histoplasma capsulatum in serum. Additionally, some of these reagents consist of Histoplasma capsulatum antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Histoplasma capsulatum from clinical specimens or cultured isolates derived from clinical specimens. The identification aids in the diagnosis of histoplasmosis caused by this fungus belonging to the genus Histoplasma and provides epidemiological information on the diseases caused by this fungus. Histoplasmosis usually is a mild and often asymptomatic respiratory infection, but in a small number of infected individuals the lesions may spread to practically all tissues and organs.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.3328 Influenza virus antigen detection test system.
|
|
(a) Identification. An influenza virus antigen detection test system is a device intended for the qualitative detection of influenza viral antigens directly from clinical specimens in patients with signs and symptoms of respiratory infection. The test aids in the diagnosis of influenza infection and provides epidemiological information on influenza. Due to the propensity of the virus to mutate, new strains emerge over time which may potentially affect the performance of these devices. Because influenza is highly contagious and may lead to an acute respiratory tract infection causing severe illness and even death, the accuracy of these devices has serious public health implications.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The device's sensitivity and specificity performance characteristics or positive percent agreement and negative percent agreement, for each specimen type claimed in the intended use of the device, must meet one of the following two minimum clinical performance criteria:
(i) For devices evaluated as compared to an FDA-cleared nucleic acid based-test or other currently appropriate and FDA accepted comparator method other than correctly performed viral culture method:
(A) The positive percent agreement estimate for the device when testing for influenza A and influenza B must be at the point estimate of at least 80 percent with a lower bound of the 95 percent confidence interval that is greater than or equal to 70 percent.
(B) The negative percent agreement estimate for the device when testing for influenza A and influenza B must be at the point estimate of at least 95 percent with a lower bound of the 95 percent confidence interval that is greater than or equal to 90 percent.
(ii) For devices evaluated as compared to correctly performed viral culture method as the comparator method:
(A) The sensitivity estimate for the device when testing for influenza A must be at the point estimate of at least 90 percent with a lower bound of the 95 percent confidence interval that is greater than or equal to 80 percent. The sensitivity estimate for the device when testing for influenza B must be at the point estimate of at least 80 percent with a lower bound of the 95 percent confidence interval that is greater than or equal to 70 percent.
(B) The specificity estimate for the device when testing for influenza A and influenza B must be at the point estimate of at least 95 percent with a lower bound of the 95 percent confidence interval that is greater than or equal to 90 percent.
(2) When performing testing to demonstrate the device meets the requirements in paragraph (b)(1) of this section, a currently appropriate and FDA accepted comparator method must be used to establish assay performance in clinical studies.
(3) Annual analytical reactivity testing of the device must be performed with contemporary influenza strains. This annual analytical reactivity testing must meet the following criteria:
(i) The appropriate strains to be tested will be identified by FDA in consultation with the Centers for Disease Control and Prevention (CDC) and sourced from CDC or an FDA-designated source. If the annual strains are not available from CDC, FDA will identify an alternative source for obtaining the requisite strains.
(ii) The testing must be conducted according to a standardized protocol considered and determined by FDA to be acceptable and appropriate.
(iii) By July 31 of each calendar year, the results of the last 3 years of annual analytical reactivity testing must be included as part of the device's labeling. If a device has not been on the market long enough for 3 years of annual analytical reactivity testing to have been conducted since the device received marketing authorization from FDA, then the results of every annual analytical reactivity testing since the device received marketing authorization from FDA must be included. The results must be presented as part of the device's labeling in a tabular format, which includes the detailed information for each virus tested as described in the certificate of authentication, either by:
(A) Placing the results directly in the device's § 809.10(b) of this chapter compliant labeling that physically accompanies the device in a separate section of the labeling where the analytical reactivity testing data can be found; or
(B) In the device's label or in other labeling that physically accompanies the device, prominently providing a hyperlink to the manufacturer's public Web site where the analytical reactivity testing data can be found. The manufacturer's home page, as well as the primary part of the manufacturer's Web site that discusses the device, must provide a prominently placed hyperlink to the Web page containing this information and must allow unrestricted viewing access.
(4) If one of the actions listed at section 564(b)(1)(A)-(D) of the Federal Food, Drug, and Cosmetic Act occurs with respect to an influenza viral strain, or if the Secretary of Health and Human Services (HHS) determines, under section 319(a) of the Public Health Service Act, that a disease or disorder presents a public health emergency, or that a public health emergency otherwise exists, with respect to an influenza viral strain:
(i) Within 30 days from the date that FDA notifies manufacturers that characterized viral samples are available for test evaluation, the manufacturer must have testing performed on the device with those viral samples in accordance with a standardized protocol considered and determined by FDA to be acceptable and appropriate. The procedure and location of testing may depend on the nature of the emerging virus.
(ii) Within 60 days from the date that FDA notifies manufacturers that characterized viral samples are available for test evaluation and continuing until 3 years from that date, the results of the influenza emergency analytical reactivity testing, including the detailed information for the virus tested as described in the certificate of authentication, must be included as part of the device's labeling in a tabular format, either by:
(A) Placing the results directly in the device's § 809.10(b) of this chapter compliant labeling that physically accompanies the device in a separate section of the labeling where analytical reactivity testing data can be found, but separate from the annual analytical reactivity testing results; or
(B) In a section of the device's label or in other labeling that physically accompanies the device, prominently providing a hyperlink to the manufacturer's public Web site where the analytical reactivity testing data can be found. The manufacturer's home page, as well as the primary part of the manufacturer's Web site that discusses the device, must provide a prominently placed hyperlink to the Web page containing this information and must allow unrestricted viewing access.
[82 FR 3618, Jan. 12, 2017]
|
|
|
Sec. 866.3330 Influenza virus serological reagents.
|
|
(a) Identification. Influenza virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to influenza in serum. The identification aids in the diagnosis of influenza (flu) and provides epidemiological information on influenza. Influenza is an acute respiratory tract disease, which is often epidemic.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3332 Reagents for detection of specific novel influenza A viruses.
|
|
(a) Identification. Reagents for detection of specific novel influenza A viruses are devices that are intended for use in a nucleic acid amplification test to directly detect specific virus RNA in human respiratory specimens or viral cultures. Detection of specific virus RNA aids in the diagnosis of influenza caused by specific novel influenza A viruses in patients with clinical risk of infection with these viruses, and also aids in the presumptive laboratory identification of specific novel influenza A viruses to provide epidemiological information on influenza. These reagents include primers, probes, and specific influenza A virus controls.
(b) Classification. Class II (special controls). The special controls are:
(1) FDA's guidance document entitled "Class II Special Controls Guidance Document: Reagents for Detection of Specific Novel Influenza A Viruses." See § 866.1(e) for information on obtaining this document.
(2) The distribution of these devices is limited to laboratories with experienced personnel who have training in standardized molecular testing procedures and expertise in viral diagnosis, and appropriate biosafety equipment and containment.
[71 FR 14379, Mar. 22, 2006]
|
|
|
Sec. 866.3336 John Cunningham Virus serological reagents.
|
|
(a) Identification. John Cunningham Virus serological reagents are devices that consist of antigens and antisera used in serological assays to identify antibodies to John Cunningham Virus in serum and plasma. The identification aids in the risk stratification for the development of progressive multifocal leukoencephalopathy in multiple sclerosis and Crohn's disease patients undergoing natalizumab therapy. These devices are for adjunctive use, in the context of other clinical risk factors for the development of progressive multifocal leukoencephalopathy.
(b) Classification. Class II (special controls). The special control for this device is the FDA guideline document entitled "Class II Special Controls Guideline: John Cunningham Virus Serological Reagents." For availability of the guideline document, see § 866.1(e).
[79 FR 3740, Jan. 23, 2014]
|
|
|
Sec. 866.3340 Klebsiella spp. serological reagents.
|
|
(a) Identification. Klebsiella spp. serological reagents are devices that consist of antigens and antisera, including antisera conjugated with a fluorescent dye (immunofluorescent reagents), that are used in serological tests to identify Klebsiella spp. from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of diseases caused by bacteria belonging to the genus Klebsiella and provides epidemiological information on these diseases. These organisms can cause serious urinary tract and pulmonary infections, particularly in hospitalized patients.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3350 Leptospira spp. serological reagents.
|
|
(a) Identification. Leptospira spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Leptospira spp. in serum or identify Leptospira spp. from cultured isolates derived from clinical specimens. Additionally, some of these antisera are conjugated with a fluorescent dye (immunofluorescent reagents) and used to identify Leptospira spp. directly from clinical specimens. The identification aids in the diagnosis of leptospirosis caused by bacteria belonging to the genus Leptospira and provides epidemiological information on this disease. Leptospira infections range from mild fever-producing illnesses to severe liver and kidney involvement producing hemorrhage and dysfunction of these organs.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.3355 Listeria spp. serological reagents.
|
|
(a) Identification. Listeria spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify Listeria spp. from cultured isolates derived from clinical specimens. Additionally, some of these reagents consist of Listeria spp. antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Listeria spp. directly from clinical specimens. The identification aids in the diagnosis of listeriosis, a disease caused by bacteria belonging to the genus Listeria, and provides epidemiological information on diseases caused by these microorganisms. Listeria monocytogenes, the most common human pathogen of this genus, causes meningitis (inflammation of the brain membranes) and meningoencephalitis (inflammation of the brain and brain membranes) and is often fatal if untreated. A second form of human listeriosis is an intrauterine infection in pregnant women that results in a high mortality rate for infants before or after birth.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3360 Lymphocytic choriomeningitis virus serological reagents.
|
|
(a) Identification. Lymphocytic choriomeningitis virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to lymphocytic choriomeningitis virus in serum. The identification aids in the diagnosis of lymphocytic choriomeningitis virus infections and provides epidemiological information on diseases caused by these viruses. Lymphocytic choriomeningitis viruses usually cause a mild cerebral meningitis (inflammation of membranes that envelop the brain) and occasionally a mild pneumonia, but in rare instances may produce severe and even fatal illnesses due to complications from cerebral meningitis and pneumonia.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3361 Mass spectrometer system for clinical use for the identification of microorganisms.
|
|
(a) Identification. A mass spectrometer system for clinical use for the identification of microorganisms is a qualitative in vitro diagnostic device intended for the identification of microorganisms cultured from human specimens. The device is comprised of an ionization source, a mass analyzer, and a spectral database. The device is indicated for use in conjunction with other clinical and laboratory findings to aid in the diagnosis of bacterial and fungal infections.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include detailed documentation for device software, including, but not limited to, standalone software applications and hardware-based devices that incorporate software.
(2) Premarket notification submissions must include database implementation methodology, construction parameters, and quality assurance protocols.
(3) A detailed explanation of the interpretation of results and acceptance criteria must be included in the device's 21 CFR 809.10(b)(9) compliant labeling.
(4) As part of the risk management activities performed as part of your 21 CFR 820.30 design controls, you must document an appropriate end user device training program that will be offered as part of your efforts to mitigate the risk of failure to correctly operate the instrument.
(5) Premarket notification submissions must include details on the appropriate end user device training program that will be offered while marketing the device.
[82 FR 49101, Oct. 24, 2017]
|
|
|
Sec. 866.3365 Multiplex nucleic acid assay for identification of microorganisms and resistance markers from positive blood cultures.
|
|
(a) Identification. A multiplex nucleic acid assay for identification of microorganisms and resistance markers from positive blood cultures is a qualitative in vitro device intended to simultaneously detect and identify microorganism nucleic acids from blood cultures that test positive by Gram stain or other microbiological stains. The device detects specific nucleic acid sequences for microorganism identification as well as for antimicrobial resistance. This device aids in the diagnosis of bloodstream infections when used in conjunction with other clinical and laboratory findings. However, the device does not replace traditional methods for culture and susceptibility testing.
(b) Classification. Class II (special controls). The special control for this device is FDA's guideline document entitled "Class II Special Controls Guideline: Multiplex Nucleic Acid Assay for Identification of Microorganisms and Resistance Markers from Positive Blood Cultures." For availability of the guideline document, see § 866.1(e).
[80 FR 30154, May 27, 2015]
|
|
|
Sec. 866.3370 Mycobacterium tuberculosis immunofluorescent reagents.
|
|
(a) Identification. Mycobacterium tuberculosis immunofluorescent reagents are devices that consist of antisera conjugated with a fluorescent dye used to identify Mycobacterium tuberculosis directly from clinical specimens. The identification aids in the diagnosis of tuberculosis and provides epidemiological information on this disease. Mycobacterium tuberculosis is the common causative organism in human tuberculosis, a chronic infectious disease characterized by formation of tubercles (small rounded nodules) and tissue necrosis (destruction), usually occurring in the lung.
(b) Classification. Class I (general controls).
|
|
|
Sec. 866.3372 Nucleic acid-based in vitro diagnostic devices for the detection of Mycobacterium tuberculosis complex in respiratory specimens.
|
|
(a) Identification. Nucleic acid-based in vitro diagnostic devices for the detection of Mycobacterium tuberculosis complex in respiratory specimens are qualitative nucleic acid-based in vitro diagnostic devices intended to detect Mycobacterium tuberculosis complex nucleic acids extracted from human respiratory specimens. These devices are non-multiplexed and intended to be used as an aid in the diagnosis of pulmonary tuberculosis when used in conjunction with clinical and other laboratory findings. These devices do not include devices intended to detect the presence of organism mutations associated with drug resistance. Respiratory specimens may include sputum (induced or expectorated), bronchial specimens (e.g., bronchoalveolar lavage or bronchial aspirate), or tracheal aspirates.
(b) Classification. Class II (special controls). The special control for this device is the FDA document entitled "Class II Special Controls Guideline: Nucleic Acid-Based In Vitro Diagnostic Devices for the Detection of Mycobacterium tuberculosis Complex in Respiratory Specimens." For availability of the guideline document, see § 866.1(e).
[79 FR 31027, May 30, 2014]
|
|
|
Sec. 866.3373 Nucleic acid-based in vitro diagnostic devices for the detection of Mycobacterium tuberculosis complex (MTB-complex) and the genetic mutations associated with MTB-complex antibiotic resistance in respiratory specimens.
|
|
(a) Identification. Nucleic acid-based in vitro diagnostic devices for the detection of Mycobacterium tuberculosis complex (MTB-complex) and the genetic mutations associated with MTB-complex antibiotic resistance in respiratory specimens are qualitative nucleic acid-based devices that detect the presence of MTB-complex-associated nucleic acid sequences in respiratory samples. These devices are intended to aid in the diagnosis of pulmonary tuberculosis and the selection of an initial treatment regimen when used in conjunction with clinical findings and other laboratory results. These devices do not provide confirmation of antibiotic susceptibility since other mechanisms of resistance may exist that may be associated with a lack of clinical response to treatment other than those detected by the device.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The FDA document entitled "Class II Special Controls Guideline: Nucleic Acid-Based In Vitro Diagnostic Devices for the Detection of Mycobacterium tuberculosis Complex and Genetic Mutations Associated with Antibiotic Resistance in Respiratory Specimens," which addresses the mitigation of risks specific to the detection of MTB-complex. For availability of the document, see § 866.1(e).
(2) The following items, which address the mitigation of risks specific to the detection of the genetic mutations associated with antibiotic resistance of MTB-complex:
(i) The device must include an external positive assay control as appropriate. Acceptable positive assay controls include MTB-complex isolates containing one or more antibiotic-resistance associated target sequences detected by the device.
(ii) The device must include internal controls as appropriate. An acceptable internal control may include human nucleic acid co-extracted with MTB-complex containing nucleic acid sequences associated with antibiotic resistance and primers amplifying human housekeeping genes (e.g., RNaseP, [beta]-actin).
(iii) The device's intended use must include a description of the scope of antibiotic resistance targeted by the assay, i.e., the specific drugs and/or drug classes.
(iv) The specific performance characteristics section of the device's labeling must include information regarding the specificity of the assay oligonucleotides for detecting mutations associated with antibiotic resistance of MTB-complex, and any information indicating the potential for non-specific binding (e.g., BLAST search).
(v) In demonstrating device performance you must perform:
(A) Pre-analytical studies that evaluate:
(1 ) Frozen samples. If there is use of any frozen samples in the device performance studies, or if there is a device claim for the use of frozen samples for testing, the effect of freezing samples prior to testing and the effect of multiple freeze/thaw cycles on both antibiotic susceptible and antibiotic resistant strains of MTB-complex.
(2 ) Nucleic acid extraction methods. Extraction methods must parallel those used in devices for the detection of MTB-complex nucleic acid and confirm that the detection of the genetic mutations associated with antibiotic resistance is not affected.
(B) Analytical studies that analyze:
(1 ) Limit of Detection. Limit of Detection must be determined in the most challenging matrix (e.g., sputum) claimed for use with the device. The Limit of Detection must be determined using both antibiotic susceptible and antibiotic resistant strains of MTB-complex. The antibiotic resistant strains must be those with well characterized genetic mutations associated with antibiotic resistance.
(2 ) Analytical Reactivity (Inclusivity). Testing must be conducted to evaluate the ability of the device to detect genetic mutations associated with antibiotic resistance in a diversity of MTB-complex strains. Isolates used in testing must be well characterized. Isolate strain characterization must be determined using standardized reference methods recognized by a reputable scientific body and appropriate to the strain lineage.
(3 ) Within-Laboratory (Repeatability) Precision Testing. Within-laboratory precision studies, if appropriate, must include at least one antibiotic resistant and one antibiotic susceptible strain of MTB-complex.
(4) Between Laboratory Reproducibility Testing. The protocol for the reproducibility study may vary slightly depending on the assay format; however, the panel must include at least one antibiotic resistant and one antibiotic susceptible strain of MTB-complex.
(C) Clinical Studies. Clinical performance of the device must be established by conducting prospective clinical studies that include subjects with culture confirmed active tuberculosis. Studies must attempt to enroll subjects at risk for antibiotic-resistant MTB-complex; however, it may be necessary to include supplemental antibiotic resistant retrospective and contrived samples. Clinical studies must compare device results to both phenotypic drug susceptibility testing and genotypic reference methods. The genotypic reference method must be a polymerase chain reaction based method that uses primers different from those in the experimental device and confirmed by bidirectional sequencing.
[79 FR 63036, Oct. 22, 2014]
|
|
|
Sec. 866.3375 Mycoplasma spp. serological reagents.
|
|
(a) Identification. Mycoplasma spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Mycoplasma spp. in serum. Additionally, some of these reagents consist of Mycoplasma spp. antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Mycoplasma spp. directly from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Mycoplasma and provides epidemiological information on diseases caused by these microorganisms. Mycoplasma spp. are associated with inflammatory conditions of the urinary and respiratory tracts, the genitals, and the mouth. The effects in humans of infection with Mycoplasma pneumoniae range from inapparent infection to mild or severe upper respiratory disease, ear infection, and bronchial pneumonia.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3380 Mumps virus serological reagents.
|
|
(a) Identification. Mumps virus serological reagents consist of antigens and antisera used in serological tests to identify antibodies to mumps virus in serum. Additionally, some of these reagents consist of antisera conjugated with a fluorescent dye (immunofluorescent reagents) used in serological tests to identify mumps viruses from tissue culture isolates derived from clinical specimens. The identification aids in the diagnosis of mumps and provides epidemiological information on mumps. Mumps is an acute contagious disease, particularly in children, characterized by an enlargement of one or both of the parotid glands (glands situated near the ear), although other organs may also be involved.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2311, Jan. 14, 2000]
|
|
|
Sec. 866.3390 Neisseria spp. direct serological test reagents.
|
|
(a) Identification. Neisseria spp. direct serological test reagents are devices that consist of antigens and antisera used in serological tests to identify Neisseria spp. from cultured isolates. Additionally, some of these reagents consist of Neisseria spp. antisera conjugated with a fluorescent dye (immunofluorescent reagents) which may be used to detect the presence of Neisseria spp. directly from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Neisseria, such as epidemic cerebrospinal meningitis, meningococcal disease, and gonorrhea, and also provides epidemiological information on diseases caused by these microorganisms. The device does not include products for the detection of gonorrhea in humans by indirect methods, such as detection of antibodies or of oxidase produced by gonococcal organisms.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.3395 Norovirus serological reagents.
|
|
(a) Identification. Norovirus serological reagents are devices that consist of antigens and antisera used in serological tests to detect the presence of norovirus antigens in fecal samples. These devices aid in the diagnosis of norovirus infection in the setting of an individual patient with symptoms of acute gastroenteritis when the individual patient is epidemiologically linked to other patients with symptoms of acute gastroenteritis and/or aid in the identification of norovirus as the etiology of an outbreak of acute gastroenteritis in the setting of epidemiologically linked patients with symptoms of acute gastroenteritis.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9. The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: Norovirus Serological Reagents." See § 866.1(e) for the availability of this guidance document.
[76 FR 14274, Mar. 9, 2012, as amended at 84 FR 71800, Dec. 30, 2019]
|
|
|
Sec. 866.3400 Parainfluenza virus serological reagents.
|
|
(a) Identification. Parainfluenza virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to parainfluenza virus in serum. The identification aids in the diagnosis of parainfluenza virus infections and provides epidemiological information on diseases caused by these viruses. Parainfluenza viruses cause a variety of respiratory illnesses ranging from the common cold to pneumonia.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3402 Plasmodium species antigen detection assays.
|
|
(a) Identification. A Plasmodium species antigen detection assay is a device that employs antibodies for the detection of specific malaria parasite antigens, including histidine-rich protein-2 (HRP2) specific antigens, and pan malarial antigens in human whole blood. These devices are used for testing specimens from individuals who have signs and symptoms consistent with malaria infection. The detection of these antigens aids in the clinical laboratory diagnosis of malaria caused by the four malaria species capable of infecting humans: Plasmodium falciparum , Plasmodium vivax , Plasmodium ovale , and Plasmodium malariae , and aids in the differential diagnosis of Plasmodium falciparum infections from other less virulent Plasmodium species. The device is intended for use in conjunction with other clinical laboratory findings.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: Plasmodium species Antigen Detection Assays." See § 866.1(e) for the availability of this guidance document.
[73 FR 29054, May 20, 2008]
|
|
|
Sec. 866.3405 Poliovirus serological reagents.
|
|
(a) Identification. Poliovirus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to poliovirus in serum. Additionally, some of these reagents consist of poliovirus antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify polioviruses from clinical specimens or from tissue culture isolates derived from clinical specimens. The identification aids in the diagnosis of poliomyelitis (polio) and provides epidemiological information on this disease. Poliomyelitis is an acute infectious disease which in its serious form affects the central nervous system resulting in atrophy (wasting away) of groups of muscles, ending in contraction and permanent deformity.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.3410 Proteus spp. (Weil-Felix) serological reagents.
|
|
(a) Identification. Proteus spp. (Weil-Felix) serological reagents are devices that consist of antigens and antisera, including antisera conjugated with a fluorescent dye (immunofluorescent reagents), derived from the bacterium Proteus vulgaris used in agglutination tests (a specific type of antigen-antibody reaction) for the detection of antibodies to rickettsia (virus-like bacteria) in serum. Test results aid in the diagnosis of diseases caused by bacteria belonging to the genus Rickettsiae and provide epidemiological information on these diseases. Rickettsia are generally transmitted by arthropods (e.g., ticks and mosquitoes) and produce infections in humans characterized by rash and fever (e.g., typhus fever, spotted fever, Q fever, and trench fever).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3415 Pseudomonas spp. serological reagents.
|
|
(a) Identification. Pseudomonas spp. serological reagents are devices that consist of antigens and antisera, including antisera conjugated with a fluorescent dye (immunofluorescent reagents), used to identify Pseudomonas spp. from clinical specimens or from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Pseudomonas. Pseudomonas aeruginosa is a major cause of hospital-acquired infections, and has been associated with urinary tract infections, eye infections, burn and wound infections, blood poisoning, abscesses, and meningitis (inflammation of brain membranes). Pseudomonas pseudomallei causes melioidosis, a chronic pneumonia.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.3460 Rabiesvirus immunofluorescent reagents.
|
|
(a) Identification. Rabiesvirus immunofluorescent reagents are devices that consist of rabiesvirus antisera conjugated with a fluorescent dye used to identify rabiesvirus in specimens taken from suspected rabid animals. The identification aids in the diagnosis of rabies in patients exposed by animal bites and provides epidemiological information on rabies. Rabies is an acute infectious disease of the central nervous system which, if undiagnosed, may be fatal. The disease is commonly transmitted to humans by a bite from a rabid animal.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.3470 Reovirus serological reagents.
|
|
(a) Identification. Reovirus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to reovirus in serum. The identification aids in the diagnosis of reovirus infections and provides epidemiological information on diseases caused by these viruses. Reoviruses are thought to cause only mild respiratory and gastrointestinal illnesses.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3480 Respiratory syncytial virus serological reagents.
|
|
(a) Identification. Respiratory syncytial virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to respiratory syncytial virus in serum. Additionally, some of these reagents consist of respiratory syncytial virus antisera conjugated with a fluorescent dye (immunofluorescent reagents) and used to identify respiratory syncytial viruses from clinical specimens or from tissue culture isolates derived from clinical specimens. The identification aids in the diagnosis of respiratory syncytial virus infections and provides epidemiological information on diseases caused by these viruses. Respiratory syncytial viruses cause a number of respiratory tract infections, including the common cold, pharyngitis, and infantile bronchopneumonia.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.3490 Rhinovirus serological reagents.
|
|
(a) Identification. Rhinovirus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to rhinovirus in serum. The identification aids in the diagnosis of rhinovirus infections and provides epidemiological information on diseases caused by these viruses. Rhinoviruses cause common colds.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3500 Rickettsia serological reagents.
|
|
(a) Identification. Rickettsia serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to rickettsia in serum. Additionally, some of these reagents consist of rickettsial antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify rickettsia directly from clinical specimens. The identification aids in the diagnosis of diseases caused by virus-like bacteria belonging to the genus Rickettsiae and provides epidemiological information on these diseases. Rickettsia are generally transmitted by arthropods (e.g., ticks and mosquitoes) and produce infections in humans characterized by rash and fever (e.g., typhus fever, spotted fever, Q fever, and trench fever).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.3510 Rubella virus serological reagents.
|
|
(a) Identification. Rubella virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to rubella virus in serum. The identification aids in the diagnosis of rubella (German measles) or confirmation of a person's immune status from past infections or immunizations and provides epidemiological information on German measles. Newborns infected in the uterus with rubella virus may be born with multiple congenital defects (rubella syndrome).
(b) Classification. Class II. The special controls for this device are:
(1) National Committee for Clinical Laboratory Standards':
(i) 1/LA6 "Detection and Quantitation of Rubella IgG Antibody: Evaluation and Performance Criteria for Multiple Component Test Products, Speciment Handling, and Use of the Test Products in the Clinical Laboratory, October 1997,"
(ii) 1/LA18 "Specifications for Immunological Testing for Infectious Diseases, December 1994,"
(iii) D13 "Agglutination Characteristics, Methodology, Limitations, and Clinical Validation, October 1993,"
(iv) EP5 "Evaluation of Precision Performance of Clinical Chemistry Devices, February 1999," and
(v) EP10 "Preliminary Evaluation of the Linearity of Quantitive Clinical Laboratory Methods, May 1998,"
(2) Centers for Disease Control's:
(i) Low Titer Rubella Standard,
(ii) Reference Panel of Well Characterized Rubella Sera, and
(3) World Health Organization's International Rubella Standard.
[47 FR 50823, Nov. 9, 1982, as amended at 52 FR 17734, May 11, 1987; 65 FR 17144, Mar. 31, 2000]
|
|
|
Sec. 866.3520 Rubeola (measles) virus serological reagents.
|
|
(a) Identification. Rubeola (measles) virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to rubeola virus in serum. The identification aids in the diagnosis of measles and provides epidemiological information on the disease. Measles is an acute, highly infectious disease of the respiratory and reticuloendothelial tissues, particularly in children, characterized by a confluent and blotchy rash.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3550 Salmonella spp. serological reagents.
|
|
(a) Identification. Salmonella spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify Salmonella spp. from cultured isolates derived from clinical specimens. Additionally, some of these reagents consist of antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Salmonella spp. directly from clinical specimens or cultured isolates derived from clinical specimens. The identification aids in the diagnosis of salmonellosis caused by bacteria belonging to the genus Salmonella and provides epidemiological information on this disease. Salmonellosis is characterized by high grade fever ("enteric fever"), severe diarrhea, and cramps.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.3600 Schistosoma spp. serological reagents.
|
|
(a) Identification. Schistosoma spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Schistosoma spp. in serum. The identification aids in the diagnosis of schistosomiasis caused by parasitic flatworms of the genus Schistosoma. Schistosomiasis is characterized by a variety of acute and chronic infections. Acute infection is marked by fever, allergic symptoms, and diarrhea. Chronic effects are usually severe and are caused by fibrous degeneration of tissue around deposited eggs of the parasite in the liver, lungs, and central nervous system. Schistosomes can also cause schistosome dermatitis (e.g., swimmer's itch), a skin disease marked by intense itching.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.3630 Serratia spp. serological reagents.
|
|
(a) Identification. Serratia spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify Serratia spp. from cultured isolates. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Serratia and provides epidemiological information on these diseases. Serratia spp. are occasionally associated with gastroenteritis (food poisoning) and wound infections.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3660 Shigella spp. serological reagents.
|
|
(a) Identification. Shigella spp. serological reagents are devices that consist of antigens and antisera, including antisera conjugated with a fluorescent dye (immunofluorescent reagents), used in serological tests to identify Shigella spp. from cultured isolates. The identification aids in the diagnosis of shigellosis caused by bacteria belonging to the genus Shigella and provides epidemiological information on this disease. Shigellosis is characterized by abdominal pain, cramps, diarrhea, and fever.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.3680 Sporothrix schenckii serological reagents.
|
|
(a) Identification. Sporothrix schenckii serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Sporothrix schenckii in serum. The identification aids in the diagnosis of sporothrichosis caused by a fungus belonging to the genus Sporothrix and provides epidemiological information on this disease. Sporothrichosis is a chronic tumorlike infection primarily of the skin.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.3700 Staphylococcus aureus serological reagents.
|
|
(a) Identification. Staphylococcus aureus serological reagents are devices that consist of antigens and antisera used in serological tests to identify enterotoxin (toxin affecting the intestine) producing staphylococci from cultured isolates. The identification aids in the diagnosis of disease caused by this bacterium belonging to the genus Staphylococcus and provides epidemiological information on these diseases. Certain strains of Staphylococcus aureus produce an enterotoxin while growing in meat, dairy, or bakery products. After ingestion, this enterotoxin is absorbed in the gut and causes destruction of the intestinal lining (gastroenteritis).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3720 Streptococcus spp. exoenzyme reagents.
|
|
(a) Identification. Streptococcus spp. exoenzyme reagents are devices used to identify antibodies to Streptococcus spp. exoenzyme in serum. The identification aids in the diagnosis of disease caused by bacteria belonging to the genus Streptococcus and provides epidemiological information on these diseases. Pathogenic streptococci are associated with infections, such as sore throat, impetigo (an infection characterized by small pustules on the skin), urinary tract infections, rheumatic fever, and kidney disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 61 FR 1119, Jan. 16, 1996; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.3740 Streptococcus spp. serological reagents.
|
|
(a) Identification. Streptococcus spp. serological reagents are devices that consist of antigens and antisera (excluding streptococcal exoenzyme reagents made from enzymes secreted by streptococci) used in serological tests to identify Streptococcus spp. from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of diseases caused by bacteria belonging to the genus Streptococcus and provides epidemiological information on these diseases. Pathogenic streptococci are associated with infections, such as sore throat, impetigo (an infection characterized by small pustules on the skin), urinary tract infections, rheumatic fever, and kidney disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.3780 Toxoplasma gondii serological reagents.
|
|
(a) Identification. Toxoplasma gondii serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Toxoplasma gondii in serum. Additionally, some of these reagents consist of antisera conjugated with a fluorescent dye (immunofluorescent reagents) used to identify Toxoplasma gondii from clinical specimens. The identification aids in the diagnosis of toxoplasmosis caused by the parasitic protozoan Toxoplasma gondii and provides epidemiological information on this disease. Congenital toxoplasmosis is characterized by lesions of the central nervous system, which if undetected and untreated may lead to brain defects, blindness, and death of an unborn fetus. The disease is characterized in children by inflammation of the brain and spinal cord.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.3820 Treponema pallidum nontreponemal test reagents.
|
|
(a) Identification. Treponema pallidum nontreponemal test reagents are devices that consist of antigens derived from nontreponemal sources (sources not directly associated with treponemal organisms) and control sera (standardized sera with which test results are compared) used in serological tests to identify reagin, an antibody-like agent, which is produced from the reaction of treponema microorganisms with body tissues. The identification aids in the diagnosis of syphilis caused by microorganisms belonging to the genus Treponema and provides epidemiological information on syphilis.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.3830 Treponema pallidum treponemal test reagents.
|
|
(a) Identification. Treponema pallidum treponemal test reagents are devices that consist of the antigens, antisera and all control reagents (standardized reagents with which test results are compared) which are derived from treponemal sources and that are used in the fluorescent treponemal antibody absorption test (FTA-ABS), the Treponema pallidum immobilization test (T.P.I.), and other treponemal tests used to identify antibodies to Treponema pallidum directly from infecting treponemal organisms in serum. The identification aids in the diagnosis of syphilis caused by bacteria belonging to the genus Treponema and provides epidemiological information on syphilis.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.3850 Trichinella spiralis serological reagents.
|
|
(a) Identification. Trichinella spiralis serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Trichinella spiralis in serum. The identification aids in the diagnosis of trichinosis caused by parasitic roundworms belonging to the genus Trichinella and provides epidemiological information on trichinosis. Trichinosis is caused by ingestion of undercooked, infested meat, especially pork, and characterized by fever, muscle weakness, and diarrhea.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.3860 Trichomonas vaginalis nucleic acid assay.
|
|
(a) Identification. A Trichomonas vaginalis nucleic acid assay is a device that consists of primers, probes, enzymes, and controls for the amplification and detection of trichomonas nucleic acids in endocervical swabs, vaginal swabs, and female urine specimens, from women symptomatic for vaginitis, cervicitis, or urethritis and/or to aid in the diagnosis of trichomoniasis in asymptomatic women. The detection of trichomonas nucleic acids, in conjunction with other laboratory tests, aids in the clinical laboratory diagnosis of trichomoniasis caused by Trichomonas vaginalis .
(b) Classification. Class II (special controls). The special controls are set forth in FDA's guideline document entitled: "Class II Special Controls Guideline: Nucleic Acid Amplification Assays for the Detection of Trichomonas vaginalis; Guideline for Industry and Food and Drug Administration Staff." See § 866.1(e) for information on obtaining this document.
[80 FR 46192, Aug. 4, 2015]
|
|
|
Sec. 866.3870 Trypanosoma spp. serological reagents.
|
|
(a) Identification. Trypanosoma spp. serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to Trypanosoma spp. in serum. The identification aids in the diagnosis of trypanosomiasis, a disease caused by parasitic protozoans belonging to the genus Trypanosoma. Trypanosomiasis in adults is a chronic disease characterized by fever, chills, headache, and vomiting. Central nervous system involvement produces typical sleeping sickness syndrome: physical exhaustion, inability to eat, tissue wasting, and eventual death. Chagas disease, an acute form of trypanosomiasis in children, most seriously affects the central nervous system and heart muscle.
(b) Classification. Class I (general controls).
|
|
|
Sec. 866.3900 Varicella-zoster virus serological reagents.
|
|
(a) Identification. Varicella-zoster virus serological reagents are devices that consist of antigens and antisera used in serological tests to identify antibodies to varicella-zoster in serum. The identification aids in the diagnosis of diseases caused by varicella-zoster viruses and provides epidemiological information on these diseases. Varicella (chicken pox) is a mild, highly infectious disease, chiefly of children. Zoster (shingles) is the recurrent form of the disease, occurring in adults who were previously infected with varicella-zoster viruses. Zoster is the response (characterized by a rash) of the partially immune host to a reactivation of varicella viruses present in latent form in the patient's body.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.3920 Assayed quality control material for clinical microbiology assays.
|
|
(a) Identification. An assayed quality control material for clinical microbiology assays is a device indicated for use in a test system to estimate test precision or to detect systematic analytical deviations that may arise from reagent or analytical instrument variation. This type of device consists of single or multiple microbiological analytes intended for use with either qualitative or quantitative assays.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include detailed device description documentation and information concerning the composition of the quality control material, including, as appropriate:
(i) Analyte concentration;
(ii) Expected values;
(iii) Analyte source;
(iv) Base matrix;
(v) Added components;
(vi) Safety and handling information; and
(vii) Detailed instructions for use.
(2) Premarket notification submissions must include detailed documentation, including line data as well as detailed study protocols and a statistical analysis plan used to establish performance, including:
(i) Description of the process for value assignment and validation.
(ii) Description of the protocol(s) used to establish stability.
(iii) Line data establishing precision/reproducibility.
(iv) Where applicable, assessment of matrix effects and any significant differences between the quality control material and typical patient samples in terms of conditions known to cause analytical error or affect assay performance.
(v) Where applicable, identify or define traceability or relationship to a domestic or international standard reference material and/or method.
(vi) Where applicable, detailed documentation related to studies for surrogate controls.
(3) Premarket notification submissions must include an adequate mitigation (e.g., real-time stability program) to the risk of false results due to potential modifications to the assays specified in the device's 21 CFR 809.10 compliant labeling.
(4) Your 21 CFR 809.10 compliant labeling must include the following:
(i) The intended use of your 21 CFR 809.10(a)(2) and (b)(2) compliant labeling must include the following:
(A) Assayed control material analyte(s);
(B) Whether the material is intended for quantitative or qualitative assays;
(C) Stating if the material is a surrogate control; and
(D) The system(s), instrument(s), or test(s) for which the quality control material is intended.
(ii) The intended use in your 21 CFR 809.10(a)(2) and (b)(2) compliant labeling must include the following statement: "This product is not intended to replace manufacturer controls provided with the device."
(iii) A limiting statement that reads "Quality control materials should be used in accordance with local, state, federal regulations, and accreditation requirements."
[82 FR 34850, July 27, 2017]
|
|
|
Sec. 866.3930 Vibrio cholerae serological reagents.
|
|
(a) Identification. Vibrio cholerae serological reagents are devices that are used in the agglutination (an antigen-antibody clumping reaction) test to identify Vibrio cholerae from cultured isolates derived from clinical specimens. The identification aids in the diagnosis of cholera caused by the bacterium Vibrio cholerae and provides epidemiological information on cholera. Cholera is an acute infectious disease characterized by severe diarrhea with extreme fluid and electrolyte (salts) depletion, and by vomiting, muscle cramps, and prostration. If untreated, the severe dehydration may lead to shock, renal failure, cardiovascular collapse, and death.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.3940 West Nile virus serological reagents.
|
|
(a) Identification. West Nile virus serological reagents are devices that consist of antigens and antisera for the detection of anti-West Nile virus IgM antibodies, in human serum, from individuals who have signs and symptoms consistent with viral meningitis/encephalitis. The detection aids in the clinical laboratory diagnosis of viral meningitis/encephalitis caused by West Nile virus.
(b) Classification. Class II (special controls). The special control is FDA's guidance entitled "Class II Special Controls Guidance Document: Serological Reagents for the Laboratory Diagnosis of West Nile Virus." See § 866.1(e) for the availability of this guidance document.
[68 FR 61745, Oct. 30, 2003]
|
|
|
Sec. 866.3945 Dengue virus serological reagents.
|
|
(a) Identification. Dengue virus serological reagents are devices that consist of antigens and antibodies for the detection of dengue virus and dengue antibodies in individuals who have signs and symptoms of dengue fever or dengue hemorrhagic fever. The detection aids in the clinical laboratory diagnosis of dengue fever or dengue hemorrhagic fever caused by dengue virus.
(b) Classification. Class II (special controls). The special control is FDA's guideline entitled "Class II Special Controls Guideline: Dengue Virus Serological Reagents." For availability of the guideline document, see § 866.1(e).
[79 FR 31023, May 30, 2014]
|
|
|
Sec. 866.3946 Dengue virus nucleic acid amplification test reagents.
|
|
(a) Identification. Dengue virus nucleic acid amplification test reagents are devices that consist of primers, probes, enzymes, and controls for the amplification and detection of dengue virus serotypes 1, 2, 3, or 4 from viral ribonucleic acid (RNA) in human serum and plasma from individuals who have signs and symptoms consistent with dengue (mild or severe). The identification of dengue virus serotypes 1, 2, 3, or 4 in human serum and plasma (sodium citrate) collected from human patients with dengue provides epidemiologic information for surveillance of circulating dengue viruses.
(b) Classification. Class II (special controls). The special control is FDA's guideline entitled "Class II Special Controls Guideline: Dengue Virus Nucleic Acid Amplification Test Reagents." For availability of the guideline document, see § 866.1(e).
[79 FR 53609, Sept. 10, 2014]
|
|
|
Sec. 866.3950 In vitro human immunodeficiency virus (HIV) drug resistance genotype assay.
|
|
(a) Identification. The in vitro HIV drug resistance genotype assay is a device that consists of nucleic acid reagent primers and probes together with software for predicting drug resistance/susceptibility based on results obtained with these primers and probes. It is intended for use in detecting HIV genomic mutations that confer resistance to specific antiretroviral drugs, as an aid in monitoring and treating HIV infection.
(b) Classification. Class II (special controls). The special control for this device is FDA's guidance document entitled "Class II Special Controls Guidance Document: In Vitro HIV Drug Resistance Genotype Assay." See § 866.1(e) for the availability of this guidance document.
[72 FR 44382, Aug. 8, 2007]
|
|
|
Sec. 866.3955 Human immunodeficiency virus (HIV) drug resistance genotyping assay using next generation sequencing technology.
|
|
(a) Identification. The HIV drug resistance genotyping assay using next generation sequencing (NGS) technology is a prescription in vitro diagnostic device intended for use in detecting HIV genomic mutations that confer resistance to specific antiretroviral drugs. The device is intended to be used as an aid in monitoring and treating HIV infection.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The intended use of the device must:
(i) Specify the analyte (RNA or DNA), the genes in which mutations are detected, the clinical indications appropriate for test use, the sample type, and the specific population(s) for which the device in intended.
(ii) State that the device in not intended for use as an aid in the diagnosis of infection with HIV or to confirm the presence of HIV infection, or for screening donors of blood, plasma, or human cells, tissues, and cellular and tissue-based products.
(2) The labeling must include:
(i) A detailed device description, including but not limited to, all procedures from collection of the patient sample to reporting the final result, all device components, the control elements incorporated into the test procedure, instrument requirements, and reagents required for use but not provided as part of the device.
(ii) Performance characteristics from analytical studies and all intended specimen types.
(iii) A list of specific mutations detected.
(iv) The name and version of the standardized database used for sequence comparison and results derivation.
(v) A detailed explanation of the interpretation of test results, including acceptance criteria for evaluating the validity of a test run.
(vi) A limitation statement that the device is intended to be used in conjunction with clinical history and other laboratory findings. Results of this test are intended to be interpreted by a physician or equivalent.
(vii) A limitation statement that lack of detection of drug resistance mutations does not preclude the possibility of genetic mutation.
(viii) A limitation statement indicating the relevant genetic mutations that are included in the standardized database of HIV genomic sequences used for comparison and results derivation but that are not detected by the test.
(ix) A limitation statement that detection of a genomic drug resistance mutation may not correlate with phenotypic gene expression.
(x) A limitation statement that the test does not detect all genetic mutations associated with antiviral drugs.
(xi) A limitation statement listing the HIV types for which the test is not intended, if any.
(3) Device verification and validation must include:
(i) Design of primer sequences and rationale for sequence selection.
(ii) Computational path from collected raw data to reported result.
(iii) Detailed documentation of analytical studies including, but not limited to, characterization of the cutoff, analytical sensitivity, inclusivity, reproducibility, interference, cross reactivity, instrument and method carryover/cross contamination, sample stability, and handling for all genomic mutations claimed in the intended use.
(iv) Precision studies that include all genomic mutations claimed in the intended use.
(v) Detailed documentation of a multisite clinical study evaluating the sensitivity and specificity of the device. Clinical study subjects must represent the intended use population and device results for all targets claimed in the intended use must be compared to Sanger sequencing or other methods found acceptable by FDA. Drug resistance-associated mutations at or above the 20 percent frequency level must detect the mutations in greater than 90 percent of at least 10 replicates, for each of drug class evaluated.
(vi) Documentation that variant calling is performed at a level of coverage that supports positive detection of all genomic mutations claimed in the intended use.
(vii) Detailed documentation of limit of detection (LoD) studies in which device performance is evaluated by testing a minimum of 100 HIV-positive clinical samples including samples with analyte concentrations near the clinical decision points and near the LoD.
(A) The LoD for the device must be determined using a minimum of 10 HIV-1 group M genotypes if applicable. A detection rate at 1 * LoD greater than or equal to 95 percent must be demonstrated for mutations with a frequency greater than 20 percent.
(B) The LoD of genetic mutations at frequency levels less than 20 percent must be established.
(viii) A predefined HIV genotyping bioinformatics analysis pipeline (BAP). The BAP must adequately describe the bioinformatic analysis of the sequencing data, including but not limited to read alignment, variant calling, assembly, genotyping, quality control, and final result reporting.
(ix) A clear description of the selection and use of the standardized database that is used for sequence comparison and results derivation.
(4) Premarket notification submissions must include the information in paragraphs (b)(3)(i) through (ix) of this section.
[85 FR 7217, Feb. 7, 2020]
|
|
|
Sec. 866.3956 Human immunodeficiency virus (HIV) serological diagnostic and/or supplemental test.
|
|
(a) Identification. Human immunodeficiency virus (HIV) serological diagnostic and supplemental tests are prescription devices for the qualitative detection of HIV antigen(s) and/or detection of antibodies against HIV in human body fluids or tissues. The tests are intended for use as an aid in the diagnosis of infection with HIV and are for professional use only. The test results are intended to be interpreted in conjunction with other relevant clinical and laboratory findings. These tests are not intended to be used for monitoring patient status, or for screening donors of blood or blood products, or human cells, tissues, and cellular and tissue-based products (HCT/Ps).
(b) Classification. Class II (special controls). The special controls for this device are:
(1) For all HIV serological diagnostic and supplemental tests
(i) The labeling must include:
(A) An intended use that states that the device is not intended for use for screening donors of blood or blood products or HCT/Ps.
(B) A detailed explanation of the principles of operation and procedures used for performing the assay.
(C) A detailed explanation of the interpretation of results and recommended actions to take based on results.
(D) Limitations, which must be updated to reflect current clinical practice and disease presentation and management. The limitations must include, but are not limited to, statements that indicate:
(1 ) The matrices with which the device has been cleared, and that use of this test kit with specimen types other than those specifically cleared for this device may result in inaccurate test results.
(2 ) The test is not intended to be used to monitor individuals who are undergoing treatment for HIV infection.
(3 ) A specimen with a reactive result should be investigated further following current guidelines.
(4 ) All test results should be interpreted in conjunction with the individual's clinical presentation, history, and other laboratory results.
(5 ) A test result that is nonreactive does not exclude the possibility of exposure to or infection with HIV. Nonreactive results in this assay may be due to analyte levels that are below the limit of detection of this assay.
(ii) Device verification and validation must include:
(A) Detailed device description, including the device components, ancillary reagents required but not provided, and an explanation of the methodology. Additional information appropriate to the technology must be included, such as the amino acid sequence of antigen(s) and design of capture antibodies.
(B) For devices with assay calibrators, the design of all primary, secondary, and subsequent quantitation standards used for calibration as well as their traceability to a reference material. In addition, analytical testing must be performed following the release of a new lot of the standard material that was used for device clearance, or when there is a transition to a new calibration standard.
(C) Detailed documentation of analytical performance studies conducted as appropriate to the technology, specimen types tested, and intended use of the device, including, but not limited to, limit of blank, limit of detection, cutoff determination, precision, endogenous and exogenous interferences, cross reactivity, carryover, quality control, matrix equivalency, and sample and reagent stability. Samples selected for use in analytical studies or used to prepare samples for use in analytical studies must be from subjects with clinically relevant circulating genotypes in the United States.
(D) Multisite reproducibility study that includes the testing of three independent production lots.
(E) Analytical sensitivity of the test must be the same as or better than that of other cleared or approved tests. Samples tested must include appropriate numbers and types of samples, including real clinical samples near the lower limit of detection. Analytical specificity of the test must be the same as or better than that of other cleared or approved tests. Samples must include appropriate numbers and types of samples from patients with different underlying illnesses or infections and from patients with potential endogenous interfering substances.
(F) Detailed documentation of performance from a multisite clinical study. Performance must be analyzed relative to an FDA-cleared or approved comparator. This study must be conducted using patient samples, with an appropriate number of HIV positive and HIV negative samples in applicable risk categories. Additional subgroups or types must be validated using appropriate numbers and types of samples. The samples may be a combination of fresh and repository samples, sourced from within and outside the United States, as appropriate. The study designs, including number of samples tested, must be sufficient to meet the following criteria:
(1 ) Clinical sensitivity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 99 percent.
(2 ) Clinical specificity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 99 percent.
(G) Strategies for detection of new strains, types, subtypes, genotypes, and genetic mutations as they emerge.
(H) Risk analysis and management strategies, such as Failure Modes Effects Analysis and/or Hazard Analysis and Critical Control Points summaries and their impact on test performance.
(I) Final release criteria to be used for manufactured test lots with appropriate evidence that lots released at the extremes of the specifications will meet the claimed analytical and clinical performance characteristics as well as the stability claims.
(J) All stability protocols, including acceptance criteria.
(K) Appropriate and acceptable procedure(s) for evaluating customer complaints and other device information that determines when to submit a medical device report.
(L) Premarket notification submissions must include the information contained in paragraph (b)(1)(ii)(A) through (K) of this section.
(iii) Manufacturers must submit a log of all complaints. The log must include the following information regarding each complaint if available: The type of event (e.g., false negative/false nonreactive or false positive/false reactive), lot, date, population, and whether or not the complaint was reported under part 803 of this chapter (Medical Device Reporting). The log must be submitted annually on the anniversary of clearance for 5 years following clearance of a traditional premarket notification.
(2) If the test is intended for Point of Care (PoC) use, the following special controls, in addition to those listed in paragraph (b)(1) of this section apply:
(i) The PoC labeling must include a statement that the test is intended for PoC use.
(ii) The PoC labeling must include the following information near the statement of the intended use:
(A) That the test is for distribution to clinical laboratories that have an adequate quality assurance program, including planned systematic activities that provide adequate confidence that requirements for quality will be met and where there is assurance that operators will receive and use the instructional materials.
(B) That the test is for use only by an agent of a clinical laboratory.
(C) Instructions for individuals to receive the "Subject Information Notice" prior to specimen collection and appropriate information when test results are provided.
(iii) PoC labeling must include instructions to follow current guidelines for informing the individual of the test result and its interpretation.
(iv) The instructions in the labeling must state that reactive results are considered preliminary and should be confirmed following current guidelines.
(v) Device verification and validation for PoC use must include:
(A) Detailed documentation of performance from a multisite clinical study conducted at appropriate PoC sites. Performance must be analyzed relative to an FDA cleared or approved comparator. This study must be conducted using patient samples, with appropriate numbers of HIV positive and HIV negative samples in applicable risk categories. Additional subgroup or type claims must be validated using appropriate numbers and types of samples. The samples may be a combination of fresh and repository samples, sourced from within and outside the United States, as appropriate. If the test is intended solely for PoC use, the test must meet only the performance criteria in paragraphs (b)(2)(v)(A)(1 ) and (2 ) of this section and not the criteria in paragraph (b)(1)(ii)(F) of this section:
(1 ) Clinical sensitivity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 98 percent.
(2 ) Clinical specificity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 98 percent.
(B) Premarket notification submissions must include the information contained in paragraph (b)(2)(v)(A) of this section.
(3) If the test is intended for supplemental use in addition to use as an aid in initial diagnosis, the following special controls, in addition to those listed in paragraphs (b)(1) and (2) of this section, as appropriate, apply:
(i) The labeling must include a statement that the test is intended for use as an additional test to confirm the presence of HIV antibodies or antigens in specimens found to be repeatedly reactive by a diagnostic screening test.
(ii) Device validation and verification for supplemental use must include a clinical study, including samples that were initially reactive and repeatedly reactive on a diagnostic test but were negative or indeterminate on a different confirmatory test. Premarket notification submissions must include this information.
(4) If the test is intended solely as a supplemental test, the following special controls, in addition to those listed in paragraphs (b)(1) and (2) of this section, except those in paragraphs (b)(1)(ii)(F) and (b)(2)(v)(A) of this section, as appropriate, apply:
(i) The labeling must include a statement that the test is intended for use as an additional test to confirm the presence of HIV antibodies or antigens in specimens found to be repeatedly reactive by a diagnostic screening test.
(ii) The labeling must clearly state that the test is not for use for initial diagnosis or is not intended as a first-line test.
(iii) Device validation and verification must include a clinical study including samples that were initially reactive and repeatedly reactive on a diagnostic test but were negative or indeterminate on a confirmatory test. Premarket notification submissions must include this information.
(5) If the test is intended to differentiate different HIV types, the following special controls, in addition to those listed in paragraphs (b)(1) through (4) of this section, as appropriate, apply:
(i) The labeling must include the statement that the test is intended for the confirmation of initial results from a diagnostic test and differentiation of different HIV types.
(ii) The results interpretation in the labeling must include instructions for the user on how to interpret the results, including un-typeable and co-infection results.
(iii) Device validation and verification must include evaluation of analytical and clinical sensitivity and specificity for each of the HIV types, strains, and subtypes of HIV intended to be differentiated. Premarket notification submissions must include this information.
[87 FR 29665, May 16, 2022]
|
|
|
Sec. 866.3957 Human immunodeficiency virus (HIV) nucleic acid (NAT) diagnostic and/or supplemental test.
|
|
(a) Identification. Human immunodeficiency virus (HIV) nucleic acid (NAT) diagnostic and supplemental tests are prescription devices for the qualitative detection of HIV nucleic acid in human body fluids or tissues. The tests are intended for use as an aid in the diagnosis of infection with HIV and are for professional use only. The test results are intended to be interpreted in conjunction with other relevant clinical and laboratory findings. These tests are not intended to be used for monitoring patient status, or for screening donors of blood or blood products, or human cells, tissues, or cellular or tissue-based products (HCT/Ps).
(b) Classification. Class II (special controls). The special controls for this device are:
(1) For all HIV NAT diagnostic and/or supplemental tests
(i) The labeling must include:
(A) An intended use that states that the device is not intended for use for screening donors of blood or blood products, or HCT/Ps.
(B) A detailed explanation of the principles of operation and procedures used for performing the assay.
(C) A detailed explanation of the interpretation of results and recommended actions to take based on results.
(D) Limitations, which must be updated to reflect current clinical practice and disease presentation and management. The limitations must include, but are not limited to, statements that indicate:
(1 ) The matrices with which the device has been cleared, and that use of this test kit with specimen types other than those specifically cleared for this device may result in inaccurate test results.
(2 ) The test is not intended to be used to monitor individuals who are undergoing treatment for HIV infection.
(3 ) A specimen with a reactive result should be investigated further following current guidelines.
(4 ) All test results should be interpreted in conjunction with the individual's clinical presentation, history, and other laboratory results.
(5 ) A test result that is nonreactive does not exclude the possibility of exposure to or infection with HIV. Nonreactive results in this assay may be due to analyte levels that are below the limit of detection of this assay.
(ii) Device verification and validation must include:
(A) Detailed device description, including the device components, ancillary reagents required but not provided, and an explanation of the methodology. Additional information appropriate to the technology must be included, such as design of primers and probes.
(B) For devices with assay calibrators, the design and nature of all primary, secondary, and subsequent quantitation standards used for calibration as well as their traceability to a reference material. In addition, analytical testing must be performed following the release of a new lot of the standard material that was used for device clearance, or when there is a transition to a new calibration standard.
(C) Detailed documentation of analytical performance studies conducted as appropriate to the technology, specimen types tested, and intended use of the device, including, but not limited to, limit of blank, limit of detection, cutoff determination, precision, endogenous and exogenous interferences, cross reactivity, carryover, quality control, matrix equivalency, and sample and reagent stability. Samples selected for use in analytical studies or used to prepare samples for use in analytical studies must be from subjects with clinically relevant circulating genotypes in the United States. The effect of each claimed nucleic-acid isolation and purification procedure on detection must be evaluated.
(D) Multisite reproducibility study that includes the testing of three independent production lots.
(E) Analytical sensitivity of the test must be the same as or better than that of other cleared or approved tests. Samples tested must include appropriate numbers and types of samples, including real clinical samples near the lower limit of detection. Analytical specificity of the test must be as the same as or better than that of other cleared or approved tests. Samples must include appropriate numbers and types of samples from patients with different underlying illnesses or infections and from patients with potential endogenous interfering substances.
(F) Detailed documentation of performance from a multisite clinical study. Performance must be analyzed relative to an FDA cleared or approved comparator. This study must be conducted using appropriate patient samples, with appropriate numbers of HIV positive and negative samples in applicable risk categories. Additional subtype, strain, or types must be validated using appropriate numbers and types of samples. The samples may be a combination of fresh and repository samples, sourced from within and outside the United States, as appropriate. The study designs, including number of samples tested, must be sufficient to meet the following criteria:
(1 ) Clinical sensitivity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 99 percent.
(2 ) Clinical specificity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 99 percent.
(G) Strategies for detection of new strains, types, subtypes, genotypes, and genetic mutations as they emerge.
(H) Risk analysis and management strategies, such as Failure Modes Effects Analysis and/or Hazard Analysis and Critical Control Points summaries and their impact on test performance.
(I) Final release criteria to be used for manufactured test lots with appropriate evidence that lots released at the extremes of the specifications will meet the claimed analytical and clinical performance characteristics as well as the stability claims.
(J) All stability protocols, including acceptance criteria.
(K) Appropriate and acceptable procedure(s) for evaluating customer complaints and other device information that determine when to submit a medical device report.
(L) Premarket notification submissions must include the information contained in paragraph (b)(1)(ii)(A) through (K) of this section.
(iii) Manufacturers must submit a log of all complaints. The log must include the following information regarding each complaint, if available: The type of event (e.g., false negative/false nonreactive or false positive/false reactive), lot, date, population, and whether or not the complaint was reported under part 803 of this chapter (Medical Device Reporting). The log must be submitted annually on the anniversary of clearance for 5 years following clearance of a traditional premarket notification.
(2) If the test is intended for Point of Care (PoC) use, the following special controls, in addition to those listed in paragraph (b)(1) of this section, apply:
(i) The PoC labeling must include a statement that the test is intended for PoC use.
(ii) The PoC labeling must include the following information near the statement of the intended use:
(A) That the test is for distribution to clinical laboratories that have an adequate quality assurance program, including planned systematic activities that provide adequate confidence that requirements for quality will be met and where there is assurance that operators will receive and use the instructional materials.
(B) That the test is for use only by an agent of a clinical laboratory.
(C) Instructions for individuals to receive the "Subject Information Notice" prior to specimen collection and appropriate information when test results are provided.
(iii) PoC labeling must include instructions to follow current guidelines for informing the individual of the test result and its interpretation.
(iv) The instructions in the labeling must state that reactive results are considered preliminary and should be confirmed following current guidelines.
(v) Device verification and validation for PoC use must include:
(A) Detailed documentation from a well-conducted multisite clinical study conducted at appropriate PoC sites. Performance must be analyzed relative to an FDA cleared or approved comparator. This study must be conducted using patient samples, with appropriate numbers of HIV positive and HIV negative samples in applicable risk categories. Additional subgroup or type claims must be validated using appropriate numbers and types of samples. The samples may be a combination of fresh and repository samples, sourced from within and outside the United States, as appropriate. If the test is intended solely for PoC use, the test must meet only the performance criteria in paragraphs (b)(2)(v)(A)(1 ) and (2 ) of this section and not the criteria in paragraph (b)(1)(ii)(F) of this section:
(1 ) Clinical sensitivity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 98 percent.
(2 ) Clinical specificity of the test must have a lower bound of the 95 percent confidence interval of greater than or equal to 98 percent.
(B) Premarket notification submissions must include the information contained in paragraph (b)(2)(v)(A) of this section.
(3) If the test is intended for supplemental use in addition to use as an aid in initial diagnosis, the following special controls, in addition to those listed in paragraphs (b)(1) and (2) of this section, as appropriate, apply:
(i) The labeling must include a statement that the test is intended for use as an additional test to confirm the presence of HIV viral nucleic acid in specimens found to be repeatedly reactive by a diagnostic screening test.
(ii) Device validation and verification for supplemental use must include a clinical study, including samples that were initially reactive and repeatedly reactive on a diagnostic test but were negative or indeterminate on a confirmatory test. Premarket notification submissions must include this information.
(4) If the test is intended solely as a supplemental test, the following special controls, in addition to those listed in paragraphs (b)(1) and (2) of this section, except those in paragraphs (b)(1)(ii)(F) and (b)(2)(v)(A) of this section, as appropriate, apply:
(i) The labeling must include a statement that the test is intended for use as an additional test to confirm the presence of HIV viral nucleic acid in specimens found to be repeatedly reactive by a diagnostic screening test.
(ii) The labeling must clearly state that the test is not for use for initial diagnosis or is not intended as a first-line test.
(iii) Device validation and verification must include a clinical study including samples that were initially reactive and repeatedly reactive on a diagnostic test but were negative or indeterminate on a confirmatory test. Premarket notification submissions must include this information.
(5) If the test is intended to differentiate different HIV types, the following special controls, in addition to those listed in paragraphs (b)(1) through (4) of this section, as appropriate, apply:
(i) The labeling must include the statement that the test is intended for the confirmation of initial results and differentiation of different HIV types.
(ii) The results interpretation in the labeling must include instructions for the user on how to interpret the results, including un-typeable and co-infection results.
(iii) Device validation and verification must include evaluation of analytical and clinical sensitivity and specificity for each of the types, strains, and subtypes of HIV intended to be differentiated. Premarket notification submissions must include this information.
[87 FR 29667, May 16, 2022]
|
|
|
Sec. 866.3958 Human immunodeficiency virus (HIV) viral load monitoring test.
|
|
(a) Identification. A human immunodeficiency virus (HIV) viral load monitoring test is an in vitro diagnostic prescription device for the quantitation of the amount of HIV ribonucleic acid (RNA) in human body fluids. The test is intended for use in the clinical management of individuals living with HIV and is for professional use only. The test results are intended to be interpreted in conjunction with other relevant clinical and laboratory findings. The test is not intended to be used as an aid in diagnosis or for screening donors of blood or blood products or human cells, tissues, or cellular and tissue-based products (HCT/Ps).
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The labeling must include:
(i) An intended use that states that the device is not intended for use as an aid in diagnosis or for use in screening donors of blood or blood products, or HCT/Ps.
(ii) A detailed explanation of the principles of operation and procedures used for assay performance.
(iii) A detailed explanation of the interpretation of results and that recommended actions should be based on current clinical guidelines.
(iv) Limitations, which must be updated to reflect current clinical practice and patient management. The limitations must include, but are not limited to, statements that indicate:
(A) The matrices and sample types with which the device has been cleared and that use of this test with specimen types other than those specifically cleared for this device may cause inaccurate test results.
(B) Mutations in highly conserved regions may affect binding of primers and/or probes resulting in the under-quantitation of virus or failure to detect the presence of virus.
(C) All test results should be interpreted in conjunction with the individual's clinical presentation, history, and other laboratory results.
(2) Device verification and validation must include:
(i) Detailed device description, including the device components, ancillary reagents required but not provided, and an explanation of the device methodology. Additional information appropriate to the technology must be included, such as detailed information on the design of primers and probes.
(ii) For devices with assay calibrators, the design and nature of all primary, secondary, and subsequent quantitation standards used for calibration as well as their traceability to a reference material. In addition, analytical testing must be performed following the release of a new lot of the standard material that was used for device clearance, or when there is a transition to a new calibration standard.
(iii) Detailed documentation of analytical performance studies conducted as appropriate to the technology, specimen types tested, and intended use of the device, including but not limited to, limit of blank, limit of detection, limit of quantitation, cutoff determination, precision, linearity, endogenous and exogenous interferences, cross-reactivity, carry-over, quality control, matrix equivalency, sample and reagent stability. Samples selected for use in analytical studies or used to prepare samples for use in analytical studies must be from subjects with clinically relevant genotypes circulating in the United States.
(iv) Multisite reproducibility study that includes the testing of three independent production lots.
(v) Analytical sensitivity of the device must demonstrate acceptable performance at current clinically relevant medical decision points. Samples tested to demonstrate analytical sensitivity must include appropriate numbers and types of samples, including real clinical samples near the lower limit of quantitation and any clinically relevant medical decision points. Analytical specificity of the device must demonstrate acceptable performance. Samples tested to demonstrate analytical specificity must include appropriate numbers and types of samples from patients with different underlying illnesses and infection and from patients with potential interfering substances.
(vi) Detailed documentation of performance from a multisite clinical study or a multisite analytical method comparison study.
(A) For devices evaluated in a multisite clinical study, the study must use specimens from individuals living with HIV being monitored for changes in viral load, and the test results must be compared to the clinical status of the patients.
(B) For tests evaluated in a multisite analytical method comparison study, the performance of the test must be compared to an FDA-cleared or approved comparator. The multisite method comparison study must include appropriate numbers and types of samples with analyte concentrations across the measuring range of the assay, representing clinically relevant genotypes. The multisite method comparison study design, including number of samples tested, must be sufficient to meet the following criteria:
(1 ) Agreement between the two tests across the measuring range of the assays must have an r2 of greater than or equal to 0.95.
(2 ) The bias between the test and comparator assay, as determined by difference plots, must be less than or equal to 0.5 log copies/mL.
(vii) Detailed documentation of a single-site analytical method comparison study between the device and an FDA-cleared or approved comparator if a multisite clinical study is performed under paragraph(b)(2)(vi) of this section. The analytical method comparison study must use appropriate numbers and types of samples with analyte concentrations across the measuring range of the assay, representing clinically relevant genotypes. The results must meet the criteria in paragraphs (b)(2)(vi)(B)(1 ) and (2 ) of this section.
(viii) Strategies for detection of new strains, types, subtypes, genotypes, and genetic mutations as they emerge.
(ix) Risk analysis and management strategies, such as Failure Modes Effects Analysis and/or Hazard Analysis and Critical Control Points summaries and their impact on test performance.
(x) Final release criteria to be used for manufactured device lots with an appropriate justification that lots released at the extremes of the specifications will meet the claimed analytical and clinical performance characteristics as well as the stability claims.
(xi) All stability protocols, including acceptance criteria.
(xii) Appropriate and acceptable procedure(s) for addressing complaints and other device information that determines when to submit a medical device report.
(xiii) Premarket notification submissions must include the information contained in paragraphs (b)(2)(i) through (xii) of this section.
[87 FR 66548, Nov. 4, 2022]
|
|
|
Sec. 866.3960 Nucleic acid-based device for the amplification, detection, and identification of microbial pathogens directly from whole blood specimens.
|
|
(a) Identification. A nucleic acid-based device for the amplification, detection, and identification of microbial pathogens directly from whole blood specimens is a qualitative in vitro device intended for the amplification, detection, and identification of microbial-associated nucleic acid sequences from patients with suspected bloodstream infections. This device is intended to aid in the diagnosis of bloodstream infection when used in conjunction with clinical signs and symptoms and other laboratory findings.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include detailed device description documentation, including the device components, ancillary reagents required but not provided, and a detailed explanation of the methodology, including primer/probe sequence, design, and rationale for sequence selection.
(2) Premarket notification submissions must include detailed documentation from the following analytical and clinical performance studies: Analytical sensitivity (limit of detection), reactivity, inclusivity, precision, reproducibility, interference, cross reactivity, carryover, and cross contamination.
(3) Premarket notification submissions must include detailed documentation from a clinical study. The study, performed on a study population consistent with the intended use population, must compare the device performance to results obtained from well-accepted reference methods.
(4) Premarket notification submissions must include detailed documentation for device software, including, but not limited to, software applications and hardware-based devices that incorporate software.
(5) The device labeling must include limitations regarding the need for culture confirmation of negative specimens, as appropriate.
(6) A detailed explanation of the interpretation of results and acceptance criteria must be included in the device's 21 CFR 809.10(b)(9) compliant labeling.
(7) Premarket notification submissions must include details on an end user device training program that will be offered while marketing the device, as appropriate.
(8) As part of the risk management activities performed as part of your 21 CFR 820.30 design controls, you must document an appropriate end user device training program that will be offered as part of your efforts to mitigate the risk of failure to correctly operate the instrument.
[82 FR 47967, Oct. 16, 2017]
|
|
|
Sec. 866.3970 Device to detect and identify microbial pathogen nucleic acids in cerebrospinal fluid.
|
|
(a) Identification. A device to detect and identify microbial pathogen nucleic acids in cerebrospinal fluid is a qualitative in vitro device intended for the detection and identification of microbial-associated nucleic acid sequences from patients suspected of meningitis or encephalitis. A device to detect and identify microbial pathogen nucleic acids in cerebrospinal fluid is intended to aid in the diagnosis of meningitis or encephalitis when used in conjunction with clinical signs and symptoms and other clinical and laboratory findings.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include detailed device description documentation, including the device components, ancillary reagents required but not provided, and a detailed explanation of the methodology, including primer/probe sequence, design, and rationale for sequence selection.
(2) Premarket notification submissions must include detailed documentation from the following analytical studies: Analytical sensitivity (limit of detection), inclusivity, reproducibility, interference, cross reactivity, and specimen stability.
(3) Premarket notification submissions must include detailed documentation from a clinical study. The study, performed on a study population consistent with the intended use population, must compare the device performance to results obtained from well-accepted comparator methods.
(4) Premarket notification submissions must include detailed documentation for device software, including, but not limited to, software applications and hardware-based devices that incorporate software.
(5) The Intended Use statement in the device labeling must include a statement that the device is intended to be used in conjunction with standard of care culture.
(6) A detailed explanation of the interpretation of results and acceptance criteria must be included in the device's 21 CFR 809.10(b)(9) compliant labeling.
(7) The device labeling must include a limitation stating that the negative results do not preclude the possibility of central nervous system infection.
(8) The device labeling must include a limitation stating that device results are not intended to be used as the sole basis for diagnosis, treatment, or other patient management decisions.
(9) The device labeling must include a limitation stating that positive results do not mean that the organism detected is infectious or is the causative agent for clinical symptoms.
(10) As part of the risk management activities performed as part of your 21 CFR 820.30 design controls, you must document an appropriate end user device training program that will be offered as part of your efforts to mitigate the risk of failure to correctly operate the instrument.
[82 FR 48763, Oct. 20, 2017]
|
|
|
Sec. 866.3980 Respiratory viral panel multiplex nucleic acid assay.
|
|
(a) Identification. A respiratory viral panel multiplex nucleic acid assay is a qualitative in vitro diagnostic device intended to simultaneously detect and identify multiple viral nucleic acids extracted from human respiratory specimens or viral culture. The detection and identification of a specific viral nucleic acid from individuals exhibiting signs and symptoms of respiratory infection aids in the diagnosis of respiratory viral infection when used in conjunction with other clinical and laboratory findings. The device is intended for detection and identification of a combination of the following viruses:
(1) Influenza A and Influenza B;
(2) Influenza A subtype H1 and Influenza A subtype H3;
(3) Respiratory Syncytial Virus subtype A and Respiratory Syncytial Virus subtype B;
(4) Parainfluenza 1, Parainfluenza 2, and Parainfluenza 3 virus;
(5) Human Metapneumovirus;
(6) Rhinovirus; and
(7) Adenovirus.
(b) Classification. Class II (special controls). The special controls are:
(1) FDA's guidance document entitled "Class II Special Controls Guidance Document: Respiratory Viral Panel Multiplex Nucleic Acid Assay;"
(2) For a device that detects and identifies Human Metapneumovirus, FDA's guidance document entitled "Class II Special Controls Guidance Document: Testing for Human Metapneumovirus (hMPV) Using Nucleic Acid Assays;" and
(3) For a device that detects and differentiates Influenza A subtype H1 and subtype H3, FDA's guidance document entitled "Class II Special Controls Guidance Document: Testing for Detection and Differentiation of Influenza A Virus Subtypes Using Multiplex Nucleic Acid Assays." See § 866.1(e) for the availability of these guidance documents.
[74 FR 52138, Oct. 9, 2009]
|
|
|
Sec. 866.3985 Device to detect and identify microorganisms and associated resistance marker nucleic acids directly in respiratory specimens.
|
|
(a) Identification. A device to detect and identify microorganisms and associated resistance marker nucleic acids directly from respiratory specimens is an in vitro diagnostic device intended for the detection and identification of microorganisms and associated resistance markers in respiratory specimens collected from patients with signs or symptoms of respiratory infection. The device is intended to aid in the diagnosis of respiratory infection in conjunction with clinical signs and symptoms and other laboratory findings. These devices do not provide confirmation of antibiotic susceptibility since mechanisms of resistance may exist other than those detected by the device.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The intended use for the 21 CFR 809.10 labeling must include a detailed description of what the device detects, the type of results provided to the user, the clinical indications appropriate for test use, and the specific population(s) for which the device is intended.
(2) The 21 CFR 809.10(b) labeling must include:
(i) A detailed device description, including all device components, control elements incorporated into the test procedure, instrument requirements, ancillary reagents required but not provided, and a detailed explanation of the methodology, including all pre-analytical methods for processing of specimens.
(ii) Performance characteristics from analytical studies, including, but not limited to, limit of detection, inclusivity, reproducibility, cross reactivity, interfering substances, competitive inhibition, carryover/cross contamination, specimen stability, and linearity, as applicable.
(iii) A limiting statement that the device is intended to be used in conjunction with clinical history, signs and symptoms, and results of other diagnostic tests, including culture and antimicrobial susceptibility testing.
(iv) A detailed explanation of the interpretation of test results for clinical specimens and acceptance criteria for any quality control testing.
(v) A limiting statement that negative results for microorganisms do not preclude the possibility of infection, and should not be used as the sole basis for diagnosis, treatment, or other patient management decisions.
(vi) If applicable, a limiting statement that detected microorganisms may not be the cause of lower respiratory tract infection and may be indicative of colonizing or normal respiratory flora.
(vii) If applicable, a limiting statement that detection of resistance markers cannot be definitively linked to specific microorganisms and that the source of a detected resistance marker may be an organism not detected by the assay, including colonizing flora.
(viii) If applicable, a limiting statement that detection of antibiotic resistance markers may not correlate with phenotypic gene expression.
(3) The 21 CFR 809.10(b) labeling and any test report generated by the device must include a limiting statement that negative results for resistance markers do not indicate susceptibility of detected microorganisms.
(4) Design verification and validation must include:
(i) Performance characteristics from clinical studies that include prospective (sequential) samples and, if appropriate, additional characterized samples. The study must be performed on a study population consistent with the intended use population and compare the device performance to results obtained from an FDA accepted reference method and/or FDA accepted comparator method, as appropriate. Results from the clinical studies must include the clinical study protocol (including predefined statistical analysis plan, if applicable), clinical study report, and results of all statistical analyses.
(ii) A detailed device description including the following:
(A) Thorough description of the assay methodology including, but not limited to, primer/probe sequences, primer/probe design, and rationale for target sequence selection, as applicable.
(B) Algorithm used to generate a final result from raw data (e.g., how raw signals are converted into a reported result).
(iii) A detailed description of device software, including, but not limited to, validation activities and outcomes.
(iv) As part of the risk management activities, an appropriate end user device training program must be offered as an effort to mitigate the risk of failure from user error.
[84 FR 9228, Mar. 14, 2019]
|
|
|
Sec. 866.3990 Gastrointestinal microorganism multiplex nucleic acid-based assay.
|
|
(a) Identification. A gastrointestinal microorganism multiplex nucleic acid-based assay is a qualitative in vitro diagnostic device intended to simultaneously detect and identify multiple gastrointestinal microbial nucleic acids extracted from human stool specimens. The device detects specific nucleic acid sequences for organism identification as well as for determining the presence of toxin genes. The detection and identification of a specific gastrointestinal microbial nucleic acid from individuals exhibiting signs and symptoms of gastrointestinal infection aids in the diagnosis of gastrointestinal infection when used in conjunction with clinical evaluation and other laboratory findings. A gastrointestinal microorganism multiplex nucleic acid-based assay also aids in the detection and identification of acute gastroenteritis in the context of outbreaks.
(b) Classification. Class II (special controls). The special controls are set forth in FDA's guideline document entitled: "Class II Special Controls Guideline: Gastrointestinal Microorganism Multiplex Nucleic Acid-Based Assays for Detection and Identification of Microorganisms and Toxin Genes from Human Stool Specimens." For availability of the guideline document, see § 866.1(e).
[80 FR 67314, Nov. 2, 2015]
|
|
|
Subpart E - Immunology Laboratory Equipment and Reagents
|
|
Sec. 866.4070 RNA Preanalytical Systems.
|
|
(a) Identification. RNA Preanalytical Systems are devices intended to collect, store, and transport patient specimens, and stabilize intracellular RNA from the specimens, for subsequent isolation and purification of the intracellular RNA for RT-PCR used in in vitro molecular diagnostic testing.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: RNA Preanalytical Systems (RNA Collection, Stabilization and Purification System for RT-PCR Used in Molecular Diagnostic Testing)." See § 866.1(e) for the availability of this guidance document.
[70 FR 49863, Aug. 25, 2005]
|
|
|
Sec. 866.4100 Complement reagent.
|
|
(a) Identification. A complement reagent is a device that consists of complement, a naturally occurring serum protein from any warm-blooded animal such as guinea pigs, that may be included as a component part of serological test kits used in the diagnosis of disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 2001, as amended at 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.4500 Immunoelectrophoresis equipment.
|
|
(a) Identification. Immunoelectrophoresis equipment for clinical use with its electrical power supply is a device used for separating protein molecules. Immunoelectrophoresis is a procedure in which a complex protein mixture is placed in an agar gel and the various proteins are separated on the basis of their relative mobilities under the influence of an electric current. The separated proteins are then permitted to diffuse through the agar toward a multispecific antiserum, allowing precipitation and visualization of the separate complexes.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.4520 Immunofluorometer equipment.
|
|
(a) Identification. Immunofluorometer equipment for clinical use with its electrical power supply is a device used to measure the fluorescence of fluorochrome-labeled antigen-antibody complexes. The concentration of these complexes may be measured by means of reflected light. A beam of light is passed through a solution in which a fluorochrome has been selectively attached to serum protein antibody molecules in suspension. The amount of light emitted by the fluorochrome label is detected by a photodetector, which converts light energy into electrical energy. The amount of electrical energy registers on a readout system such as a digital voltmeter or a recording chart. This electrical readout is called the fluorescence value and is used to measure the concentration of antigen-antibody complexes.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.4540 Immunonephelometer equipment.
|
|
(a) Identification. Immunonephelometer equipment for clinical use with its electrical power supply is a device that measures light scattering from antigen-antibody complexes. The concentration of these complexes may be measured by means of reflected light. A beam of light passed through a solution is scattered by the particles in suspension. The amount of light is detected by a photodetector, which converts light energy into electrical energy. The amount of electrical energy registers on a readout system such as a digital voltmeter or a recording chart. This electrical readout is called the light-scattering value and is used to measure the concentration of antigen-antibody complexes. This generic type of device includes devices with various kinds of light sources, such as laser equipment.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.4600 Ouchterlony agar plate.
|
|
(a) Identification. An ouchterlony agar plate for clinical use is a device containing an agar gel used to examine antigen-antibody reactions. In immunodiffusion, antibodies and antigens migrate toward each other through gel which originally contained neither of these reagents. As the reagents come in contact with each other, they combine to form a precipitate that is trapped in the gel matrix and is immobilized.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.4700 Automated fluorescence in situ hybridization (FISH) enumeration systems.
|
|
(a) Identification. An automated FISH enumeration system is a device that consists of an automated scanning microscope, image analysis system, and customized software applications for FISH assays. This device is intended for in vitro diagnostic use with FISH assays as an aid in the detection, counting and classification of cells based on recognition of cellular color, size, and shape, and in the detection and enumeration of FISH signals in interphase nuclei of formalin-fixed, paraffin-embedded human tissue specimens.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: Automated Fluorescence in situ Hybridization (FISH) Enumeration Systems." See § 866.1(e) for the availability of this guidance document.
[70 FR 14534, Mar. 23, 2005]
|
|
|
Sec. 866.4750 Automated indirect immunofluorescence microscope and software-assisted system.
|
|
(a) Identification. An automated indirect immunofluorescence microscope and software assisted system is a device that acquires, analyzes, stores, and displays digital images of indirect immunofluorescent slides. It is intended to be used as an aid in the determination of antibody status in clinical samples. The device may include a fluorescence microscope with light source, a motorized microscope stage, dedicated instrument controls, a camera, a computer, a sample processor, or other hardware components. The device may use fluorescent signal acquisition and processing software, data storage and transferring mechanisms, or assay specific algorithms to suggest results. A trained operator must confirm results generated with the device.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The labeling for the device must reference legally marketed assays intended for use with the device.
(2) Premarket notification submissions must include the following information:
(i) A detailed description of the device that includes:
(A) A detailed description of instrumentation and equipment, and illustrations or photographs of non-standard equipment or methods, if applicable;
(B) Detailed documentation of the software, including, but not limited to, stand-alone software applications and hardware-based devices that incorporate software, if applicable;
(C) A detailed description of appropriate internal and external quality controls that are recommended or provided. The description must identify those control elements that are incorporated into the recommended testing procedures;
(D) Detailed description and specifications for sample preparation, processing, and storage, if applicable;
(E) Methodology and protocols for detecting fluorescence and visualizing results; and
(F) Detailed specification of the criteria for test results interpretation and reporting.
(ii) Data demonstrating the performance characteristics of the device, which must include:
(A) A comparison study of the results obtained with the conventional manual method (i.e., reference standard), the device, and the reading of the digital image without aid of the software, using the same set of patient samples for each. The study must use a legally marketed assay intended for use with the device. Patient samples must be from the assay-specific intended use population and differential diagnosis population. Samples must also cover the assay measuring range, if applicable;
(B) Device clinical performance established by comparing device results at multiple U.S. sites to the clinical diagnostic standard used in the United States, using patient samples from the assay-specific intended use population and the differential diagnosis population. For all samples, the diagnostic clinical criteria and the demographic information must be collected and provided. Clinical validation must be based on the determination of clinical sensitivity and clinical specificity using the test results (e.g., antibody status based on fluorescence to include pattern and titer, if applicable) compared to the clinical diagnosis of the subject from whom the clinical sample was obtained. The data must be summarized in tabular format comparing the result generated by automated, manual, and digital only interpretation to the disease status;
(C) Device precision/reproducibility data generated from within-run, between-run, between-day, between-lot, between-operator, between-instruments, between-site, and total precision for multiple nonconsecutive days (as applicable) using multiple operators, multiple instruments and at multiple sites. A well-characterized panel of patient samples or pools from the associated assay specific intended use population must be used;
(D) Device linearity data generated from patient samples covering the assay measuring range, if applicable;
(E) Device analytical sensitivity data, including limit of blank, limit of detection, and limit of quantitation, if applicable;
(F) Device assay specific cutoff, if applicable;
(G) Device analytical specificity data, including interference by endogenous and exogenous substances, if applicable;
(H) Device instrument carryover data, if applicable;
(I) Device stability data including real-time stability under various storage times and temperatures, if applicable; and
(J) Information on traceability to a reference material and description of value assignment of calibrators and controls, if applicable.
(iii) Identification of risk mitigation elements used by the device, including description of all additional procedures, methods, and practices, incorporated into the directions for use that mitigate risks associated with testing.
(3) Your 21 CFR 809.10 compliant labeling must include:
(i) A warning statement that reads "The device is for use by a trained operator in a clinical laboratory setting";
(ii) A warning statement that reads "All software-aided results must be confirmed by the trained operator";
(iii) A warning statement that reads "This device is only for use with reagents that are indicated for use with the device"; and
(iv) A description of the protocol and performance studies performed in accordance with paragraph (b)(2)(ii) of this section and a summary of the results, if applicable.
[82 FR 52648, Nov. 14, 2017, as amended at 86 FR 20283, Apr. 19, 2021]
|
|
|
Sec. 866.4800 Radial immunodiffusion plate.
|
|
(a) Identification. A radial immunodiffusion plate for clinical use is a device that consists of a plastic plate to which agar gel containing antiserum is added. In radial immunodiffusion, antigens migrate through gel which originally contains specific antibodies. As the reagents come in contact with each other, they combine to form a precipitate that is trapped in the gel matrix and immobilized.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.4830 Rocket immunoelectrophoresis equipment.
|
|
(a) Identification. Rocket immunoelectrophoresis equipment for clinical use is a device used to perform a specific test on proteins by using a procedure called rocket immunoelectrophoresis. In this procedure, an electric current causes the protein in solution to migrate through agar gel containing specific antisera. The protein precipitates with the antisera in a rocket-shaped pattern, giving the name to the device. The height of the peak (or the area under the peak) is proportional to the concentration of the protein.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Sec. 866.4900 Support gel.
|
|
(a) Identification. A support gel for clinical use is a device that consists of an agar or agarose preparation that is used while measuring various kinds of, or parts of, protein molecules by various immunochemical techniques, such as immunoelectrophoresis, immunodiffusion, or chromatography.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 54 FR 25047, June 12, 1989; 66 FR 38792, July 25, 2001]
|
|
|
Subpart F - Immunological Test Systems
|
|
Sec. 866.5040 Albumin immunological test system.
|
|
(a) Identification. An albumin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the albumin (a plasma protein) in serum and other body fluids. Measurement of albumin aids in the diagnosis of kidney and intestinal diseases.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.5060 Prealbumin immunological test system.
|
|
(a) Identification. A prealbumin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the prealbumin (a plasma protein) in serum and other body fluids. Measurement of prealbumin levels in serum may aid in the assessment of the patient's nutritional status.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5065 Human allotypic marker immunological test system.
|
|
(a) Identification. A human allotypic marker immunological test system is a device that consists of the reagents used to identify by immunochemical techniques the inherited human protein allotypic markers (such as nGm, nA2 m, and Km allotypes) in serum and other body fluids. The identification may be used while studying population genetics.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5080 Alpha-1-antichymotrypsin immunological test system.
|
|
(a) Identification. An alpha -1-antichymotrypsin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques alpha -1-antichymotrypsin (a protein) in serum, other body fluids, and tissues. Alpha -1-antichymotrypsin helps protect tissues against proteolytic (protein-splitting) enzymes released during infection.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5090 Antimitochondrial antibody immunological test system.
|
|
(a) Identification. An antimitochondrial antibody immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the antimitochondrial antibodies in human serum. The measurements aid in the diagnosis of diseases that produce a spectrum of autoantibodies (antibodies produced against the body's own tissue), such as primary biliary cirrhosis (degeneration of liver tissue) and chronic active hepatitis (inflammation of the liver).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5100 Antinuclear antibody immunological test system.
|
|
(a) Identification. An antinuclear antibody immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the autoimmune antibodies in serum, other body fluids, and tissues that react with cellular nuclear constituents (molecules present in the nucleus of a cell, such as ribonucleic acid, deoxyribonucleic acid, or nuclear proteins). The measurements aid in the diagnosis of systemic lupus erythematosus (a multisystem autoimmune disease in which antibodies attack the victim's own tissues), hepatitis (a liver disease), rheumatoid arthritis, Sjogren's syndrome (arthritis with inflammation of the eye, eyelid, and salivary glands), and systemic sclerosis (chronic hardening and shrinking of many body tissues).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5110 Antiparietal antibody immunological test system.
|
|
(a) Identification. An antiparietal antibody immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the specific antibody for gastric parietal cells in serum and other body fluids. Gastric parietal cells are those cells located in the stomach that produce a protein that enables vitamin B12 to be absorbed by the body. The measurements aid in the diagnosis of vitamin B12 deficiency (or pernicious anemia), atrophic gastritis (inflammation of the stomach), and autoimmune connective tissue diseases (diseases resulting when the body produces antibodies against its own tissues).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5120 Antismooth muscle antibody immunological test system.
|
|
(a) Identification. An antismooth muscle antibody immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the antismooth muscle antibodies (antibodies to nonstriated, involuntary muscle) in serum. The measurements aid in the diagnosis of chronic hepatitis (inflammation of the liver) and autoimmune connective tissue diseases (diseases resulting from antibodies produced against the body's own tissues).
(b) Classification Class II (performance standards).
|
|
|
Sec. 866.5130 Alpha-1-antitrypsin immunological test system.
|
|
(a) Identification. An alpha -1-antitrypsin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the alpha -1-antitrypsin (a plasma protein) in serum, other body fluids, and tissues. The measurements aid in the diagnosis of several conditions including juvenile and adult cirrhosis of the liver. In addition, alpha -1-antitrypsin deficiency has been associated with pulmonary emphysema.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5150 Bence-Jones proteins immunological test system.
|
|
(a) Identification. A Bence-Jones proteins immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the Bence-Jones proteins in urine and plasma. Immunoglobulin molecules normally consist of pairs of polypeptide chains (subunits) of unequal size (light chains and heavy chains) bound together by several disulfide bridges. In some cancerous conditions, there is a proliferation of one plasma cell (antibody-producing cell) with excess production of light chains of one specific kind (monoclonal light chains). These free homogeneous light chains not associated with an immunoglobulin molecule can be found in urine and plasma, and have been called Bence-Jones proteins. Measurement of Bence-Jones proteins and determination that they are monoclonal aid in the diagnosis of multiple myeloma (malignant proliferation of plasma cells), Waldenstrom's macroglobulinemia (increased production of large immunoglobulins by spleen and bone marrow cells), leukemia (cancer of the blood-forming organs), and lymphoma (cancer of the lymphoid tissue).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5160 Beta-globulin immunological test system.
|
|
(a) Identification. A beta -globulin immunological test system is a device that consists of reagents used to measure by immunochemical techniques beta globulins (serum protein) in serum and other body fluids. Beta -globulin proteins include beta -lipoprotein, transferrin, glycoproteins, and complement, and are rarely associated with specific pathologic disorders.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5170 Breast milk immunological test system.
|
|
(a) Identification. A breast milk immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the breast milk proteins.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 59 FR 63007, Dec. 7, 1994; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5180 Fecal calprotectin immunological test system.
|
|
(a) Identification. A fecal calprotectin immunological test system is an in vitro diagnostic device that consists of reagents used to quantitatively measure, by immunochemical techniques, fecal calprotectin in human stool specimens. The device is intended forin vitro diagnostic use as an aid in the diagnosis of inflammatory bowel diseases (IBD), specifically Crohn's disease and ulcerative colitis, and as an aid in differentiation of IBD from irritable bowel syndrome.
(b) Classification. Class II (special controls). The special control for these devices is FDA's guidance document entitled "Class II Special Controls Guidance Document: Fecal Calprotectin Immunological Test Systems." For the availability of this guidance document, see § 866.1(e).
[71 FR 42598, July 27, 2006]
|
|
|
Sec. 866.5200 Carbonic anhydrase B and C immunological test system.
|
|
(a) Identification. A carbonic anhydrase B and C immunological test system is a device that consists of the reagents used to measure by immunochemical techniques specific carbonic anhydrase protein molecules in serum and other body fluids. Measurements of carbonic anhydrase B and C aid in the diagnosis of abnormal hemoglobin metabolism.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5210 Ceruloplasmin immunological test system.
|
|
(a) Identification. A ceruloplasmin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the ceruloplasmin (copper-transporting serum protein) in serum, other body fluids, or tissues. Measurements of ceruloplasmin aid in the diagnosis of copper metabolism disorders.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 84 FR 71800, Dec. 30, 2019]
|
|
|
Sec. 866.5220 Cohn fraction II immunological test system.
|
|
(a) Identification. A Cohn fraction II immunological test system is a device that consists of the reagents that contain or are used to measure that fraction of plasma containing protein gamma globulins, predominantly of the IgG class. The device may be used as a coprecipitant in radioimmunoassay methods, as raw material for the purification of IgG subclasses, and to reduce nonspecific adsorption of plasma proteins in immunoassay techniques. Measurement of these proteins aids in the diagnosis of any disease concerned with abnormal levels of IgG gamma globulins such as agammaglobulinemia or multiple myeloma.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 59 FR 63007, Dec. 7, 1994; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5230 Colostrum immunological test system.
|
|
(a) Identification. A colostrum immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the specific proteins in colostrum. Colostrum is a substance excreted by the mammary glands during pregnancy and until production of breast milk begins 1 to 5 days after childbirth.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 59 FR 63007, Dec. 7, 1994; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5240 Complement components immunological test system.
|
|
(a) Identification. A complement components immunological test system is a device that consists of the reagents used to measure by immunochemical techniques complement components C1q, C1r, C1s, C2, C3, C4, C5, C6, C7, C8, and C9, in serum, other body fluids, and tissues. Complement is a group of serum proteins which destroy infectious agents. Measurements of these proteins aids in the diagnosis of immunologic disorders, especially those associated with deficiencies of complement components.
(b) Classification. Class II (performance standards).
[47 FR 50823, Nov. 9, 1982, as amended at 53 FR 11253, Apr. 6, 1988]
|
|
|
Sec. 866.5250 Complement C1 inhibitor (inactivator) immunological test system.
|
|
(a) Identification. A complement C1 inhibitor (inactivator) immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the complement C1 inhibitor (a plasma protein) in serum. Complement C1 inhibitor occurs normally in plasma and blocks the action of the C1 component of complement (a group of serum proteins which destroy infectious agents). Measurement of complement C1 inhibitor aids in the diagnosis of hereditary angioneurotic edema (increased blood vessel permeability causing swelling of tissues) and a rare form of angioedema associated with lymphoma (lymph node cancer).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5260 Complement C3b inactivator immunological test system.
|
|
(a) Identification. A complement C3b inactivator immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the complement C3b inactivator (a plasma protein) in serum. Complement is a group of serum proteins that destroy infectious agents. Measurement of complement C3b inactivator aids in the diagnosis of inherited antibody dysfunction.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5270 C-reactive protein immunological test system.
|
|
(a) Identification. A C-reactive protein immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the C-reactive protein in serum and other body fluids. Measurement of C-reactive protein aids in evaluation of the amount of injury to body tissues.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5320 Properdin factor B immunological test system.
|
|
(a) Identification. A properdin factor B immunological test system is a device that consists of the reagents used to measure by immunochemical techniques properdin factor B in serum and other body fluids. The deposition of properdin factor B in body tissues or a corresponding depression in the amount of properdin factor B in serum and other body fluids is evidence of the involvement of the alternative to the classical pathway of activation of complement (a group of plasma proteins which cause the destruction of cells which are foreign to the body). Measurement of properdin factor B aids in the diagnosis of several kidney diseases, e.g., chronic glomerulonephritis (inflammation of the glomeruli of the kidney), lupus nephritis (kidney disease associated with a multisystem autoimmune disease, systemic lupus erythematosus), as well as several skin diseases, e.g., dermititis herpetiformis (presence of vesicles on the skin that burn and itch), and pemphigus vulgaris (large vesicles on the skin). Other diseases in which the alternate pathway of complement activation has been implicated include rheumatoid arthritis, sickle cell anemia, and gram-negative bacteremia.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.5330 Factor XIII, A, S, immunological test system.
|
|
(a) Identification. A factor XIII, A, S, immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the factor XIII (a bloodclotting factor), in platelets (A) or serum (S). Measurements of factor XIII, A, S, aid in the diagnosis and treatment of certain bleeding disorders resulting from a deficiency of this factor.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9. This exemption does not apply to factor deficiency tests classified under § 864.7290 of this chapter.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5340 Ferritin immunological test system.
|
|
(a) Identification. A ferritin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the ferritin (an iron-storing protein) in serum and other body fluids. Measurements of ferritin aid in the diagnosis of diseases affecting iron metabolism, such as hemochromatosis (iron overload) and iron deficiency amemia.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5350 Fibrinopeptide A immunological test system.
|
|
(a) Identification. A fibrinopeptide A immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the fibrinopeptide A (a blood-clotting factor) in plasma and other body fluids. Measurement of fibrinopeptide A may aid in the diagnosis and treatment of certain blood-clotting disorders.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5360 Cohn fraction IV immunological test system.
|
|
(a) Identification. A Cohn fraction IV immunological test system is a device that consists of or measures that fraction of plasma proteins, predominantly alpha- and beta- globulins, used as a raw material for the production of pure alpha- or beta- globulins. Measurement of specific alpha- or beta- globulins aids in the diagnosis of many diseases, such as Wilson's disease (an inherited disease affecting the liver and brain), Tangier's disease (absence of alpha- 1-lipoprotein), malnutrition, iron deficiency anemia, red blood cell disorders, and kidney disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982; 47 FR 56846, Dec. 21, 1982, as amended at 59 FR 63007, Dec. 7, 1994; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5370 Cohn fraction V immunological test system.
|
|
(a) Identification. A Cohn fraction V immunological test system is a device that consists of or measures that fraction of plasma containing predominantly albumin (a plasma protein). This test aids in the diagnosis of diseases where albumin levels may be depressed, e.g., nephrosis (disease of the kidney), proteinuria (protein in the urine), gastroenteropathy (disease of the stomach and small intestine), rheumatoid arthritis, and viral hepatitis.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 59 FR 63007, Dec. 7, 1994; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5380 Free secretory component immunological test system.
|
|
(a) Identification. A free secretory component immunological test system is a device that consists of the reagents used to measure by immunochemical techniques free secretory component (normally a portion of the secretory IgA antibody molecule) in body fluids. Measurement of free secretory component (protein molecules) aids in the diagnosis or repetitive lung infections and other hypogammaglobulinemic conditions (low antibody levels).
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.5400 Alpha-globulin immunological test system.
|
|
(a) Identification. An alpha- globulin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the alpha- globulin (a serum protein) in serum and other body fluids. Measurement of alpha- globulin may aid in the diagnosis of inflammatory lesions, infections, severe burns, and a variety of other conditions.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5420 Alpha-1-glycoproteins immunological test system.
|
|
(a) Identification. An alpha- 1-glycoproteins immunological test system is a device that consists of the reagents used to measure by immunochemical techniques alpha- 1-glycoproteins (a group of plasma proteins found in the alpha- 1 group when subjected to electrophoresis) in serum and other body fluids. Measurement of specific alpha- 1-glycoproteins may aid in the diagnosis of collagen (connective tissue) disorders, tuberculosis, infections, extensive malignancy, and diabetes.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5425 Alpha-2-glycoproteins immunological test system.
|
|
(a) Identification. An alpha -2-glycoproteins immunolgical test system is a device that consists of the reagents used to measure by immunochemical techniques the alpha -2-glycoproteins (a group of plasma proteins found in the alpha- 2 group when subjected to electrophoresis) in serum and other body fluids. Measurement of alpha -2-glycoproteins aids in the diagnosis of some cancers and genetically inherited deficiencies of these plasma proteins.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5430 Beta-2-glycoprotein I immunological test system.
|
|
(a) Identification. A beta -2-glycoprotein I immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the beta -2-glycoprotein I (a serum protein) in serum and other body fluids. Measurement of beta -2-glycoprotein I aids in the diagnosis of an inherited deficiency of this serum protein.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5440 Beta-2-glycoprotein III immunological test system.
|
|
(a) Identification. A beta -2-glycoprotein III immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the beta -2-glycoprotein III (a serum protein) in serum and other body fluids. Measurement of beta -2-glycoprotein III aids in the diagnosis of an inherited deficiency of this serum protein and a variety of other conditions.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5460 Haptoglobin immunological test system.
|
|
(a) Identification. A haptoglobin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the haptoglobin (a protein that binds hemoglobin, the oxygen-carrying pigment in red blood cells) in serum. Measurement of haptoglobin may aid in the diagnosis of hemolytic diseases (diseases in which the red blood cells rupture and release hemoglobin) related to the formation of hemoglobin-haptoglobin complexes and certain kidney diseases.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.5470 Hemoglobin immunological test system.
|
|
(a) Indentification. A hemoglobin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the different types of free hemoglobin (the oxygen-carrying pigment in red blood cells) in blood, urine, plasma, or other body fluids. Measurements of free hemoglobin aid in the diagnosis of various hematologic disorders, such as sickle cell anemia, Fanconi's anemia (a rare inherited disease), aplastic anemia (bone marrow does not produce enough blood cells), and leukemia (cancer of the blood-forming organs).
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 84 FR 71800, Dec. 30, 2019]
|
|
|
Sec. 866.5490 Hemopexin immunological test system.
|
|
(a) Indentification. A hemopexin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the hemopexin (a serum protein that binds heme, a component of hemoglobin) in serum. Measurement of hemopexin aids in the diagnosis of various hematologic disorders, such as hemolytic anemia (anemia due to shortened in vivo survival of mature red blood cells and inability of the bone marrow to compensate for their decreased life span) and sickle cell anemia.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 63 FR 59227, Nov. 3, 1998]
|
|
|
Sec. 866.5500 Hypersensitivity pneumonitis immunological test system.
|
|
(a) Identification. A hypersensitivity pneumonitis immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the immunoglobulin antibodies in serum which react specifically with organic dust derived from fungal or animal protein sources. When these antibodies react with such dusts in the lung, immune complexes precipitate and trigger an inflammatory reaction (hypersensitivity pneumonitis). Measurement of these immunoglobulin G antibodies aids in the diagnosis of hypersensitivity pneumonitis and other allergic respiratory disorders.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5510 Immunoglobulins A, G, M, D, and E immunological test system.
|
|
(a) Identification. An immunoglobulins A, G, M, D, and E immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the immunoglobulins A, G, M, D, an E (serum antibodies) in serum. Measurement of these immunoglobulins aids in the diagnosis of abnormal protein metabolism and the body's lack of ability to resist infectious agents.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5520 Immunoglobulin G (Fab fragment specific) immunological test system.
|
|
(a) Identification. An immunoglobulin G (Fab fragment specific) immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the Fab antigen-binding fragment resulting from breakdown of immunoglobulin G antibodies in urine, serum, and other body fluids. Measurement of Fab fragments of immunoglobulin G aids in the diagnosis of lymphoproliferative disorders, such as multiple myeloma (tumor of bone marrow cells), Waldenstrom's macroglobulinemia (increased immunoglobulin production by the spleen and bone marrow cells), and lymphoma (tumor of the lymphoid tissues).
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 61 FR 1119, Jan. 16, 1996; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5530 Immunoglobulin G (Fc fragment specific) immunological test system.
|
|
(a) Identification. An immunoglobulin G (Fc fragment specific) immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the Fc (carbohydrate containing) fragment of immunoglobulin G (resulting from breakdown of immunoglobulin G antibodies) in urine, serum, and other body fluids. Measurement of immunoglobulin G Fc fragments aids in the diagnosis of plasma cell antibody-forming abnormalities, e.g., gamma heavy chain disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 61 FR 1119, Jan. 16, 1996; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5540 Immunoglobulin G (Fd fragment specific) immunological test system.
|
|
(a) Identification. An immunoglobulin G (Fd fragment specific) immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the amino terminal (antigen-binding) end (Fd fragment) of the heavy chain (a subunit) of the immunoglobulin antibody molecule in serum. Measurement of immunoglobulin G Fd fragments aids in the diagnosis of plasma antibody-forming cell abnormalities.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 59 FR 63007, Dec. 7, 1994; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5550 Immunoglobulin (light chain specific) immunological test system.
|
|
(a) Identification. An immunoglobulin (light chain specific) immunological test system is a device that consists of the reagents used to measure by immunochemical techniques both kappa and lambda types of light chain portions of immunoglobulin molecules in serum, other body fluids, and tissues. In some disease states, an excess of light chains are produced by the antibody-forming cells. These free light chains, unassociated with gamma globulin molecules, can be found in a patient's body fluids and tissues. Measurement of the various amounts of the different types of light chains aids in the diagnosis of multiple myeloma (cancer of antibody-forming cells), lymphocytic neoplasms (cancer of lymphoid tissue), Waldenstrom's macroglobulinemia (increased production of large immunoglobulins), and connective tissue diseases such as rheumatoid arthritis or systemic lupus erythematosus.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5560 Lactic dehydrogenase immunological test system.
|
|
(a) Identification. A lactic dehydrogenase immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the activity of the lactic dehydrogenase enzyme in serum. Increased levels of lactic dehydrogenase are found in a variety of conditions, including megaloblastic anemia (decrease in the number of mature red blood cells), myocardial infarction (heart disease), and some forms of leukemia (cancer of the blood-forming organs). However, the diagnostic usefulness of this device is limited because of the many conditions known to cause increased lactic dehydrogenase levels.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5570 Lactoferrin immunological test system.
|
|
(a) Identification. A lactoferrin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the lactoferrin (an iron-binding protein with the ability to inhibit the growth of bacteria) in serum, breast milk, other body fluids, and tissues. Measurement of lactoferrin may aid in the diagnosis of an inherited deficiency of this protein.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2312, Jan. 14, 2000]
|
|
|
Sec. 866.5580 Alpha-1-lipoprotein immunological test system.
|
|
(a) Identification. An alpha -1-lipoprotein immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the alpha- 1-lipoprotein (high-density lipoprotein) in serum and plasma. Measurement of alpha- 1-lipoprotein may aid in the diagnosis of Tangier disease (a hereditary disorder of fat metabolism).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5590 Lipoprotein X immunological test system.
|
|
(a) Identification. A lipoprotein X immunological test system is a device that consists of the reagents used to measure by immunochemical techniques lipoprotein X (a high-density lipoprotein) in serum and other body fluids. Measurement of lipoprotein X aids in the diagnosis of obstructive liver disease.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2313, Jan. 14, 2000]
|
|
|
Sec. 866.5600 Low-density lipoprotein immunological test system.
|
|
(a) Identification. A low-density lipoprotein immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the low-density lipoprotein in serum and other body fluids. Measurement of low-density lipoprotein in serum may aid in the diagnosis of disorders of lipid (fat) metabolism and help to identify young persons at risk from cardiovascular diseases.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5620 Alpha-2-macroglobulin immunological test system.
|
|
(a) Identification. An alpha -2-macroglobulin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the alpha -2-macroglobulin (a serum protein) in plasma. Measurement of alpha -2-macroglobulin may aid in the diagnosis of blood-clotting or clot lysis disorders.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 84 FR 71800, Dec. 30, 2019]
|
|
|
Sec. 866.5630 Beta-2-microglobulin immunological test system.
|
|
(a) Identification. A beta -2-microglobulin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques beta -2-microglobulin (a protein molecule) in serum, urine, and other body fluids. Measurement of beta -2-microglobulin aids in the diagnosis of active rheumatoid arthritis and kidney disease.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 84 FR 71800, Dec. 30, 2019]
|
|
|
Sec. 866.5640 Infectious mononucleosis immunological test system.
|
|
(a) Identification. An infectious mononucleosis immunological test system is a device that consists of the reagents used to measure by immunochemical techniques heterophile antibodies frequently associated with infectious mononucleosis in serum, plasma, and other body fluids. Measurements of these antibodies aid in the diagnosis of infectious mononucleosis.
(b) Classification. Class II (performance standards).
[47 FR 50823, Nov. 9, 1982; 47 FR 56846, Dec. 21, 1982]
|
|
|
Sec. 866.5660 Multiple autoantibodies immunological test system.
|
|
(a) Identification. A multiple autoantibodies immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the autoantibodies (antibodies produced against the body's own tissues) in serum and other body fluids. Measurement of multiple autoantibodies aids in the diagnosis of autoimmune disorders (disease produced when the body's own tissues are injured by autoantibodies).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5665 Aquaporin-4 autoantibody immunological test system.
|
|
(a) Identification. An Aquaporin-4 autoantibody immunological test system is a device that consists of reagents used to measure by immunochemical techniques autoantibodies in human serum samples that react with Aquaporin-4 (AQP4Ab). The measurements aid in the diagnosis of neuromyelitis optica (NMO) and neuromyelitis optica spectrum disorders (NMOSD) in conjunction with other clinical, laboratory, and radiological (e.g., magnetic resonance imaging) findings.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include the following information:
(i) A detailed device description including:
(A) A detailed description of all components including all required ancillary reagents in the test;
(B) If applicable, a detailed description of instrumentation and equipment, including illustrations or photographs of non-standard equipment or manuals;
(C) If applicable, detailed documentation of the device software, including, but not limited to, standalone software applications and hardware-based devices that incorporate software;
(D) A detailed description of appropriate internal and external quality controls that are recommended or provided. The description must identify those control elements that are incorporated into the specified testing procedures;
(E) Detailed specifications for sample collection, processing, and storage;
(F) A detailed description of methodology and assay procedure;
(G) A description of how the assay cutoff (the medical decision point between positive and negative) was established and validated as well as supporting data; and
(H) Detailed specification of the criteria for test results interpretation and reporting.
(ii) Detailed information demonstrating the performance characteristics of the device, including:
(A) Device precision/reproducibility data generated from within-run, between-run, between-day, between-lot, between-site, and total precision for multiple nonconsecutive days, as applicable. A well characterized panel of patient samples or pools from the indicated population that covers the device measuring range must be used.
(B) Device linearity data generated from samples covering the device measuring range, if applicable.
(C) Information on traceability to a reference material and description of value assignment of calibrators and controls, if applicable.
(D) Device analytical sensitivity data, including limit of blank, limit of detection, and limit of quantitation, if applicable.
(E) Device analytical specificity data, including interference by endogenous and exogenous substances, as well as cross-reactivity with samples derived from patients with other autoimmune diseases or conditions.
(F) Device instrument carryover data, when applicable.
(G) Device stability data, including real-time stability under various storage times and temperatures.
(H) Specimen stability data, including stability under various storage times, temperatures, freeze-thaw, and transport conditions, where appropriate.
(I) Method comparison data generated by comparison of the results obtained with the device to those obtained with a legally marketed predicate device with similar indications of use. A well-characterized panel of patient samples from the indicated population covering the device measuring range must be used.
(J) Specimen matrix comparison data, if more than one specimen type or anticoagulant can be tested with the device. Samples used for comparison must be from well-characterized patient samples covering the device measuring range.
(K) Clinical performance must be established by comparing data generated by testing samples from the indicated population and the differential diagnosis or non-target disease groups with the device to the clinical diagnostic standard.
(1 ) The diagnosis of NMO and NMOSD must be based on clinical findings, laboratory tests (e.g., serological tests), and radiological tests (e.g., magnetic resonance imaging).
(2 ) The differential diagnosis or non-target disease group must include the applicable diseases or conditions, including but not be limited to the following: Multiple sclerosis, stroke, Lyme disease, shingles, syphilis, human immunodeficiency virus, hepatitis B, tuberculosis, Srgen's syndrome, systemic lupus erythematous, systemic vasculitis, sarcoidosis, Graves' disease, Hashimoto's disease, Type I diabetes, rheumatoid arthritis, Addison's disease, and myasthenia gravis.
(3 ) Diagnosis of diseases or conditions for the differential or non-target disease groups must be based on established diagnostic criteria and clinical evaluation.
(4 ) For all samples, the diagnostic clinical criteria and the demographic information must be collected and provided.
(5 ) The clinical validation results must demonstrate clinical sensitivity and clinical specificity for the test values based on the presence or absence of NMO and NMOSD.
(6 ) The data must be summarized in tabular format comparing the interpretation of results to the disease status.
(L) Expected/reference values generated by testing an adequate number of samples from apparently healthy normal individuals.
(iii) Identification of risk mitigation elements used by the device, including description of all additional procedures, methods, and practices incorporated into the directions for use that mitigate risks associated with testing.
(2) The device's 21 CFR 809.10(b) compliant labeling must include warnings relevant to the device including:
(i) A warning statement that reads "The device is for use by laboratory professionals in a clinical laboratory setting"; and
(ii) A warning statement that reads "The device is not to be used as a stand-alone device but as an adjunct to other clinical information. A diagnosis of Neuromyelitis Optica (NMO) and Neuromyelitis Optica Spectrum Disorders (NMOSD) should not be made on a single test result. The clinical symptoms, results from physical examination, laboratory tests (e.g., serological tests), and radiological tests (e.g. Magnetic Resonance Imaging), when appropriate, should always be taken into account when considering the diagnosis of NMO and NMOSD."
(3) The device's 21 CFR 809.10(b) compliant labeling must include a detailed description of the protocol and performance studies performed in accordance with paragraph (b)(1)(ii) of this section and a summary of the results.
[82 FR 50076, Oct. 30, 2017]
|
|
|
Sec. 866.5670 Zinc transporter 8 autoantibody immunological test system.
|
|
(a) Identification. A zinc transporter 8 autoantibody immunological test system is a device that consists of reagents used to measure, by immunochemical techniques, the autoantibodies in human serum samples that react with Zinc Transporter 8 (ZnT8). The measurements aid in the diagnosis of Type 1 diabetes mellitus (autoimmune mediated diabetes) in conjunction with other clinical and laboratory findings.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include the following information:
(i) A detailed description of the device that includes:
(A) A detailed description of all components in the test system, including a description of the assay components in the kit and all required ancillary reagents;
(B) A detailed description of instrumentation and equipment, and illustrations or photographs of non-standard equipment or methods if applicable;
(C) Detailed documentation of the device software, including, but not limited to, standalone software applications and hardware-based devices that incorporate software where applicable;
(D) A detailed description of appropriate internal and external quality controls that are recommended or provided. The description must identify those control elements that are incorporated into the recommended testing procedures;
(E) Detailed specifications for sample collection, processing, and storage;
(F) A detailed description of methodology and assay procedure; and
(G) Detailed specification of the criteria for test results interpretation and reporting.
(ii) Information that demonstrates the performance characteristics of the device, including:
(A) Device precision/reproducibility data generated from within-run, between-run, between-day, between-lot, between-operator, between-instruments, between-site, and total precision for multiple nonconsecutive days as applicable. A well characterized panel of patient samples or pools from the intended use population that covers the device measuring range must be used;
(B) Device linearity data generated from patient samples covering the assay measuring range if applicable;
(C) Information on traceability to a reference material and description of value assignment of calibrators and controls if applicable;
(D) Device analytical sensitivity data, including limit of blank, limit of detection and limit of quantitation if applicable;
(E) Device analytical specificity data, including interference by endogenous and exogenous substances, as well as cross-reactivity with samples derived from patients with other autoimmune diseases or conditions;
(F) Device instrument carryover data when applicable;
(G) Device stability data including real-time stability under various storage times and temperatures;
(H) Specimen stability data, including stability under various storage times, temperatures, freeze-thaw, and transport conditions where appropriate;
(I) Method comparison data generated by comparison of the results obtained with the device to those obtained with a legally marketed predicate device with similar indication of use. Patient samples from the intended use population covering the device measuring range must be used;
(J) Specimen matrix comparison data if more than one specimen type or anticoagulant can be tested with the device. Samples used for comparison must be from patient samples covering the device measuring range;
(K) A description of how the assay cut-off (the medical decision point between positive and negative) was established and validated as well as supporting data;
(L) Clinical performance must be established by comparing data generated by testing samples from the intended use population and the differential diagnosis groups with the device to the clinical diagnostic standard. The diagnosis of Type 1 diabetes mellitus must be based on clinical history, physical examination, and laboratory tests, such as one or more pancreatic or insulin autoantibody test. Because the intended use population for Type 1 diabetes mellitus includes subjects less than 18 years old, samples from representative numbers of these subjects must be included. Representative numbers of samples from all age strata must also be included. The differential diagnosis groups must include, but not be limited to the following: Type 2 diabetes mellitus; metabolic syndrome; latent autoimmune diabetes in adults; other autoimmune diseases such as celiac disease (without a concomitant diagnosis of Type 1 diabetes mellitus), systemic lupus erythematosus, rheumatoid arthritis, and Hashimoto's thyroiditis; infection; renal disease; and testicular cancer. Diseases for the differential groups must be based on established diagnostic criteria and clinical evaluation. For all samples, the diagnostic clinical criteria and the demographic information must be collected and provided. The clinical validation results must demonstrate clinical sensitivity and clinical specificity for the test values based on the presence or absence of Type 1 diabetes mellitus. The data must be summarized in tabular format comparing the interpretation of results to the disease status; and
(M) Expected/reference values generated by testing an adequate number of samples from apparently healthy normal individuals.
(iii) Identification of risk mitigation elements used by the device, including description of all additional procedures, methods, and practices incorporated into the directions for use that mitigate risks associated with testing.
(2) Your 21 CFR 809.10(a) compliant label and 21 CFR 809.10(b) compliant labeling must include warnings relevant to the assay including:
(i) A warning statement that reads, "The device is for use by laboratory professionals in a clinical laboratory setting";
(ii) A warning statement that reads, "The test is not a stand-alone test but an adjunct to other clinical information. A diagnosis of Type 1 diabetes mellitus should not be made on a single test result. The clinical symptoms, results on physical examination, and laboratory tests (e.g., serological tests), when appropriate, should always be taken into account when considering the diagnosis of Type 1 diabetes mellitus and Type 2 diabetes mellitus";
(iii) A warning statement that reads, "Absence of Zinc T8 autoantibody does not rule out a diagnosis of Type 1 diabetes mellitus"; and
(iv) A warning statement that reads, "The assay has not been demonstrated to be effective for monitoring the stage of disease or its response to treatment."
(3) Your 21 CFR 809.10(b) compliant labeling must include a description of the protocol and performance studies performed in accordance with paragraph (b)(1)(ii) of this section and a summary of the results.
[82 FR 49103, Oct. 20, 2017]
|
|
|
Sec. 866.5680 Myoglobin immunological test system.
|
|
(a) Identification. A myoglobin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the myoglobin (an oxygen storage protein found in muscle) in serum and other body fluids. Measurement of myoglobin aids in the rapid diagnosis of heart or renal disease.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5700 Whole human plasma or serum immunological test system.
|
|
(a) Identification. A whole human plasma or serum immunological test system is a device that consists of reagents used to measure by immunochemical techniques the proteins in plasma or serum. Measurements of proteins in plasma or serum aid in the diagnosis of any disease concerned with abnormal levels of plasma or serum proteins, e.g., agammaglobulinemia, allergies, multiple myeloma, rheumatoid vasculitis, or hereditary angioneurotic edema.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 59 FR 63007, Dec. 7, 1994; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5715 Plasminogen immunological test system.
|
|
(a) Identification. A plasminogen immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the plasminogen (an inactive substance from which plasmin, a blood-clotting factor, is formed) in serum, other body fluids, and tissues. Measurement of plasminogen levels may aid in the diagnosis of fibrinolytic (blood-clotting) disorders.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2313, Jan. 14, 2000]
|
|
|
Sec. 866.5735 Prothrombin immunological test system.
|
|
(a) Identification. A prothrombin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the prothrombin (clotting factor II) in serum. Measurements of the amount of antigenically competent (ability to react with protein antibodies) prothrombin aid in the diagnosis of blood-clotting disorders.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9. This exemption does not apply to multipurpose systems for in vitro coagulation studies classified under § 864.5425 of this chapter or prothrombin time tests classified under § 864.7750 of this chapter.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2313, Jan. 14, 2000]
|
|
|
Sec. 866.5750 Radioallergosorbent (RAST) immunological test system.
|
|
(a) Identification. A radioallergosorbent immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the allergen antibodies (antibodies which cause an allergic reaction) specific for a given allergen. Measurement of specific allergen antibodies may aid in the diagnosis of asthma, allergies, and other pulmonary disorders.
(b) Classification. Class II (special controls). The device, when intended to detect any of the allergens included in Table 1 in this paragraph, is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
Table 1 - Class II Exempt Allergens Under § 866.5750 - Radioallergosorbent (RAST) Immunological Test Systems
| Allergen code
| Allergen product
| Source
(taxonomical name)
|
|---|
| Grass Pollens
| | g1 | Sweet vernal grass | Anthoxanthum odoratum.
| | g3 | Cocksfoot grass, Orchard grass | Dactylis glomerata.
| | g4 | Meadow fescue | Festuca elatior.
| | g5 | Rye-grass (perennial rye grass) | Lolium perenne.
| | g7 | Common reed (common reed grass) | Phragmites communis.
| | g8 | Meadow grass, Kentucky blue (June grass) | Poa pratensis.
| | g9 | Redtop, Bentgrass | Agrostis stolonifera, Agrostis gigantea (Agrostis alba).
| | g11 | Brome grass | Bromus inermis.
| | g12 | Cultivated rye (cultivated rye grass) | Secale cereale.
| | g13 | Velvet grass | Holcus lanatus.
| | g14 | Cultivated oat (cultivated oat grass) | Avena sativa.
| | g15 | Cultivated wheat (cultivated wheat grass) | Triticum aestivum (Triticum spp.).
| | g16 | Meadow foxtail (meadow foxtail grass) | Alopecurus pratensis.
| | g17 | Bahia grass | Paspalum notatum.
| | g24 | Wheat grass, Western | Agropyron smithii (Elymus smithii).
| | g30 | Bluegrass, annual | Poa annua.
| | g70 | Wild rye grass | Elymus triticoides Elymus condensatus.
| | g71 | Canary grass | Phalaris arundinacea.
| | g201 | Barley, cultivated | Hordeum vulgare.
| | g202 | Maize, corn (cultivated corn) | Zea mays.
| | g203 | Salt grass | Distichlis spicata.
| | g204 | False oat-grass | Arrhenatherum elatius.
| | g216 | Cyn d 1 | Cynodon dactylon.
| | g701 | Phl p 1.0102, Phl p 5.0101 | Phleum pratense.
| | g702 | Phl p 7.0101 | Phleum pratense.
| | g703 | Phl p 12.0101 | Phleum pratense.
| | Weed Pollens
| | w2 | Western ragweed | Ambrosia psilostachya.
| | w4 | False ragweed | Ambrosia acanthicarpa (Franseria acanthicarpa).
| | w5 | Wormwood | Artemisia absinthium Artemisia annua.
| | w6 | Mugwort | Artemisia vulgaris.
| | w7 | Marguerite, ox-eye daisy | Chrysanthemum leucanthemum.
| | w8 | Dandelion | Taraxacum vulgare, Taraxacum officinale.
| | w9 | Plantain (English), Ribwort | Plantago lanceolata.
| | w10 | Goosefoot, lamb's quarters | Chenopodium album.
| | w11 | Saltwort (prickly), Russian thistle | Salsola kali (Salsola pestifer).
| | w12 | Goldenrod | Solidago virgaurea (Solidago spp.).
| | w13 | Cocklebur, common | Xanthium commune.
| | w14 | Common pigweed (rough pigweed) | Amaranthus retroflexus.
| | w15 | Scale, Lenscale | Atriplex lentiformis.
| | w16 | Rough marsh elder | Iva ciliate, Iva annua.
| | w17 | Firebush (Kochia) | Kochia scoparia.
| | w18 | Sheep sorrel | Rumex acetosella.
| | w19 | Wall pellitory | Parietaria officinalis.
| | w20 | Nettle (Common stinging nettle) | Urtica dioica.
| | w21 | Wall pellitory | Parietaria judaica.
| | w22 | Japanese hop (careless weed) | Humulus japonicas (Humulus scandens).
| | w23 | Yellow dock, Yellow dockweed | Rumex crispus.
| | w24 | Spiny pigweed | Amaranthus spinosus.
| | w27 | Carnation | Dianthus spp.
| | w28 | Rose | Rosa rugosa.
| | w33 | Clover | Trifolium pratense.
| | w35 | Mexican tea | Chenopodium ambrosioides.
| | w36 | Rabbit bush | Ambrosia deltoidea (Franseria deltoides).
| | w37 | Salt bush, annual | Atriplex wrightii.
| | w39 | Water hemp, Western | Amaranthus rudis (Acnida tamariscina).
| | w41 | Burrobrush | Hymenoclea salsola.
| | w42 | Poverty weed | Baccharis neglecta.
| | w43 | Common sagebrush | Artemisia tridentata.
| | w45 | Alfalfa | Medicago sativa.
| | w46 | Dog fennel | Eupatorium capillifolium.
| | w53 | Geranium | Geranium spp.
| | w67 | Groundsel bush | Baccharis halimifolia.
| | w69 | Iodine bush | Allenrolfea occidentalis.
| | w70 | Ragweed, slender | Ambrosia confertiflora.
| | w75 | Wing scale (wingscale) | Atriplex canescens.
| | w82 | Careless weed | Amaranthus palmeri, Amaranthus hybridus.
| | w90 | Japanese hop | Humulus japonicas (Humulus scandens).
| | w203 | Rape (rape pollen) | Brassica napus.
| | w204 | Sunflower | Helianthus annuus.
| | w206 | Camomile | Matricaria chamomilla.
| | w207 | Lupin | Lupinus spp.
| | w210 | Sugar-beet | Beta vulgaris.
| | w211 | Par j 2.0101 | Parietaria judaica.
| | w231 | Art v 1 | Artemisia vulgaris (Mugwort).
| | w232 | Sal k 1 | Salsola kali.
| | w233 | Art v 3 | Artemisa vulgaris (LTP, Mugwort).
| | w234 | Pla l 1 | Plantago lanceolata.
| | w235 | Che a 1.0101 | Chenopodium album.
| | w236 | Mer a 1.0101 | Mercurialis annua.
| | a753 | Art v 1 | Artemisia vulgaris (Mugwort weed).
| | Tree Pollens
| | t1 | Box-elder (Maple) | Acer negundo, Acer saccharum.
| | t2 | Gray alder, speckled alder (alder) | Alnus incana.
| | t4 | Hazel, hazelnut | Corylus avellana, Corylus americana.
| | t5 | American beech (beech) | Fagus grandifolia (Fagus americana).
| | t6 | Mountain juniper, Mountain cedar | Juniperus ashei (Juniperus sabinoides).
| | t8 | Elm | Ulmus americana.
| | t9 | Olive | Olea europaea.
| | t10 | Walnut | Juglans californica, Juglans nigra.
| | t11 | Maple leaf sycamore, London plane, Plane tree | Platanus acerifolia.
| | t61 | Sycamore | Platanus occidentalis.
| | t12 | Willow | Salix caprea, Salix nigra.
| | t14 | Cottonwood (Eastern Cottonwood/Black Cottonwood) | Populus deltoides.
| | t15 | White ash | Fraxinus americana.
| | t16 | White pine | Pinus strobus.
| | t18 | Eucalyptus, gum-tree | Eucalyptus globulus (Eucalyptus spp.).
| | t19/t26 | Acacia | Acacia longifolia (Acacia spp.).
| | t20 | Mesquite | Prosopis glandulosa/Prosopis juliflora.
| | t21 | Melaleuca, cajeput tree | Melaleuca quinquenervia (Melaleuca leucadendron).
| | t22 | Pecan, hickory | Carya illinoinensis (Carya pecan).
| | t23 | Italian/Mediterranean/funeral cypress | Cupressus sempervirens.
| | t24 | Japanese cypress | Chamaecyparis obtusa (Chamaecyparis spp.).
| | t25 | Ash | Fraxinus excelsior.
| | t27 | Maple, red | Acer rubrum.
| | t29 | Acacia | Acacia spp.
| | t30 | Birch, white | Betula populifolia.
| | t32 | Willow, black | Salix nigra.
| | t33 | Ash, Arizona | Fraxinus velutina.
| | t35 | Cedar, salt | Tamarix gallica.
| | t37 | Bald cypress (white bald cypress) | Taxodium distichum.
| | t38 | Elm, Chinese/Siberian | Ulmus pumila.
| | t40 | Hazelnut tree | Corylus americana.
| | t41 | White hickory | Carya alba (Carya tomentosa).
| | t42 | Oak, red | Quercus rubra.
| | t43 | Loblolly pine | Pinus taeda.
| | t44 | Hackberry | Celtis occidentalis.
| | t45 | Cedar elm | Ulmus crassifolia.
| | t47 | Juniper, one seed | Juniperus monosperma.
| | t48 | Pine, lodgepole | Pinus contorta.
| | t49 | Pine, ponderosa | Pinus ponderosa.
| | t50 | Beech, European | Fagus sylvatica.
| | t51 | Tree of Heaven | Ailanthus altissima.
| | t52 | Western white pine | Pinus monticola.
| | t54 | Russian olive | Elaeagnus angustifolia.
| | t55 | Scotch broom | Cytisus scoparius.
| | t56 | Bayberry | Myrica cerifera.
| | t57 | Red cedar | Juniperus virginiana.
| | t60 | Western juniper | Juniperus occidentalis.
| | t61 | Sycamore | Platanus occidentalis.
| | t70 | Mulberry (white mulberry) | Morus alba.
| | t71 | Red mulberry | Morus rubra.
| | t72 | Queen palm | Arecastrum romanzoffiamon.
| | t73 | Australian pine | Casuarina equisetifolia.
| | t77 | Oak mix (red, white, black) | Quercus spp.
| | t80 | Japanese cypress | Chamaecyparis obtusa.
| | t81 | Japanese alder | Alnus japonica.
| | t83 | Mango tree | Mangifera indica.
| | t90 | Walnut, black | Juglans nigra.
| | t96 | Poplar, white (poplar) | Populus alba.
| | t103/t218 | Virginia live oak (live oak) | Quercus virginiana.
| | t105 | Pepper tree | Schinus molle.
| | t110 | Orange tree | Citrus sinensis.
| | t201 | Spruce, Norway spruce | Picea abies (Picea excelsa).
| | t202 | Alder, smooth | Alnus incana spp. Rugosa (Alnus rugosa).
| | t203 | Horse chestnut | Aesculus hippocastanum.
| | t205 | Elder | Sambucus nigra.
| | t206 | Chestnut | Castanea sativa.
| | t207 | Douglas fir | Pseudotsuga menziesii (Pseudotsuga taxifolia).
| | t208 | Linden | Tilia cordata.
| | t209 | Horn beam | Carpinus betulus.
| | t210 | Privet | Ligustrum vulgare.
| | t211 | Sweet gum | Liquidambar styraciflua.
| | t212 | Cedar | Libocedrus decurrens.
| | t213 | Pine | Pinus radiata.
| | t214 | Date palm | Phoenix canariensis.
| | t215 | Lilac | Syringa vulgaris.
| | t217 | Pepper tree | Schinus molle.
| | t217 | Red alder | Alnus rubra.
| | t218 | Virginia live oak | Quercus virginiana.
| | t218 | Bayberry (bayberry/sweet gale) | Myrica gale.
| | t219 | Palo verde | Cercidium floridum.
| | t219 | Red cedar | Juniperus virginiana.
| | t220 | Bet v 4 | Betula verrucosa (Birch).
| | t221 | Bet v 2.0101, Bet v 4 | Betula verrucosa (Birch).
| | t222 | Cypress (Arizona cypress) | Cupressus arizonica.
| | t223 | Oil palm | Elaeis guineensis.
| | t224 | Ole e 1 | Olea europaea.
| | t225 | Bet v 6 | Betula verrucosa (Birch).
| | t226 | Cup a 1 | Cupressus arizonica.
| | t227 | Ole e 7 | Olea Europaea.
| | t228 | Aspen, quaking | Populus tremuloides.
| | t229 | Eastern hemlock | Tsuga canadensis.
| | t230 | Redwood (sequoia) | Sequoia sempervirens.
| | t232 | Pussy willow | Salix discolor.
| | t240 | Ole e 9.0101 | Olea Europaea.
| | t241 | Pla a 1.0101 | Platanus acerifolia.
| | t242 | Pla a 2 | Platanus acerifolia.
| | t243 | Pla a 3.0101 | Platanus acerifolia.
| | t244 | Cor a 1.0103 | Corylus avellana.
| | t245 | Aln g 1.0101 | Alnus glutinosa.
| | t246 | Cry j 1 | Cryptomeria japonica.
| | t280 | Locust tree | Robinia pseudoacacia.
| | t401 | Brazilian peppertree | Schinus terebinthifolius.
| | t402 | Mastic tree | Pistacia lentiscus.
| | t404 | Tree of heaven | Ailanthus altissima.
| | t406 | Date palm | Phoenix dactylifera.
| | a482 | Ole e 1 | Olea europaea (Olive Oil).
| | Mites
| | d207 | Blo t 5.0101 | Blomia tropicalis.
| | d208 | Lep d 2.0101 | Lepidoglyphus destructor.
| | Microorganisms, Molds, Yeast
| | m1 | Penicillium chrysogenum (Penicillium notatum) | Penicillium chrysogenum (Penicillium notatum).
| | m2 | Cladosporium herbarum (Hormodendrum) | Cladosporium herbarum (Hormodendrum).
| | m3 | Aspergillus fumigatus | Aspergillus fumigatus.
| | m4 | Mucor racemosus | Mucor racemosus.
| | m5 | Candida albicans | Candida albicans.
| | m7 | Botrytis cinerea | Botrytis cinerea.
| | m8 | Drechslera halodes (Setomelanomma rostrata, Helminthosporium halodes, Helminthosporium interseminatum) | Drechslera halodes (Setomelanomma rostrata, Helminthosporium halodes.
| | m9 | Fusarium moniliforme (Fusarium proliferatum) | Fusarium moniliforme (Fusarium proliferatum).
| | m10 | Stemphylium botryosum | Stemphylium herbarum (Stemphylium botryosum).
| | m11 | Rhizopus nigricans | Rhizopus nigricans.
| | m12 | Aureobasidium pullulans | Aureobasidium pullulans.
| | m13 | Phoma betae | Phoma betae.
| | m14 | Epicoccum purpurascens | Epicoccum purpurascens (Epicoccum nigrum).
| | m15 | Trichoderma viride | Trichoderma viride.
| | m16 | Curvularia lunata | Curvularia lunata, Curvularia specifera (K923044).
| | m17 | Cladosporium fulvum | Cladosporium fulvum.
| | m18 | Fusarium culmorum | Fusarium culmorum.
| | m19 | Aspergillus versicolor | Aspergillus versicolor.
| | m20 | Mucor mucedo | Mucor mucedo.
| | m21 | Aspergillus clavatus | Aspergillus clavatus.
| | m22 | Micropolyspora faeni | Saccharopolyspora rectivirgula (Micropolyspora faeni).
| | m23 | Thermoactinomyces vulgaris | Thermoactinomyces vulgaris.
| | m24 | Stachybotrys atra | Stachybotrys chartarum (Stachybotrys atra).
| | m24 | Paecilomyces spp | Paecilomyces spp.
| | m25 | Aspergillus versicolor | Aspergillus versicolor.
| | m25 | Penicillium brevicompactum | Penicillium brevicompactum.
| | m26 | Cladosporium cladosporioides | Cladosporium cladosporioides.
| | m26 | Penicillium citrinum | Penicillium citrinum.
| | m27 | Penicillium spp | Penicillium spp.
| | m29 | Aspergillus repens | Aspergillus repens.
| | m30 | Penicillium roqueforti | Penicillium roqueforti.
| | m32 | Cladosporium cladosporioides | Cladosporium cladosporioides.
| | m34 | Serpula lacrymans | Serpula lacrymans.
| | m36 | Aspergillus terreus | Aspergillus terreus.
| | m37 | Trichophyton mentagrophytes | Trichophyton mentagrophytes.
| | m40 | Aspergillus amstelodami | Aspergillus amstelodami.
| | m43 | Saccharomyces Carlsberg | Saccharomyces carlsbergensis.
| | m44 | Saccharomyces cerevisiae | Saccharomyces cerevisiae.
| | m45 | Hormodendrum hordei | Hormodendrum hordei.
| | m46 | Bipolaris spicifera | Bipolaris spicifera.
| | m47 | Aspergillus nidulans | Aspergillus nidulans.
| | m48 | Aspergillus oryzae | Aspergillus oryzae.
| | m49 | Fusarium oxysporum | Fusarium oxysporum.
| | m50 | Micropolyspora faeni | Saccharopolyspora rectivirgula (Micropolyspora faeni).
| | m51 | Thermoactinomyces vulgaris | Thermoactinomyces vulgaris.
| | m53 | Microspora canis | Microsporum canis (Microspora canis).
| | m54 | Aspergillus flavus | Aspergillus flavus.
| | m63 | Helminthosporium intersemin | Helminthosporium intersemin.
| | m66 | Mucor plumbeus | Mucor plumbeus.
| | m67 | Mycogone | Mycogone perniciosa.
| | m68 | Nigrospora oryzae | Nigrospora oryzae.
| | m69 | Rhodotorula | Rhodotorula rubra (Rhodotorula mucilaginosa).
| | m70 | Malassezia furfur (Pityrosporum orbiculare) | Malassezia furfur (Pityrosporum orbiculare).
| | m71 | Spondylocladium | Spondylocladium spp.
| | m72 | Epidermophyton | Epidermophyton floccosum.
| | m73 | Epicoccum nigrum | Epicoccum purpurascens (Epicoccum nigrum).
| | m80 | Staphylococcal enterotoxin A (Sta a SEA) | Staphylococcus aureus.
| | m80 | Helminthosporium spp | Helminthosporium spp.
| | m81 | Staphylococcal enterotoxin B (Sta a SEB) | Staphylococcus aureus.
| | m88 | Stemphylium solani | Stemphylium solani.
| | m93 | Gliocladium fimbriatum | Gliocladium fimbriatum.
| | m94 | Phycomyces blakesleeanus | Phycomyces blakesleeanus.
| | m201 | Tilletia tritici (Ustilago nuda, Ustilago tritici) (Barley smut) | Tilletia tritici (Ustilago nuda, Ustilago tritici).
| | m202 | Acremonium kiliense (Cephalosporium acremonium) | Acremonium kiliense (Cephalosporium acremonium).
| | m203 | Trichosporon pullulans | Trichosporon pullulans.
| | m204 | Ulocladium chartarum | Ulocladium chartarum.
| | m205 | Trichophyton rubrum | Trichophyton rubrum.
| | m207 | Aspergillus niger | Aspergillus niger.
| | m208 | Chaetomium globosum | Chaetomium globosum.
| | m209 | Penicillium frequentans | Penicillium glabrum (Penicillium frequentans).
| | m209 | Stachybotrys chartarum | Stachybotrys chartarum (Stachybotrys atra).
| | m210 | Trichophyton mentagrophytes var. goetzii | Trichophyton mentagrophytes var. goetzii.
| | m211 | Trichophyton mentagrophytes var. interdigitale | Trichophyton mentagrophytes var. interdigitale.
| | m211 | Oat smut | Ustilago avenae.
| | m212 | Micropolyspora faeni | Saccharopolyspora rectivirgula (Micropolyspora faeni).
| | m212 | Geotrichum candidum | Geotrichum candidum.
| | m213 | Bermuda grass smut | Ustilago cynodontis.
| | m214 | Johnson grass smut | Sphacelotheca cruenta.
| | m215 | Corn smut | Ustilago maydis.
| | m218 | Asp f 1.0101 | Aspergillus fumigatus.
| | a3050 | Asp r 1 | Aspergillus restrictus.
| | m219 | Asp f 2 | Aspergillus fumigatus.
| | m220 | Asp f 3.0101 | Aspergillus fumigatus.
| | m221 | Asp f 4 | Aspergillus fumigatus.
| | m222 | Asp f 6.0101 | Aspergillus fumigatus.
| | m223 | Staphylococcal enterotoxin C (Sta a SEC) | Staphylococcus aureus.
| | m224 | Staphylococcal enterotoxin D (Sta a SED) | Staphylococcus aureus.
| | m226 | Staphylococcal enterotoxin TSST (Sta a TSST) | Staphylococcus aureus.
| | m227 | Malassezia spp. (Pityrosporum spp.) | Malassezia spp. (Pityrosporum spp.).
| | m228 | Aspergillus flavus.
| | | m229 | Alt a 1.0101 | Alternaria alternata (Alternaria tenuis).
| | m230 | Alt a 6.0101 | Alternaria alternata (Alternaria tenuis).
| | m231 | Cla h 8.0101 | Cladosporium herbarum (Hormodendrum).
| | m300 | Eurotium spp | Eurotium spp.
| | m304 | Aspergillus oryzae | Aspergillus oryzae.
| | m305 | Penicillium brevicompactum | Penicillium brevicompactum.
| | m309 | Aspergillus terreus | Aspergillus terreus.
| | m310 | Aspergillus nidulans | Aspergillus nidulans.
| | m311 | Aspergillus flavus | Aspergillus flavus.
| | m312 | Aspergillus clavatus | Aspergillus clavatus.
| | Epidermal & Animal
| | e6 | Guinea pig epithelium | Cavia porcellus.
| | e7 | Pigeon droppings | Columba palumbus, Columba livia.
| | e25 | Chicken serum | Gallus domesticus (Gallus gallus domesticus; Gallus spp.).
| | e26 | Parrot serum | Psittacoidea spp.
| | e62 | Camel | Camelus dromedaries.
| | e70 | Goose feathers | Anser anser.
| | e71 | Mouse epithelium | Mus musculus (Mus spp.).
| | e73 | Rat epithelium | Rattus norvegicus.
| | e74 | Rat urine proteins | Rattus norvegicus, Rattus rattus.
| | e75 | Rat serum proteins | Rattus norvegicus, Rattus rattus.
| | e76 | Mouse serum proteins | Mus musculus (Mus spp.).
| | e77 | Budgerigar droppings | Melopsittacus undulatus.
| | e78 | Budgerigar feathers | Melopsittacus undulatus.
| | e79 | Budgerigar serum proteins | Melopsittacus undulatus.
| | e80 | Goat epithelium | Capra hircus.
| | e81 | Sheep epithelium | Ovis aries (Ovis spp.).
| | e82 | Rabbit epithelium | Oryctolagus cuniculus (Oryctolagus spp.).
| | e83 | Swine epithelium | Sus scrofa (Sus scrofa domesticus; Sus spp.).
| | e84 | Hamster epithelium | Cricetus cricetus, Mesocricetus auratus, and Phodopus sungorus.
| | e85 | Chicken feathers | Gallus domesticus (Gallus gallus domesticus; Gallus spp.).
| | e86 | Duck feathers | Anas platyrhynchos.
| | e87 | Rat epithelium, serum proteins, and urine proteins | Rattus norvegicus Rattus rattus.
| | e88 | Mouse epithelium, serum proteins, and urine proteins (mouse) | Mus musculus (Mus spp.).
| | e89 | Turkey feathers | Meleagris gallopavo.
| | e90 | Budgerigar serum proteins, feathers, and droppings | Melopsittacus undulatus.
| | e91 | Pigeon serum proteins, feathers, and droppings | Streptopelia roseogrisea, Psittacidae spp.
| | e92 | Parrot serum proteins, feathers, and droppings | Ara spp.
| | e93 | Pigeon serum proteins | Streptopelia roseogrisea.
| | e94 | Fel d 1.0101 | Felis domesticus.
| | a345 | Fel d 1 | Felis domesticus.
| | e98 | Parrot droppings | Psittacoidea spp.
| | e101 | Can f 1.0101 | Canis familiaris (Canis domesticus).
| | a174 | Can f 1 | Canis familiaris (Canis domesticus).
| | e102 | Can f 2.0101 | Canis familiaris (Canis domesticus).
| | e196 | Parakeet feathers | Nymphicus hollandicus.
| | e197 | Parakeet droppings | Nymphicus hollandicus.
| | e198 | Parakeet serum | Nymphicus hollandicus.
| | e199 | Canary bird serum | Serinus canarius.
| | e200 | Canary bird droppings | Serinus canarius.
| | e201 | Canary bird feathers (Canary feathers) | Serinus canarius.
| | e202 | Reindeer epithelium | Rangifer tarandus.
| | e203 | Mink epithelium | Mustela spp.
| | e204 | Bos d 6 | Bos domesticus (Bos taurus; Bos spp.).
| | e205 | Horse, serum proteins | Equus caballus (Equus spp.).
| | e206 | Rabbit, serum proteins | Oryctolagus cuniculus (Oryctolagus spp.).
| | e208 | Chinchilla epithelium | Chinchilla laniger.
| | e209 | Gerbil epithelium | Meriones unguiculatus.
| | e210 | Fox epithelium | Vulpes vulpes.
| | e211 | Rabbit, urine proteins | Oryctolagus cuniculus (Oryctolagus spp.).
| | e212 | Swine, urine proteins | Sus scrofa (Sus scrofa domesticus; Sus spp.).
| | e213 | Parrot feathers | Ara spp.
| | e214 | Finch feathers | Lonchura domestica.
| | e215 | Pigeon feathers | Streptopelia roseogrisea (Streptopelia spp.), Columbia spp.
| | e216 | Deer epithelium | Dama dama.
| | e217 | Ferret epithelium | Mustela putorius.
| | e218 | Chicken droppings | Gallus domesticus (Gallus gallus domesticus; Gallus spp.).
| | e219 | Chicken, serum proteins | Gallus domesticus (Gallus gallus domesticus; Gallus spp.).
| | e220 | Fel d 2, Cat serum albumin | Felis domesticus.
| | e221 | Can f 3 | Canis familiaris (Canis domesticus) (Dog serum albumin).
| | e222 | Swine serum albumin (Sus s PSA) | Sus scrofa (Sus scrofa domesticus; Sus spp.).
| | e225 | Lovebird feathers | Psittacoidea agapomis.
| | e226 | Can f 5.0101 | Canis familiaris.
| | e227 | Equ c 1.0101 | Equus caballus.
| | e228 | Fel d 4.0101 | Felis domesticus.
| | e230 | Equ c 3 | Equus caballus.
| | e231 | Mus m 1 | Mus musculus.
| | Food
| | f9 | Rice | Oryza sativa.
| | f12 | Pea (green pea) | Pisum sativum.
| | f15 | White bean | Phaseolus vulgaris.
| | f19 | Cayenne pepper | Capsicum frutescens (Capsicum annum).
| | f21 | Sugar cane | Saccharum officinarum.
| | f22 | Raspberry | Rubus idaeus.
| | f26 | Pork | Sus scrofa (Sus scrofa domesticus; Sus spp.).
| | f29 | Watermelon | Citrullus lanatus (Citrullus vulgaris).
| | f31 | Carrot | Daucus carota.
| | f32 | Oyster mushroom | Pleurotus ostreatus.
| | f33 | Orange | Citrus sinensis.
| | f35 | Potato | Solanum tuberosum.
| | f43 | Mother's milk | Homo sapiens.
| | f44 | Strawberry | Fragaria vesca (Fragaria spp.).
| | f45 | Yeast, baker's | Saccharomyces cerevisiae.
| | f46 | Pepper, Red | Capsicum annuum.
| | f47 | Garlic | Allium sativum.
| | f48 | Onion | Allium cepa.
| | f49 | Apple | Malus x domestica (Malus spp.).
| | f51 | Bamboo shoot | Phyllostachys pubescens.
| | f52 | Cacao/chocolate | Theobroma cacao.
| | f54 | Sweet potato | Ipomoea batatas.
| | f55 | Common millet | Panicum miliaceum.
| | f56 | Foxtail millet | Setaria italica.
| | f57 | Japanese millet | Echinochloa crus-galli.
| | f58 | Pacific squid | Todarodes pacificus.
| | f59 | Octopus | Octopus vulgaris (Octopus spp.).
| | f63 | Kefir | NA.
| | f67 | Parmesan cheese | NA.
| | f81 | Cheese, cheddar type | NA.
| | f82 | Cheese, mold type | NA.
| | f83 | Chicken | Gallus domesticus (Gallus gallus domesticus; Gallus spp.).
| | f86 | Parsley | Petroselinum crispum.
| | f87 | Melon | Cucumis melo Cucumis melo + Citrullus lanatus.
| | f88 | Mutton (lamb) | Ovis aries (Ovis spp.).
| | f90 | Malt | Hordeum vulgare.
| | f92 | Banana | Musa spp.
| | f93 | Cacao | Theobroma cacao.
| | f94 | Pear | Pyrus communis (Pyrus spp.).
| | f97 | Yam | Dioscorea spp. Dioscorea opposita.
| | f97 | Chamomile tea | Matricaria chamomilla.
| | f98 | Gliadin | Triticum aestivum (Triticum spp.).
| | f102 | Cantaloupe | Cucumis melo var. cantalupensis.
| | f105 | Chocolate | Theobroma cacao.
| | f109 | Cottonseed | Gossypium hirsutum.
| | f110 | Giant radish | Raphanus sativus.
| | f118 | Zucchini | Cucurbita pepo.
| | f119 | Radish | Raphanus sativus.
| | f120 | Venison | Capreolus capeolus.
| | f121 | Pinto bean | Phaseolus vulgaris.
| | f122 | Cheese, American | NA.
| | f127 | Black-eyed pea | Vigna unguiculata.
| | f131 | Black Olive | Olea europaea.
| | f136 | Red beet | Beta vulgaris var. conditiva.
| | f139 | Goat's Cheese | Capra aegagrus.
| | f140 | Bran | NA.
| | f141 | Corn (vegetables) | Zea mays.
| | f152 | Green bell pepper | Capsicum annuum.
| | f155 | Brewer's yeast | Saccharomyces carlsbergensis.
| | f157 | Duck | Anas domesticus.
| | f158 | Goose | Anser anser.
| | f160 | Camembert cheese | NA.
| | f162 | Nectarine | Prunus persica var. nucipersica.
| | f163 | Kohlrabi | Brassica oleracea var. gongylodes.
| | f65 | Perch
| | | f166 | Leek | Allium porrum.
| | f170 | Cheese (Switzerland) (Swiss cheese) | NA.
| | f174 | Fig | Ficus carica.
| | f177 | Cranberry | Vaccinium macrocarpon.
| | f179 | Raisin | Vitis spp.
| | f182 | Lima bean | Phaseolus lunatus.
| | f198 | Flaxseed (bruised grain) | Linum usitatissimum.
| | f199 | Untreated native milk | Bos domesticus (Bos taurus; Bos spp.).
| | f208 | Lemon | Citrus limon.
| | f209 | Grapefruit | Citrus paradisi.
| | f210 | Pineapple | Ananas comosus.
| | f211 | Blackberry | Rubus fruticosus.
| | f212 | Mushroom (champignon) | Agaricus hortensis (Agaricus spp.).
| | f213 | Rabbit | Oryctolagus cuniculus (Oryctolagus spp.).
| | f214 | Spinach | Spinacia oleracea.
| | f215 | Lettuce | Lactuca sativa.
| | f216 | Cabbage | Brassica oleracea var. capitata.
| | f217 | Brussels sprouts | Brassica oleracea var. gem.
| | f218 | Paprika, sweet pepper | Capsicum annuum.
| | f219 | Fennel seed | Foeniculum vulgare.
| | f219 | Sage | Salvia officinalis.
| | f220 | Cinnamon | Cinnamomum spp.
| | f221 | Coffee | Coffea spp.
| | f222 | Tea | Camellia sinensis.
| | f223 | Green olive | Olea europaea.
| | f225 | Summer squash, pumpkin | Cucurbita pepo.
| | f225 | Pumpkin | Cucurbita maxima.
| | f226 | Pumpkin seed | Cucurbita pepo.
| | f227 | Sugar-beet seed | Beta vulgaris.
| | f229 | Safflower Seed | Carthamus tinctorius.
| | f231 | Milk, boiled | Bos domesticus (Bos taurus; Bos spp.).
| | f234 | Vanilla | Vanilla planifolia.
| | f237 | Apricot | Prunus armeniaca.
| | f241 | Gouda cheese | NA.
| | f242 | Cherry | Prunus avium.
| | f244 | Cucumber | Cucumis sativus.
| | f246 | Guar, guar gum | Cyamopsis tetragonoloba.
| | f247 | Honey | NA.
| | f248 | Rosemary | Rosmarinus officinalis.
| | f254 | Plaice | Pleuronectes platessa.
| | f255 | Plum | Prunus domestica, Prunus americana.
| | f258 | Squid | Loligo spp.
| | f259 | Grape | Vitis vinifera (Vitis spp.).
| | f260 | Broccoli | Brassica oleracea var. italica (Brassica oleracea var. cultivar).
| | f261 | Asparagus | Asparagus officinalis.
| | f262 | Aubergine, eggplant | Solanum melongena.
| | f263 | Green pepper | Piper nigrum, Capsicum annuum.
| | f264 | Eel | Anguilla anguilla.
| | f265 | Caraway | Carum carvi.
| | f265 | Cumin | Cuminum cyminum.
| | f266 | Mace | Myristica fragrans.
| | f267 | Cardamon | Elettaria cardamomum.
| | f268 | Clove | Syzygium aromaticum.
| | f269 | Basil | Ocimum basilicum.
| | f270 | Ginger | Zingiber officinale.
| | f271 | Anise | Pimpinella anisum.
| | f272 | Tarragon | Artemisia dracunculus.
| | f273 | Thyme | Thymus vulgaris.
| | f274 | Marjoram | Origanum majorana.
| | f275 | Lovage | Levisticum officinale.
| | f276 | Fennel, fresh | Foeniculum vulgare.
| | f277 | Dill | Anethum graveolens.
| | f278 | Bay leaf | Laurus nobilis.
| | f279 | Chili pepper | Capsicum frutescens.
| | f280 | Black pepper | Piper nigrum.
| | f281 | Curry (Santa Maria) | NA.
| | f282 | Nutmeg | Myristica fragrans.
| | f283 | Oregano | Origanum vulgare.
| | f284 | Turkey meat | Meleagris gallopavo.
| | f285 | Elk/moose meat | Alces spp.
| | f286 | Mare's milk | Equus caballus (Equus spp.).
| | f287 | Red kidney bean | Phaseolus vulgaris.
| | f288 | Blueberry | Vaccinium myrtillus (Vaccinium spp.).
| | f289 | Date | Phoenix dactylifera.
| | f291 | Cauliflower | Brassica oleracea var. botrytis.
| | f292 | Guava | Psidium guajava.
| | f293 | Papaya | Carica papaya.
| | f294 | Passion fruit, Maracuja | Passiflora edulis (Passiflora spp.).
| | f295 | Carambola | Averrhoa carambola.
| | f296 | Carob | Ceratonia siliqua.
| | f297 | Gum Arabic | Acacia senegal (Acacia spp.).
| | f298 | Tragacanth | Astragalus spp.
| | f299 | Sweet chestnut (chestnut) | Castanea sativa.
| | f300 | Pinto bean | Phaseolus spp.
| | f301 | Persimmon (kaki fruit, sharon) | Diospyros kaki.
| | f302 | Mandarin (tangerine, clementine, satsumas) | Citrus reticulata.
| | f305 | Fenugreek | Trigonella foenum-graecum.
| | f306 | Lime | Citrus aurantifolia.
| | f307 | Hake | Merluccius merluccius.
| | f308 | Sardine (pilchard) | Sardina pilchardus.
| | f310 | Blue vetch | Lathyrus sativus.
| | f311 | Megrim | Lepidorhombus whiffiagonis.
| | f315 | Green bean | Phaseolus vulgaris.
| | f316 | Rape seed | Brassica napus.
| | f317 | Coriander | Coriandrum sativum.
| | f318 | Jack fruit | Artocarpus heterophyllus.
| | f319 | Beetroot | Beta vulgaris.
| | f320 | Crayfish | Astacus astacus.
| | f321 | Horse meat | Equus caballus (Equus spp.).
| | f322 | Red currant | Ribes sylvestre.
| | f324 | Hop (fruit cone) | Humulus lupulus.
| | f325 | Saffron | Colchicum autumnale.
| | f328 | Fig | Ficus carica.
| | f329 | Watermelon | Citrullus lanatus.
| | f330 | Rose hip | Rosa spp.
| | f331 | Saffron | Crocus sativus.
| | f332 | Mint | Mentha piperita.
| | f333 | Linseed | Linum usitatissimum.
| | f336 | Jujube | Ziziphus jujuba.
| | f336 | Wine vinegar | Vitis vinifera (Vitis spp.).
| | f337 | Sole | Solea solea.
| | f337 | English sole | Parophrys vetulus.
| | f338 | Wine, white | Vitis vinifera (Vitis spp.).
| | f339 | Allspice | Pimenta dioica.
| | f339 | Wine, red | Vitis vinifera (Vitis spp.).
| | f341 | Cranberry | Vaccinium oxycoccus, Vaccinium macrocarpon.
| | f342 | Olive (black, fresh) | Olea europaea.
| | f343 | Raspberry | Rubus idaeus.
| | f344 | Sage | Salvia officinalis.
| | f346 | Chives | Allium schoenoprasum.
| | f347 | Quinoa | Chenopodium quinoa.
| | f348 | Litchi | Litchi chinensis.
| | f349 | Chum salmon roe | Oncorhynchus keta.
| | f358 | Artichoke | Cynara scolymus.
| | f360 | Yogurt | NA.
| | f368 | Black bass | Micropterus dolomieu (Micropterus dolomieui).
| | f374 | Karaya gum | Sterculia urens.
| | f375 | Horseradish | Armoracia rusticana.
| | f377 | Maple syrup | NA.
| | f379 | Okra | Abelmoschus esculentus.
| | f382 | Beet, sugar | Beta vulgaris var. altissima.
| | f401 | Loquat | Eriobotrya japonica.
| | f402 | Fig | Ficus carica.
| | f403 | Brewer's yeast | Saccharomyces cerevisiae.
| | f405 | Mint | Mentha spp.
| | f406 | Arugula | Eruca vesicaria.
| | House Dust
| | h1 | Greer Labs., Inc | NA.
| | h2 | Hollister-Stier Labs | NA.
| | h6 | Japan | NA.
| | Venoms & Insects
| | i7 | Midge | Chironomus yoshimatsui.
| | i8 | Moth | Bombyx mori, Heterocera spp.
| | i47 | Water flea | Daphnia spp.
| | i49 | Deer fly | Chrysops spp.
| | i51 | Black ant | Camponotus pennsylvanicus.
| | i54 | Flea mix (dog/cat), common flea | Ctenocephalides spp.
| | i71 | Mosquito | Aedes communis, Aedes spp. and Culex spp.
| | i72 | Green nimitti | Cladotanytarsus lewisi.
| | i73 | Blood worm | Chironomus thummi, Chironomusri parius, Chironomus spp.
| | i75 | European hornet | Vespa crabro.
| | i76 | Berlin beetle | Trogoderma angustum.
| | i77 | European paper wasp | Polistes dominulus.
| | i78 | Fly | Musca domestica.
| | i80 | Bumblebee | Bombus pennsylvanicus.
| | i201 | Horse bot fly | Gasterophilus intestinalis.
| | i202 | Grain weevil | Sitophilus granarius.
| | i203 | Mediterranean flour moth | Ephestia kuehniella (Anagasta kuehniella).
| | i204 | Horse fly | Tabanus spp.
| | i205 | Bumblebee | Bombus terrestris.
| | i208 | Api m 1.0101 | Apis mellifera.
| | a45 | Api m 1 | Apis mellifera.
| | i209 | Ves v 5.0101 | Vespula vulgaris.
| | a670 | Ves v 5 | Vespula vulgaris.
| | i210 | Pol d 5.0101 | Polistes dominulus.
| | i211 | Ves v 1.0101 | Vespula vulgaris.
| | i213 | Api m 4 | Apis mellifera.
| | i214 | Api m 2 | Apis mellifera.
| | i215 | Api m 3 | Apis mellifera.
| | i216 | Api m 5 | Apis mellifera.
| | i217 | Api m 10 | Apis mellifera.
| | i220 | Bla g 1.0101 | Blattella germanica.
| | i221 | Bla g 2.0101 | Blattella germanica.
| | i222 | Bla g 5.0101 | Blattella germanica.
| | i223 | Bla g 7 | Blattella germanica.
| | a46 | Api m 2 | Apis mellifera.
| | Miscellaneous
| | o1 | Cotton, crude fibers | Gossypium spp.
| | o3 | Cotton (treated) | Gossypium spp.
| | o70 | Seminal fluid | Homo sapiens.
| | o71 | Staphylococcus aureus | Staphylococcus aureus.
| | o72 | Pichia pastoris crude extract customer specific | Pichia pastoris.
| | o72 | Sperm-sediment | Homo sapiens.
| | o73 | Pichia pastoris crude extr. vector customer specific | Pichia pastoris.
| | o74 | Pichia pastoris with vector customer specific | Pichia pastoris.
| | o201 | Tobacco leaf, tobacco dust | Nicotiana tabacum.
| | o202 | Artemia salina, fish feed | Artemia salina.
| | o203 | Tetramin, fish feed | NA.
| | o207 | Daphnia, fish feed | Daphnia spp.
| | o211 | Mealworm | Tenebrio molitor.
| | o212 | Streptavidin | Streptomyces avidini.
| | o213 | MBP (maltose binding protein) | Escherichia coli.
| | o214 | CCD; MUXF3 from bromelain | Ananas comosus.
| | o72 | Enterotoxin A (Sta a SEA) | Staphylococcus aureus.
| | o73 | Enterotoxin B (Sta a SEB) | Staphylococcus aureus.
| | Parasites
| | p1 | Ascaris | Ascaris suum.
| | p2 | Echinococcus | Echinococcus granulosus.
| | p3 | Schistosoma | Schistosoma mansoni.
| | p4 | Anisakis (Herring Worm) | Anisakis simplex (Anisakis spp.).
| | p5 | Toxocara canis | Toxocara canis.
| | p10 | Ani s 3.0101 | Anisakis simplex (Anisakis spp.).
| | p11 | Ani s 1 | Anisakis simplex (Anisakis spp.).
| | Occupational
| | k4 | Threshing dust | NA.
| | k5 | Flax | NA.
| | k7 | Hay Dust | NA.
| | k8 | Hop (hops) | Humulus lupulus.
| | k12 | Grain mill dust | NA.
| | k14 | Kapok | NA.
| | k20 | Sheep's wool (treated) (wool) | Ovis aries (Ovis spp.).
| | k21 | Sheep's wool (Untreated) | Ovis aries (Ovis spp.).
| | k23 | Straw Dust | NA.
| | k33 | Oak | NA.
| | k70 | Green coffee bean | Coffea spp.
| | k71 | Castor bean | Ricinus communis.
| | k72 | Ispaghula | Plantago psyllium/Plantago ovata.
| | k73 | Silk waste | NA.
| | k74 | Silk | Bombyx mori.
| | k75 | Isocyanate TDI (Toluene diisocyanate) | NA.
| | k76 | Isocyanate MDI (Diphenylmethane diisocyanate) | NA.
| | k77 | Isocyanate HDI (Hexamethylen diisocyanate) | NA.
| | k78 | Ethylene oxide | NA.
| | k79 | Phthalic anhydride | NA.
| | k80 | Formaldehyde/Formalin | NA.
| | k81 | Ficus | Ficus benjamina (Ficus spp.).
| | k83 | Cotton seed | Gossypium hirsutum.
| | k84 | Sunflower seed | Helianthus annuus.
| | k85 | Chloramin T | NA.
| | k86 | Trimellitic anhydride, TMA | NA.
| | k87 | Asp o 21, alpha-amylase | Aspergillus oryzae.
| | k89 | Orris root | Iris florentina.
| | k99 | HSA (Human Serum Albumin) (Hom s HSA) | Homo sapiens.
| | k201 | Car p 1, Papain | Carica papaya.
| | k202 | Ana c 2, Bromelain | Ananas comosus.
| | k204 | Maxatase | Bacillus licheniformis.
| | k205 | Alcalase | Bacillus spp.
| | k206 | Savinase, Protease 1 (Bac l Subtilisin) | Bacillus spp.
| | k208 | Gal d 4, Lysozyme | Gallus domesticus (Gallus gallus domesticus; Gallus spp.).
| | k209 | Hexahydrophtalic anhydrid | NA.
| | k210 | Maleic anhydride | NA.
| | k211 | Methyltetrahydrophtalic anhydrid | NA.
| | k212 | Abachi wood dust | Triplochiton scleroxylon.
| | k213 | Pepsin (Sus s Pepsin) | Sus scrofa (Sus scrofa domesticus; Sus spp.).
| | k213 | TCPA | NA.
| | k214 | Bougainvillea | Bougainvillea spp.
| | k225 | Horse radish peroxidase (Arm r HRP) | Armoracia rusticana.
| | k226 | Ascorbate oxidase (Cuc p ascorbate oxidase) | Cucurbita pepo.
| | k301 | Flour dust | Triticum spp.
| | k501 | Savinase customer specific | Proprietary knowledge of customer.
| | k502 | Lipolase customer specific | Proprietary knowledge of customer.
| | k503 | Termamyl customer specific | Proprietary knowledge of customer.
| | k504 | Clazinase customer specific | Proprietary knowledge of customer. |
[47 FR 50823, Nov. 9, 1982, as amended at 84 FR 71800, Dec. 30, 2019]
|
|
|
Sec. 866.5760 Tryptase test system.
|
|
(a) Identification. A tryptase test system is a device that aids in the diagnosis of systemic mastocytosis. It is intended for in vitro diagnostic use as an aid in the clinical diagnosis of patients with a suspicion of systemic mastocytosis in conjunction with other clinical and laboratory findings.
(b) Classification. Class II (special controls). The special control is FDA's guideline entitled "Class II Special Controls Guideline: Tryptase Test System as an Aid in the Diagnosis of Systemic Mastocytosis." For availability of the document, see § 866.1(e).
[79 FR 56010, Sept. 18, 2014]
|
|
|
Sec. 866.5765 Retinol-binding protein immunological test system.
|
|
(a) Identification. A retinol-binding protein immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the retinol-binding protein that binds and transports vitamin A in serum and urine. Measurement of this protein may aid in the diagnosis of kidney disease and in monitoring patients with kidney transplants.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 65 FR 2313, Jan. 14, 2000]
|
|
|
Sec. 866.5775 Rheumatoid factor immunological test system.
|
|
(a) Identification. A rheumatoid factor immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the rheumatoid factor (antibodies to immunoglobulins) in serum, other body fluids, and tissues. Measurement of rheumatoid factor may aid in the diagnosis of rheumatoid arthritis.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5785 Anti-Saccharomyces cerevisiae (S. cerevisiae) antibody (ASCA) test systems.
|
|
(a) Identification. The Anti-Saccharomyces cerevisiae (S. cerevisiae ) antibody (ASCA) test system is an in vitro diagnostic device that consists of the reagents used to measure, by immunochemical techniques, antibodies to S. cerevisiae (baker's or brewer's yeast) in human serum or plasma. Detection of S. cerevisiae antibodies may aid in the diagnosis of Crohn's disease.
(b) Classification. Class II (special controls). The special control is FDA's "Guidance for Industry and FDA Reviewers: Class II Special Control Guidance Document for Anti-Saccharomyces cerevisiae (S. cerevisiae ) Antibody (ASCA) Premarket Notifications."
[65 FR 70307, Nov. 22, 2000]
|
|
|
Sec. 866.5800 Seminal fluid (sperm) immunological test system.
|
|
(a) Identification. A seminal fluid (sperm) immunological test system is a device that consists of the reagents used for legal purposes to identify and differentiate animal and human semen. The test results may be used as court evidence in alleged instances of rape and other sex-related crimes.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[54 FR 25047, June 12, 1989, as amended at 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5820 Systemic lupus erythematosus immunological test system.
|
|
(a) Identification. A systemic lupus erythematosus (SLE) immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the autoimmune antibodies in serum and other body fluids that react with cellular nuclear double-stranded deoxyribonucleic acid (DNA) or other nuclear constituents that are specifically diagnostic of SLE. Measurement of nuclear double-stranded DNA antibodies aids in the diagnosis of SLE (a multisystem autoimmune disease in which tissues are attacked by the person's own antibodies).
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5830 Brain trauma assessment test.
|
|
(a) Identification. A brain trauma assessment test is a device that consists of reagents used to detect and measure brain injury biomarkers in human specimens. The measurements aid in the evaluation of patients with suspected mild traumatic brain injury in conjunction with other clinical information to assist in determining the need for head imaging per current standard of care.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The 21 CFR 809.10(b) compliant labeling must include detailed descriptions of and results from performance testing conducted to evaluate precision, accuracy, linearity, analytical sensitivity, interference, and cross-reactivity. This information must include the following:
(i) Performance testing of device precision must, at minimum, use one unmodified clinical specimen from the intended use population with concentration of the brain injury biomarker(s) near the medical decision point. Contrived specimens that have been generated from pooling of multiple samples or spiking of purified analyte to cover the measuring range may be used, but the contrived samples must be prepared to mimic clinical specimens as closely as possible. This testing must evaluate repeatability and reproducibility using a protocol from an FDA-recognized standard.
(ii) Device performance data must be demonstrated through a clinical study and must include the following:
(A) Data demonstrating clinical validity including the clinical sensitivity and specificity, and positive and negative predictive value of the test in the intended use population of patients with suspected mild traumatic brain injury (i.e., Glasgow Coma Score (GCS) of 13-15), or equivalent standard of care for determination of severity of traumatic brain injury (TBI).
(B) Study must be performed using the operators and in settings that are representative of the types of operators and settings for which the device is intended to be used.
(C) All eligible subjects must meet the well-defined study inclusion and exclusion criteria that define the intended use population. The prevalence of diseased or injured subjects in the study population must reflect the prevalence of the device's intended use population, or alternatively, statistical measures must be used to account for any bias due to enrichment of subpopulations of the intended use population.
(D) All eligible subjects must have undergone a head computerized tomography (CT) scan or other appropriate clinical diagnostic standard used to determine the presence of an intracranial lesion as part of standard of care and must also be evaluated by the subject device. All clinical diagnostic standards used in the clinical study must follow standard clinical practice in the United States.
(E) Relevant demographic variables and baseline characteristics including medical history and neurological history. In addition, head injury characteristics, neurological assessments, and physical evidence of trauma must be provided for each subject. This information includes but is not limited to the following: Time since head injury, time from head injury to CT scan, time from head injury to blood draw, GCS score or equivalent, experience of loss of consciousness, presence of confusion, episodes of vomiting, post-traumatic amnesia characteristics, presence of post-traumatic seizures, drug or alcohol intoxication, mechanism of injury, acute intracranial lesion type, neurosurgical lesion, and cranial fracture.
(F) Each CT scan or other imaging result must be independently evaluated in a blinded manner by at least two board-certified radiologists to determine whether it is positive or negative as defined by the presence or absence of acute intracranial lesions. This independent review must be conducted without access to test results of the device. Prior to conducting the review, the criteria and procedures to be followed for scoring the images must be established, including the mechanism for determining consensus.
(G) All the clinical samples must be tested with the subject device blinded to the TBI status and the neurological-lesion-status of the subject.
(H) Details on how missing values in data are handled must be provided.
(I) For banked clinical samples, details on storage conditions and storage period must be provided. In addition, a specimen stability study must be conducted for the duration of storage to demonstrate integrity of archived clinical samples. The samples evaluated in the assay test development must not be used to establish the clinical validity of the assays.
(iii) Performance testing of device analytical specificity must include the most commonly reported concomitant medications present in specimens from the intended use population. Additionally, potential cross-reacting endogenous analytes must be evaluated at the highest concentration reported in specimens from the intended use population.
(iv) Expected/reference values generated by testing a statistically appropriate number of samples from apparently healthy normal individuals.
(2) The 21 CFR 809.10(a) and (b) compliant labeling must include the following limitations:
(i) A limiting statement that this device is not intended to be used a stand-alone device but as an adjunct to other clinical information to aid in the evaluation of patients who are being considered for standard of care neuroimaging.
(ii) A limiting statement that reads "A negative result is generally associated with the absence of acute intracranial lesions. An appropriate neuroimaging method is required for diagnosis of acute intracranial lesions."
(iii) As applicable, a limiting statement that reads "This device is for use by laboratory professionals in a clinical laboratory setting."
[83 FR 27701, June 14, 2018]
|
|
|
Sec. 866.5860 Total spinal fluid immunological test system.
|
|
(a) Identification. A total spinal fluid immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the total protein in cerebrospinal fluid. Measurement of spinal fluid proteins may aid in the diagnosis of multiple sclerosis and other diseases of the nervous system.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 61 FR 1119, Jan. 16, 1996; 66 FR 38793, July 25, 2001]
|
|
|
Sec. 866.5870 Thyroid autoantibody immunological test system.
|
|
(a) Identification. A thyroid autoantibody immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the thyroid autoantibodies (antibodies produced against the body's own tissues). Measurement of thyroid autoantibodies may aid in the diagnosis of certain thyroid disorders, such as Hashimoto's disease (chronic lymphocytic thyroiditis), nontoxic goiter (enlargement of thyroid gland), Grave's disease (enlargement of the thyroid gland with protrusion of the eyeballs), and cancer of the thyroid.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5880 Transferrin immunological test system.
|
|
(a) Identification. A transferrin immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the transferrin (an iron-binding and transporting serum protein) in serum, plasma, and other body fluids. Measurement of transferrin levels aids in the diagnosis of malnutrition, acute inflammation, infection, and red blood cell disorders, such as iron deficiency anemia.
(b) Classification. Class II (performance standards).
|
|
|
Sec. 866.5890 Inter-alpha trypsin inhibitor immunological test system.
|
|
(a) Identification. An inter-alpha trypsin inhibitor immunological test system is a device that consists of the reagents used to measure by immunochemical techniques the inter-alpha trypsin inhibitor (a protein) in serum and other body fluids. Measurement of inter-alpha trypsin inhibitor may aid in the diagnosis of acute bacterial infection and inflammation.
(b) Classification. Class I (general controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to § 866.9.
[47 FR 50823, Nov. 9, 1982, as amended at 53 FR 11253, Apr. 6, 1988; 65 FR 2313, Jan. 14, 2000]
|
|
|
Sec. 866.5900 Cystic fibrosis transmembrane conductance regulator (CFTR) gene mutation detection system.
|
|
(a) Identification. The CFTR gene mutation detection system is a device used to simultaneously detect and identify a panel of mutations and variants in the CFTR gene. It is intended as an aid in confirmatory diagnostic testing of individuals with suspected cystic fibrosis (CF), carrier identification, and newborn screening. This device is not intended for stand-alone diagnostic purposes, prenatal diagnostic, pre-implantation, or population screening.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: CFTR Gene Mutation Detection System." See § 866.1(e) for the availability of this guidance document.
[70 FR 61738, Oct. 26, 2005]
|
|
|
Sec. 866.5910 Quality control material for cystic fibrosis nucleic acid assays.
|
|
(a) Identification. Quality control material for cystic fibrosis nucleic acid assays. A quality control material for cystic fibrosis nucleic acid assays is a device intended to help monitor reliability of a test system by detecting analytical deviations such as those that may arise from reagent or instrument variation in genetic testing. This type of device includes recombinant, synthetic, and cell line-based DNA controls.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9. The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: Quality Control Material for Cystic Fibrosis Nucleic Acid Assays." See § 866.1(e) for the availability of this guidance document.
[72 FR 1176, Jan. 10, 2007, as amended at 84 FR 71811, Dec. 30, 2019]
|
|
|
Sec. 866.5930 Newborn screening test for severe combined immunodeficiency disorder (SCID).
|
|
(a) Identification. A newborn screening test for SCID is a prescription device intended to measure T-cell receptor excision circle (TREC) DNA obtained from dried blood spot specimens on filter paper using a polymerase chain reaction based test as an aid in screening newborns for SCID. Presumptive positive results must be followed up by diagnostic confirmatory testing. This test is not intended for use as a diagnostic test, or for screening of SCID-like syndromes, such as DiGeorge syndrome or Omenn syndrome. It is also not intended to screen for less acute SCID syndromes, such as leaky SCID or variant SCID.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include the following information:
(i) The intended use must indicate:
(A) The test is not intended for diagnostic use, or for screening of SCID-like syndromes, such as DiGeorge syndrome or Omenn syndrome; and
(B) The test is not intended to screen for less acute SCID syndromes, such as leaky SCID or variant SCID.
(ii) A detailed description of all components in the test that includes:
(A) A detailed description of the test components, all required reagents, instrumentation and equipment, including illustrations or photographs of nonstandard equipment or methods;
(B) Detailed documentation of the device software including, but not limited to, standalone software applications and hardware-based devices that incorporate software;
(C) Specifications for the filter paper, which must be appropriately labeled for in vitro diagnostic use, to be used in specimen collection and how it will be used in specimen collection validation. These specifications must include: descriptive characteristics of the filter paper, instructions on how a lab should choose the appropriate filter paper, chemical properties of the filter paper, interference concerns associated with the chemicals in the filter paper, absorption properties of the filter paper, punch size, absorption capacity, testing for homogeneity of punches, diameter of the circle for the dried blood spot aliquot, absorption time, physical composition, and number and size of punches to be tested;
(D) Methodology and protocols for detection of T-cell receptor excision circles and methods for determination of results. The cutoff must be selected before conducting clinical and analytical studies;
(E) A description of the result outputs along with sample reports. Sample reports must include the scale used in reporting of results (e.g., TREC copies/[micro]L) and the range of values that will be reported out; and
(F) A description of appropriate internal and external controls that are recommended or provided. The description must identify those control elements that are incorporated into the testing procedure.
(iii) Information that demonstrates the performance characteristics of the test, including:
(A) Data that demonstrates the clinical validity of the device, using well characterized prospectively or retrospectively obtained clinical specimens representative of the intended use population. A minimum of 10 to 15 confirmed positive specimens must be obtained from more than 1 site, including relevant annotation, and, at 1 year or beyond, a SCID diagnosis by flow cytometry or clinically meaningful information regarding the status of the subject must be obtained. Additional specimens should have been obtained that are characterized by other disorders that can be found by screening specimens that have low or absent TREC (e.g., other T-cell lymphopenic disorders) to supplement the range of results. The clinical validation study must have a pre-specified clinical decision point (i.e., cutoff to distinguish positive and negative results). Results must be summarized in tabular format comparing interpretation of results to the reference method. Point estimates together with two-sided 95 percent confidence intervals must be provided for the positive percent agreement, negative percent agreement, and overall percent agreement. Data must include the retest rate, the false positive rate before retest, the final false positive rate, and the false negative rate;
(B) Device reproducibility data generated, using a minimum of three sites of which at least two must be external sites, with two operators at each site. Each site must conduct a minimum of five runs per operator over five nonconsecutive days evaluating a minimum of six different relevant TREC concentrations that span and are well distributed over the measuring range and include the clinical cutoff. Specimens must include cord blood and cord blood diluted with ABO matched adult blood specimens. Identical specimens from the same sample panel must be tested at each site. Each specimen must be run in triplicate and include controls run in triplicate. Results must be reported as the standard deviation and percentage coefficient of variation for each level tested. Results must also be displayed as a dichotomous variable around the cutoff. Total variation must be partitioned into the sum of within-lab and between-lab variations with pre-specified acceptance criteria and 95 percent confidence intervals for all data. Pre-specified acceptance criteria must be provided and followed;
(C) Device precision data using clinical samples to evaluate the within-lot, between-lot, within-run, between run, and total variation. A range of TREC levels of the specimen must include samples within the measuring range, samples above and below the measuring range, as well as with samples very near above and below the cutoff value. At least three replicates of each specimen must be tested with controls and calibrator(s) according to the device instructions for use. The precision study must use well characterized samples using different lots, instruments, and operators. Results must be summarized in tabular format. Pre-specified acceptance criteria must be provided and followed;
(D) Linearity of the test must be demonstrated using a dilution panel from clinical samples. The range of dilution samples must include samples within the measuring range, samples above and below the measuring range, as well as with samples very near above and below the cutoff value. Results of the regression analysis must be summarized in tabular format and fitted into a linear regression model with the individual measurement results against the dilution factors. Pre-specified acceptance criteria must be provided and followed;
(E) Device analytic sensitivity data, including limit of blank, limit of detection, and limit of quantification;
(F) Device specificity data, including interference, carryover, cross-contamination, and in silico analysis of potential off-target genomic sequences;
(G) Device stability data, including real-time stability of samples under various storage times, temperatures, and freeze-thaw conditions. A separate shipping stability study must be performed;
(H) Lot-to-lot reproducibility study of each filter paper that will be validated with the test. The lot-to-lot study must include a minimum of three lots of each blood spot card that will be validated with the test and be conducted over five nonconsecutive days. The sample panel must consist of specimens with a range of TREC levels and include samples within the measuring range, samples above and below the measuring range, and samples very near above and below the cutoff value. Multiple punches must be obtained from each card for demonstration of homogeneity of the analyte across the dried blood spot. Comparability of the test performance for each filter paper must be demonstrated. Stability and storage of TREC DNA on each blood spot card must be demonstrated. Results of the lot-to-lot study must be summarized providing the mean, standard deviation, and percentage coefficient of variation in a tabular format. Data must be calculated for within-run, between-run, within-lot, and between-lot. Data demonstrating the concordance between results across different filter papers must be provided. Study acceptance criteria must be provided and followed; and
(I) If applicable, a thermocycler reproducibility study must be performed using thermocyclers from three independent thermocyler manufacturers. The sample panel must consist of specimens with a range of TREC levels and must include samples within the measuring range, samples above and below the measuring range, and samples very near above and below the cutoff value. The study must be done using three filter paper lots and conducted over five nonconsecutive days. Results of the thermocycler reproducibility study must be summarized providing the mean, standard deviation, and percentage coefficient of variance in a tabular format. Data must be calculated for the within-run, between-run, within-lot, between-lot, and between thermocycler manufacturer study results. Study acceptance criteria must be provided and followed.
(iv) Identification of risk mitigation elements used by your device, including a description of all additional procedures, methods, and practices incorporated into the directions for use that mitigate risks associated with testing.
(2) Your § 809.10 compliant labeling must include:
(i) A warning statement that reads "This test is not intended for diagnostic use, preimplantation or prenatal testing, or for screening of SCID-like syndromes, such as DiGeorge syndrome or Omenn syndrome. It is also not intended to screen for less acute SCID syndromes, such as leaky SCID or variant SCID.";
(ii) A warning statement that reads "Test results are intended to be used in conjunction with other clinical and diagnostic findings, consistent with professional standards of practice, including confirmation by alternative methods and clinical evaluation, as appropriate.";
(iii) A description of the performance studies listed in paragraph (b)(1)(iii) and a summary of the results; and
(iv) A description of the filter paper specifications required for the test.
[82 FR 50079, Oct. 30, 2017]
|
|
|
Sec. 866.5940 Autosomal recessive carrier screening gene mutation detection system.
|
|
(a) Identification. Autosomal recessive carrier screening gene mutation detection system is a qualitative in vitro molecular diagnostic system used for genotyping of clinically relevant variants in genomic DNA isolated from human specimens intended for prescription use or over-the-counter use. The device is intended for autosomal recessive disease carrier screening in adults of reproductive age. The device is not intended for copy number variation, cytogenetic, or biochemical testing.
(b) Classification. Class II (special controls). The device is exempt from the premarket notification procedures in subpart E of part 807 of this chapter subject to the limitations in § 866.9, except § 866.9(c)(2). Autosomal recessive carrier screening gene mutation detection system must comply with the following special controls:
(1) If the device is offered over-the-counter, the device manufacturer must provide information to a potential purchaser or actual test report recipient about how to obtain access to a board-certified clinical molecular geneticist or equivalent to assist in pre- and post-test counseling.
(2) The device must use a collection device that is FDA cleared, approved, or classified as 510(k) exempt, with an indication for in vitro diagnostic use in DNA testing.
(3) The device's labeling must include a prominent hyperlink to the manufacturer's public Web site where the manufacturer shall make the information identified in this section publicly available. The manufacturer's home page, as well as the primary part of the manufacturer's Web site that discusses the device, must provide a prominently placed hyperlink to the Web page containing this information and must allow unrestricted viewing access. If the device can be purchased from the Web site or testing using the device can be ordered from the Web site, the same information must be found on the Web page for ordering the device or provided in a prominently placed and publicly accessible hyperlink on the Web page for ordering the device. Any changes to the device that could significantly affect safety or effectiveness would require new data or information in support of such changes, which would also have to be posted on the manufacturer's Web site. The information must include:
(i) A detailed device description including:
(A) Gene (or list of the genes if more than one) and variants the test detects (using standardized nomenclature, Human Genome Organization (HUGO) nomenclature, and coordinates).
(B) Scientifically established clinical validity of each variant detected and reported by the test, which must be well-established in peer-reviewed journal articles, authoritative summaries of the literature such as Genetics Home Reference (http://ghr.nlm.nih.gov/ ), GeneReviews (http://www.ncbi.nlm.nih.gov/books/NBK1116/ ), or similar summaries of valid scientific evidence, and/or professional society recommendations, including:
(1 ) Genotype-phenotype information for the reported mutations.
(2 ) Relevant American College of Medical Genetics (ACMG) or American Congress of Obstetricians and Gynecologists (ACOG) guideline recommending testing of the specific gene(s) and variants the test detects and recommended populations, if available. If not available, a statement stating that professional guidelines currently do not recommend testing for this specific gene(s) and variants.
(3 ) Table of expected prevalence of carrier status in major ethnic and racial populations and the general population.
(C) The specimen type (e.g., saliva, whole blood), matrix, and volume.
(D) Assay steps and technology used.
(E) Specification of required ancillary reagents, instrumentation, and equipment.
(F) Specification of the specimen collection, processing, storage, and preparation methods.
(G) Specification of risk mitigation elements and description of all additional procedures, methods, and practices incorporated into the directions for use that mitigate risks associated with testing.
(H) Information pertaining to the probability of test failure (e.g., failed quality control) based on data from clinical samples, description of scenarios in which a test can fail (i.e., low sample volume, low DNA concentration, etc.), how customers will be notified, and followup actions to be taken.
(I) Specification of the criteria for test result interpretation and reporting.
(ii) Information that demonstrates the performance characteristics of the device, including:
(A) Accuracy (method comparison) of study results for each claimed specimen type.
(1 ) Accuracy of the device shall be evaluated with fresh clinical specimens collected and processed in a manner consistent with the device's instructions for use. If this is impractical, fresh clinical samples may be substituted or supplemented with archived clinical samples. Archived samples shall have been collected previously in accordance with the device's instructions for use, stored appropriately, and randomly selected. In some instances, use of contrived samples or human cell line samples may also be appropriate; the contrived or human cell line samples shall mimic clinical specimens as much as is feasible and provide an unbiased evaluation of the device's accuracy.
(2 ) Accuracy must be evaluated as compared to bidirectional sequencing or other methods identified as appropriate by FDA. Performance criteria for both the comparator method and device must be predefined and appropriate to the test's intended use. Detailed appropriate study protocols must be provided.
(3 ) Information provided shall include the number and type of specimens, broken down by clinically relevant variants, that were compared to bidirectional sequencing or other methods identified as appropriate by FDA. The accuracy, defined as positive percent agreement (PPA) and negative percent agreement (NPA), must be measured; accuracy point estimates must be greater than 99 percent (both per reported variant and overall) and uncertainty of the point estimate must be presented using the 95 percent confidence interval. Clinical specimens must include both homozygous wild type and heterozygous genotypes. The number of clinical specimens for each variant reported that must be included in the accuracy study must be based on the variant prevalence. Common variants (greater than 0.1 percent allele frequency in ethnically relevant population) must have at least 20 unique heterozygous clinical specimens tested. Rare variants (less than or equal to 0.1 percent allele frequency in ethnically relevant population) shall have at least three unique mutant heterozygous specimens tested. Any no calls (i.e., absence of a result) or invalid calls (e.g., failed quality control) in the study must be included in accuracy study results and reported separately. Variants that have a point estimate for PPA or NPA of less than 99 percent (incorrect test results as compared to bidirectional sequencing or other methods identified as appropriate by FDA) must not be incorporated into test claims and reports. Accuracy measures generated from clinical specimens versus contrived samples or cell lines must be presented separately. Results must be summarized and presented in tabular format, by sample and by genotype. Point estimate of PPA should be calculated as the number of positive results divided by the number of specimens known to harbor variants (mutations) without "no calls" or invalid calls. The point estimate of NPA should be calculated as the number of negative results divided by the number of wild type specimens tested without "no calls" or invalid calls, for each variant that is being reported. Point estimates should be calculated along with 95 percent two-sided confidence intervals.
(4 ) Information shall be reported on the clinical positive predictive value (PPV) and negative predictive value (NPV) for carrier status (and where possible, for each variant) in each population. Specifically, to calculate PPV and NPV, estimate test coverage (TC) and the percent of persons with variant(s) included in the device among all carriers: PPV = (PPA * TC * Ï?)/(PPA * TC * Ï? + (1 â?? NPA) * (1 â?? Ï?)) and NPV = (NPA * (1 â?? Ï?))/(NPA *(1 â?? Ï?) + (1 â?? PPA*TC) * Ï?) where PPA and NPA described either in paragraph (b)(3)(ii)(A)(4 )(i ) or in paragraph (b)(3)(ii)(A)(4 )(ii ) of this section and Ï? is prevalence of carriers in the population (pre-test risk to be a carrier for the disease).
(i ) For the point estimates of PPA and NPA less than 100 percent, use the calculated estimates in the PPV and NPV calculations.
(ii ) Point estimates of 100 percent may have high uncertainty. If these variants are measured using highly multiplexed technology, calculate the random error rate for the overall device and incorporate that rate in the estimation of the PPA and NPA as calculated previously. Then use these calculated estimates in the PPV and NPV calculations. This type of accuracy study is helpful in determining that there is no systematic error in such devices.
(B) Precision (reproducibility): Precision data must be generated using multiple instruments and multiple operators, on multiple non-consecutive days, and using multiple reagent lots. The sample panel must include specimens with claimed sample type (e.g. saliva samples) representing different genotypes (i.e., wild type, heterozygous). Performance criteria must be predefined. A detailed study protocol must be created in advance of the study and then followed. The "failed quality control" rate must be indicated. It must be clearly documented whether results were generated from clinical specimens, contrived samples, or cell lines. The study results shall state, in a tabular format, the variants tested in the study and the number of replicates for each variant, and what testing conditions were studied (i.e., number of runs, days, instruments, reagent lots, operators, specimens/type, etc). The study must include all nucleic acid extraction steps from the claimed specimen type or matrix, unless a separate extraction study for the claimed sample type is performed. If the device is to be used at more than one laboratory, different laboratories must be included in the precision study (and reproducibility must be evaluated). The percentage of "no calls" or invalid calls, if any, in the study must be provided as a part of the precision (reproducibility) study results.
(C) Analytical specificity data: Data must be generated evaluating the effect on test performance of potential endogenous and exogenous interfering substances relevant to the specimen type, evaluation of cross-reactivity of known cross-reactive alleles and pseudogenes, and assessment of cross-contamination.
(D) Analytical sensitivity data: Data must be generated demonstrating the minimum amount of DNA that will enable the test to perform accurately in 95 percent of runs.
(E) Device stability data: The manufacturer must establish upper and lower limits of input nucleic acid and sample stability that will achieve the claimed accuracy and reproducibility. Data supporting such claims must be described.
(F) Specimen type and matrix comparison data: Specimen type and matrix comparison data must be generated if more than one specimen type or anticoagulant can be tested with the device, including failure rates for the different specimen types.
(iii) If the device is offered over-the-counter, including cases in which the test results are provided direct-to-consumer, the manufacturer must conduct a study that assesses user comprehension of the device's labeling and test process and provide a concise summary of the results of the study. The following items must be included in the user study:
(A) The test manufacturer must perform pre- and post-test user comprehension studies to assess user ability to understand the possible results of a carrier test and their clinical meaning. The comprehension test questions must directly evaluate the material being presented to the user in the test reports.
(B) The test manufacturer must provide a carrier testing education module to potential and actual test report recipients. The module must define terms that are used in the test reports and explain the significance of carrier status.
(C) The user study must meet the following criteria:
(1 ) The study participants must be comprised of a statistically justified and demographically diverse population (determined using methods such as quota-based sampling) that is representative of the intended user population. Furthermore, the users must be comprised of a diverse range of age and educational levels that have no prior experience with the test or its manufacturer. These factors shall be well-defined in the inclusion and exclusion criteria.
(2 ) All sources of bias (e.g., non-responders) must be predefined and accounted for in the study results with regard to both responders and non-responders.
(3 ) The testing must follow a format where users have limited time to complete the studies (such as an onsite survey format and a one-time visit with a cap on the maximum amount of time that a participant has to complete the tests).
(4 ) Users must be randomly assigned to study arms. Test reports given to users must: Define the condition being tested and related symptoms; explain the intended use and limitations of the test; explain the relevant ethnicities regarding the variant tested; explain carrier status and relevance to the user's ethnicity; and provide links to additional information pertaining to situations where the user is concerned about their test results or would like followup information as indicated in test labeling. The study shall assess participants' ability to understand the following comprehension concepts: The test's limitations, purpose, and results.
(5 ) Study participants must be untrained, naive to the test subject of the study, and be provided only the materials that will be available to them when the test is marketed.
(6 ) The user comprehension study must meet the predefined primary endpoint criteria, including a minimum of a 90 percent or greater overall comprehension rate (i.e. selection of the correct answer) for each comprehension concept to demonstrate that the education module and test reports are adequate for over-the-counter use.
(D) A summary of the user comprehension study must be provided and include the following:
(1 ) Results regarding reports that are provided for each gene/variant/ethnicity tested.
(2 ) Statistical methods used to analyze all data sets.
(3 ) Completion rate, non-responder rate, and reasons for non-response/data exclusion, as well as a summary table of comprehension rates regarding comprehension concepts (purpose of test, test results, test limitations, ethnicity relevance for the test results, etc.) for each study report.
(4) Your 21 CFR 809.10 compliant labeling and any test report generated must include the following warning and limitation statements, as applicable:
(i) A warning that reads "The test is intended only for autosomal recessive carrier screening in adults of reproductive age."
(ii) A statement accurately disclosing the genetic coverage of the test in lay terms, including, as applicable, information on variants not queried by the test, and the proportion of incident disease that is not related to the gene(s) tested. For example, where applicable, the statement would have to include a warning that the test does not or may not detect all genetic variants related to the genetic disease, and that the absence of a variant tested does not rule out the presence of other genetic variants that may be disease-related. Or, where applicable, the statement would have to include a warning that the basis for the disease for which the genetic carrier status is being tested is unknown or believed to be non-heritable in a substantial number of people who have the disease, and that a negative test result cannot rule out the possibility that any offspring may be affected with the disease. The statement would have to include any other warnings needed to accurately convey to consumers the degree to which the test is informative for carrier status.
(iii) For prescription use tests, the following warnings that read:
(A) "The results of this test are intended to be interpreted by a board-certified clinical molecular geneticist or equivalent and should be used in conjunction with other available laboratory and clinical information."
(B) "This device is not intended for disease diagnosis, prenatal testing of fetuses, risk assessment, prognosis or pre-symptomatic testing, susceptibility testing, or newborn screening."
(iv) For over-the-counter tests, a statement that reads "This test is not intended to diagnose a disease, or tell you anything about your risk for developing a disease in the future. On its own, this test is also not intended to tell you anything about the health of your fetus, or your newborn child's risk of developing a particular disease later on in life."
(v) For over-the-counter tests, the following warnings that read:
(A) "This test is not a substitute for visits to a healthcare provider. It is recommended that you consult with a healthcare provider if you have any questions or concerns about your results."
(B) "The test does not diagnose any health conditions. Results should be used along with other clinical information for any medical purposes."
(C) "The laboratory may not be able to process your sample. The probability that the laboratory cannot process your saliva sample can be up to [actual probability percentage]."
(D) "Your ethnicity may affect how your genetic health results are interpreted."
(vi) For a positive result in an over-the-counter test when the positive predictive value for a specific population is less than 50 percent and more than 5 percent, a warning that reads "The positive result you obtained may falsely identify you as a carrier. Consider genetic counseling and followup testing."
(vii) For a positive result in an over-the-counter test when the positive predictive value for a specific population is less than 5 percent, a warning that reads "The positive result you obtained is very likely to be incorrect due to the rarity of this variant. Consider genetic counseling and followup testing."
(5) The testing done to comply with paragraph (b)(3) of this section must show the device meets or exceeds each of the following performance specifications:
(i) The accuracy must be shown to be equal to or greater than 99 percent for both PPA and NPA. Variants that have a point estimate for PPA or NPA of less than 99 percent (incorrect test results as compared to bidirectional sequencing or other methods identified as appropriate by FDA) must not be incorporated into test claims and reports.
(ii) Precision (reproducibility) performance must meet or exceed 99 percent for both positive and negative results.
(iii) The user comprehension study must obtain values of 90 percent or greater user comprehension for each comprehension concept.
(6) The distribution of this device, excluding the collection device described in paragraph (b)(2) of this section, shall be limited to the manufacturer, the manufacturer's subsidiaries, and laboratories regulated under the Clinical Laboratory Improvement Amendments.
[80 FR 65630, Oct. 27, 2015, as amended at 82 FR 51570, Nov. 7, 2017]
|
|
|
Sec. 866.5950 Genetic health risk assessment system.
|
|
(a) Identification. A genetic health risk assessment system is a qualitative in vitro molecular diagnostic system used for detecting variants in genomic deoxyribonucleic acid (DNA) isolated from human specimens that will provide information to users about their genetic risk of developing a disease to inform lifestyle choices and/or conversations with a health care professional. This assessment system is for over-the-counter use. This device does not determine the person's overall risk of developing a disease.
(b) Classification. Class II (special controls). The genetic health risk assessment system device, when it has previously received a first-time FDA marketing authorization (e.g., 510(k) clearance) for the genetic health risk assessment system (a "one-time FDA reviewed genetic health risk assessment system"), is exempt from the premarket notification procedures in part 807, subpart E, of this chapter subject to the limitations in § 866.9. The device must comply with the following special controls:
(1) The 21 CFR 809.10 compliant labeling and any prepurchase page and test report generated, unless otherwise specified, must include:
(i) A section addressed to users with the following information:
(A) The limiting statement explaining that this test provides genetic risk information based on assessment of specific genetic variants but does not report on a user's entire genetic profile. This test [does not/may not, as appropriate] detect all genetic variants related to a given disease, and the absence of a variant tested does not rule out the presence of other genetic variants that may be related to the disease.
(B) The limiting statement explaining that other companies offering a genetic risk test may be detecting different genetic variants for the same disease, so the user may get different results using a test from a different company.
(C) The limiting statement explaining that other factors such as environmental and lifestyle risk factors may affect the risk of developing a given disease.
(D) The limiting statement explaining that some people may feel anxious about getting genetic test health results. This is normal. If the potential user feels very anxious, such user should speak to his or her doctor or other health care professional prior to collection of a sample for testing. This test is not a substitute for visits to a doctor or other health care professional. Users should consult with their doctor or other health care professional if they have any questions or concerns about the results of their test or their current state of health.
(E) Information about how to obtain access to a genetic counselor, board-certified clinical molecular geneticist, or equivalent health care professional about the results of a user's test.
(F) The limiting statement explaining that this test is not intended to diagnose a disease, tell you anything about your current state of health, or be used to make medical decisions, including whether or not you should take a medication or how much of a medication you should take.
(G) A limiting statement explaining that the laboratory may not be able to process a sample, and a description of the next steps to be taken by the manufacturer and/or the customer, as applicable.
(ii) A section in your 21 CFR 809.10 labeling and any test report generated that is for health care professionals who may receive the test results from their patients with the following information:
(A) The limiting statement explaining that this test is not intended to diagnose a disease, determine medical treatment, or tell the user anything about their current state of health.
(B) The limiting statement explaining that this test is intended to provide users with their genetic information to inform lifestyle decisions and conversations with their doctor or other health care professional.
(C) The limiting statement explaining that any diagnostic or treatment decisions should be based on testing and/or other information that you determine to be appropriate for your patient.
(2) The genetic test must use a sample collection device that is FDA-cleared, -approved, or -classified as 510(k) exempt, with an indication for in vitro diagnostic use in over-the-counter DNA testing.
(3) The device's labeling must include a hyperlink to the manufacturer's public Web site where the manufacturer shall make the information identified in paragraph (b)(3) of this section publicly available. The manufacturer's home page, as well as the primary part of the manufacturer's Web site that discusses the device, must provide a hyperlink to the Web page containing this information and must allow unrestricted viewing access. If the device can be purchased from the Web site or testing using the device can be ordered from the Web site, the same information must be found on the Web page for ordering the device or provided in a publicly accessible hyperlink on the Web page for ordering the device. Any changes to the device that could significantly affect safety or effectiveness would require new data or information in support of such changes, which would also have to be posted on the manufacturer's Web site. The information must include:
(i) An index of the material being provided to meet the requirements in paragraph (b)(3) of this section and its location.
(ii) A section that highlights summary information that allows the user to understand how the test works and how to interpret the results of the test. This section must, at a minimum, be written in plain language understandable to a lay user and include:
(A) Consistent explanations of the risk of disease associated with all variants included in the test. If there are different categories of risk, the manufacturer must provide literature references that support the different risk categories. If there will be multiple test reports and multiple variants, the risk categories must be defined similarly among them. For example, "increased risk" must be defined similarly between different test reports and different variant combinations.
(B) Clear context for the user to understand the context in which the cited clinical performance data support the risk reported. This includes, but is not limited to, any risks that are influenced by ethnicity, age, gender, environment, and lifestyle choices.
(C) Materials that explain the main concepts and terminology used in the test that include:
(1 ) Definitions: Scientific terms that are used in the test reports.
(2 ) Prepurchase page: This page must contain information that informs the user about what information the test will provide. This includes, but is not limited to, variant information, the condition or disease associated with the variant(s), professional guideline recommendations for general genetic risk testing, the limitations associated with the test (e.g., test does not detect all variants related to the disease) and any precautionary information about the test the user should be aware of before purchase. When the test reports the risk of a life-threatening or irreversibly debilitating disease or condition for which there are few or no options to prevent, treat, or cure the disease, a user opt-in section must be provided. This opt-in page must be provided for each disease that falls into this category and must provide specific information relevant to each test result. The opt-in page must include:
(i ) An option to accept or decline to receive this specific test result;
(ii ) Specification of the risk involved if the user is found to have the specific genetic test result;
(iii ) Professional guidelines that recommend when genetic testing for the associated target condition is or is not recommended; and
(iv ) A recommendation to speak with a health care professional, genetic counselor, or equivalent professional before getting the results of the test.
(3 ) Frequently asked questions (FAQ) page: This page must provide information that is specific for each variant/disease pair that is reported. Information provided in this section must be scientifically valid and supported by corresponding publications. The FAQ page must explain the health condition/disease being tested, the purpose of the test, the information the test will and will not provide, the relevance of race and ethnicity to the test results, information about the population to which the variants in the test is most applicable, the meaning of the result(s), other risk factors that contribute to disease, appropriate followup procedures, how the results of the test may affect the user's family, including children, and links to resources that provide additional information.
(iii) A technical information section containing the following information:
(A) Gene(s) and variant(s) the test detects using standardized nomenclature, Human Genome Organization nomenclature and coordinates as well as Single Nucleotide Polymorphism Database (dbSNP) reference SNP numbers (rs#).
(B) Scientifically established disease-risk association of each variant detected and reported by the test. This risk association information must include:
(1 ) Genotype-phenotype information for the reported variants.
(2 ) Table of expected frequency and risks of developing the disease in relevant ethnic populations and the general population.
(3 ) A statement about the current professional guidelines for testing these specific gene(s) and variant(s).
(i ) If professional guidelines are available, provide the recommendations in the professional guideline for the gene, variant, and disease, for when genetic testing should or should not be performed, and cautionary information that should be communicated when a particular gene and variant is detected.
(ii ) If professional guidelines are not available, provide a statement that the professional guidelines are not available for these specific gene(s) and variant(s).
(C) The specimen type (e.g., saliva, capillary whole blood).
(D) Assay steps and technology used.
(E) Specification of required ancillary reagents, instrumentation, and equipment.
(F) Specification of the specimen collection, processing, storage, and preparation methods.
(G) Specification of risk mitigation elements and description of all additional procedures, methods, and practices incorporated into the directions for use that mitigate risks associated with testing.
(H) Information pertaining to the probability of test failure (i.e., percentage of tests that failed quality control) based on data from clinical samples, a description of scenarios in which a test can fail (i.e., low sample volume, low DNA concentration, etc.), how users will be notified of a test failure, and the nature of followup actions on a failed test to be taken by the user and the manufacturer.
(I) Specification of the criteria for test result interpretation and reporting.
(J) Information that demonstrates the performance characteristics of the test, including:
(1 ) Accuracy of study results for each claimed specimen type.
(i ) Accuracy of the test shall be evaluated with fresh clinical specimens collected and processed in a manner consistent with the test's instructions for use. If this is impractical, fresh clinical samples may be substituted or supplemented with archived clinical samples. Archived samples shall have been collected previously in accordance with the instructions for use, stored appropriately, and randomly selected. In some limited circumstances, use of contrived samples or human cell line samples may also be appropriate and used as an acceptable alternative. The contrived or human cell line samples shall mimic clinical specimens as much as is feasible and provide an unbiased evaluation of the device accuracy.
(ii ) Accuracy must be evaluated by comparison to bidirectional Sanger sequencing or other methods identified as appropriate by FDA. Performance criteria for both the comparator method and the device must be predefined and appropriate to the device's intended use. Detailed study protocols must be provided.
(iii ) Test specimens must include all genotypes that will be included in the tests and reports. The number of samples tested in the accuracy study for each variant reported must be based on the variant frequency using either the minimum numbers of samples identified in this paragraph or, when determined appropriate and identified by FDA, a minimum number of samples determined using an alternative method. When appropriate, the same samples may be used in testing to demonstrate the accuracy of testing for multiple genotypes by generating sequence information at multiple relevant genetic locations. At least 20 unique samples representing the wild-type genotype must be tested. To test samples that are heterozygous for the reported variant(s), common variants (>0.1 percent variant frequency in the relevant population) must be tested with at least 20 unique samples. Rare variants (â?¤0.1 percent variant frequency in the relevant population) must be tested with at least three unique samples. To test samples that are homozygous for the reported variant(s), variants with â?¥2 percent variant frequency in a relevant population must be tested with at least 20 unique samples. Variants with a frequency in the relevant population <2 percent and â?¥0.5 percent must be tested with at least 10 unique samples. Variants with a frequency in the relevant population <0.5 percent must be tested with at least three unique samples. If variants with a frequency of <0.5 percent are not found within the relevant population and homozygous samples are not tested, then the test results for this homozygous rare variant must not be reported to the user.
(iv ) Information about the accuracy study shall include the number and type of samples that were compared to bidirectional Sanger sequencing or other methods identified as appropriate by FDA. This information must either be reported in tabular format and arranged by clinically relevant variants or reported using another method identified as appropriate by FDA. As an example, for samples with different genotypes DD, Dd, and dd, the following table represents data from the accuracy study presented in tabular format:

(v ) The accuracy represents the degrees of agreement between the device results and the comparator results. The accuracy must be evaluated by measuring different percent agreements (PA) of device results with the comparator results and percent of `no calls' or `invalid calls.' Calculate the rate of `no calls' and `invalid calls' for each comparator output as %Inv(DD) = A4/NDD, %Inv(Dd) = B4/NDd, %Inv(dd) = C4/Ndd. If `no calls' or `invalid calls' are required to be retested according to the device instructions for use, the percent of final `no calls' or `invalid calls' must be provided. In the table presenting the results of the accuracy study, use only the final results (i.e., after retesting the initial `no calls' or `invalid calls', if required according to the instructions for use). Samples that resulted in a `no call' or `invalid call' after retesting must not be included in the final calculations of agreement. If the percentages of `no calls' or `invalid calls' for each comparator output are similar, combine these estimates as (A4 + B4 + C4)/(NDD + NDd + Ndd) and provide a 95 percent two-sided confidence interval. The percent of final `no calls' or `invalid calls' must be clinically acceptable.
(vi ) Point estimates of percent agreement for each genotype must be calculated as the number of correct calls for that genotype divided by the number of samples known to contain that genotype excluding `no calls' or `invalid calls'. The calculations must be performed as follows:
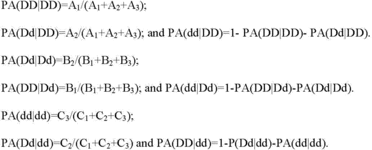
(vii ) For percent agreements for DD, Dd and dd (PA(DD|DD), PA(Dd|Dd) and PA(dd|dd)) as described in paragraph (b)(3)(iii)(J)(1 )(vi ) of this section, the 95 percent two-sided confidence intervals must be provided. The accuracy point estimates for percent agreements for DD, Dd and dd must be â?¥99 percent per reported variant and overall. Any variants that have a point estimate for either PA(DD|DD), PA(Dd|Dd), or PA(dd|dd) of <99 percent compared to bidirectional sequencing or other methods identified as appropriate by FDA must not be incorporated into test claims and reports. Accuracy results generated from clinical specimens versus contrived samples or cell lines must be presented separately. Results must be summarized and presented in tabular format by sample type and by genotype or must be reported using another method identified as appropriate by FDA (see paragraph (b)(3)(iii)(J)(1 )(iv ) of this section).
(viii ) Information must be reported on the Technical Positive Predictive Value (TPPV) related to the analytical (technical) performance of the device for genotypes in each relevant subpopulation (e.g., ethnicity, gender, age, geographical location, etc.). TPPV is the percentage of individuals with the genotype truly present among individuals whose test reports indicate that this genotype is present. The TPPV depends on the accuracy measures of percent agreements and on the frequency of the genotypes in the subpopulation being studied. The f(DD) is the frequency of DD and f(Dd) is the frequency of Dd in the subpopulation being studied; TPPV must be calculated as described in paragraphs (b)(3)(iii)(J)(1 )(ix ) through (xi ) of this section.
(ix ) For variants where the point estimates of PA(DD|DD), PA(Dd|Dd) and PA(dd|dd) are less than 100 percent, use these point estimates in TPPV calculations.
(x ) Point estimates of 100 percent in the accuracy study may have high uncertainty about performance of the test in the population. If these variants are measured using highly multiplexed technology, calculate the random error rate for the overall device. The accuracy study described in paragraph (b)(3)(iii)(J) of this section in those cases is more to determine that there is no systematic error in such devices. In those cases, incorporate that rate in the estimation of the percent agreements as calculated in paragraph (b)(3)(iii)(J)(1 )(vi ) of this section and include it in TPPV calculations.
(xi ) The TPPV for subpopulations with genotype frequencies of f(dd), f(Dd) and f(DD) = 1â??f(dd)â??f(Dd) in the subpopulation is calculated as:

(2 ) Precision and reproducibility data must be provided using multiple instruments and multiple operators, on multiple non-consecutive days, and using multiple reagent lots. The sample panel must either include specimens from the claimed sample type (e.g., saliva) representing all genotypes for each variant (e.g., wild type, heterozygous, and homozygous) or, if an alternative panel composition of specimens is identified by FDA as appropriate, a panel composed of those specimens FDA identified as appropriate. A detailed study protocol must be created in advance of the study and must include predetermined acceptance criteria for performance results. The percentage of samples that failed quality control must be indicated (i.e., the total number of sample replicates for which a sequence variant cannot be called (no calls) or that fail sequencing quality control criteria divided by the total number of replicates tested). It must be clearly documented whether results were generated from clinical specimens, contrived samples, or cell lines. The study results shall report the variants tested in the study and the number of replicates for each variant, and what conditions were tested (i.e., number of runs, days, instruments, reagent lots, operators, specimens/type, etc.). Results must be evaluated and presented in tabular format and stratified by study parameter (e.g., by site, instrument(s), reagent lot, operator, and sample variant). The study must include all extraction steps from the claimed specimen type or matrix, unless a separate extraction reproducibility study for the claimed sample type is performed. If the device is to be used at more than one laboratory, different laboratories must be included in the reproducibility study and reproducibility across sites must be evaluated. Any no calls or invalid calls in the study must be listed as a part of the precision and reproducibility study results.
(3 ) Analytical specificity data: Data must be provided that evaluates the effect of potential endogenous and exogenous interferents on test performance, including specimen extraction and variant detection. Interferents tested must include those reasonably likely to be potentially relevant to the sample type used for the device.
(4 ) Interfering variant data: Nucleotide mutations that can interfere with the technology must be cited and evaluated. Data must be provided to demonstrate the effect of the interfering variant(s) on the performance of the correct calls. Alternatively, for each suspected interfering mutation for which data is not provided demonstrating the effect of the interfering variant, the manufacturer must identify the suspected interfering variants in the labeling and indicate that the impact that the interfering variants may have on the assay's performance has not been studied by providing a statement that reads "It is possible that the presence of [insert clearly identifying information for the suspected interfering variant] in a sample may interfere with the performance of this test. However, its effect on the performance of this test has not been studied."
(5 ) Analytical sensitivity data: Data must be provided demonstrating the minimum amount of DNA that will enable the test to perform correctly in 95 percent of runs.
(6 ) Reagent stability: The manufacturer must evaluate reagent stability using wild-type, heterozygous, and homozygous samples. Reagent stability data must demonstrate that the reagents maintain the claimed accuracy and reproducibility. Data supporting such claims must be provided.
(7 ) Specimen type and matrix comparison data: Specimen type and matrix comparison data must be generated if more than one specimen type can be tested with this device, including failure rates for the different specimens.
(K) Clinical performance summary.
(1 ) Information to support the clinical performance of each variant reported by the test must be provided.
(2 ) Manufacturers must organize information by the specific variant combination as appropriate (e.g., wild type, heterozygous, homozygous, compound heterozygous, hemizygous genotypes). For each variant combination, information must be provided in the clinical performance section to support clinical performance for the risk category (e.g., not at risk, increased risk). For each variant combination, a summary of key results must be provided in tabular format or using another method identified as appropriate by FDA to include the appropriate information regarding variant type, data source, definition of the target condition (e.g., disease), clinical criteria for determining whether the target disease is present or absent, description of subjects with the target disease present and target disease absent (exclusion or inclusion criteria), and technical method for genotyping. When available, information on the effect of the variant on risk must be provided as the risk of a disease (lifetime risk or lifetime incidences) for an individual compared with the general population risk.
(i ) If odds ratios are available, using information about the genotype distribution either among individuals with the target disease absent, or in the general population, or information about the risk variant frequency and odds ratios, the likelihood ratios for the corresponding device results along with 95 percent confidence intervals must be calculated. Using information about pretest risk (Ï?), an estimate of likelihood ratio (LR), and a relationship between post-test risk R as R/(1â??R) = LR-Ï?/(1â??Ï?), the post-test risk R must be calculated.
(ii ) When available, likelihood ratios (LR) for different test results must be presented in a tabular format along with references to the source data or using another method identified as appropriate by FDA as stated in paragraph (b)(3)(iii)(K)(2) of this section. When these values are not directly available in published literature, likelihood ratios can be separately calculated along with the 95 percent confidence interval with references to the source data. Note that a minimum requirement for the presence of the variant's effect on the risk is that a corresponding LR is statistically higher than 1 (a lower bound of 95 percent two-sided confidence interval is larger than 1). It means that the post-test risk is statistically higher than the pretest risk (an observed value of the difference between the post-test and pretest risks).
(L) Materials that explain the main concepts and terminology used in the test that includes, but is not limited to:
(1 ) Definitions: Scientific terms that are used in the test reports.
(2 ) Prepurchase page: This page must contain information that informs the user about what the test will provide. This includes, but is not limited to, variant information, the condition or disease associated with the variant(s), professional guideline recommendations for general genetic risk testing, the limitations associated with the test (e.g., test does not detect all variants related to the disease) and any precautionary information about the test the user should be aware of before purchase. When the test reports the risk of a life-threatening or irreversibly debilitating disease or condition for which there are few or no options to prevent, treat, or cure the disease, a user opt-in section must be provided. This opt-in page must be provided for each disease that falls into this category and must provide specific information relevant to each test result. The opt-in page must include:
(i ) An option to accept or decline to receive this specific test result;
(ii ) Specification of the risk involved if the user is found to have the specific genetic test result;
(iii ) Professional guidelines that recommend when genetic testing for the associated target condition is or is not recommended; and
(iv ) A recommendation to speak with a health care professional, genetic counselor, or equivalent professional before getting the results of the test.
(3 ) Frequently asked questions (FAQ) page: This page must provide information that is specific for each variant/disease pair that is reported. Information provided in this section must be scientifically valid and supported by corresponding publications. The FAQ page must explain the health condition/disease being tested, the purpose of the test, the information the test will and will not provide, the relevance of race and ethnicity on the test results, information about the population to which the variants in the test is most applicable, the meaning of the result(s), other risks factors that contribute to disease, appropriate followup procedures, how the results of the test may affect the user's family, including children, and links to resources that provide additional information.
(M) User comprehension study: Information on a study that assesses comprehension of the test process and results by potential users of the test must be provided.
(1 ) The test manufacturer must provide a genetic risk education module to naive user comprehension study participants prior to their participation in the user comprehension study. The module must define terms that are used in the test reports and explain the significance of genetic risk reports.
(2 ) The test manufacturer must perform pre- and post-test user comprehension studies. The comprehension test questions must include directly evaluating a representative sample of the material being presented to the user as described in paragraph (b)(3)(ii) of this section.
(3 ) The manufacturer must provide a justification from a physician and/or genetic counselor that identifies the appropriate general and variant-specific concepts contained within the material being tested in the user comprehension study to ensure that all relevant concepts are incorporated in the study.
(4 ) The user study must meet the following criteria:
(i ) The study participants must comprise a statistically sufficient sample size and demographically diverse population (determined using methods such as quota-based sampling) that is representative of the intended user population. Furthermore, the study participants must comprise a diverse range of age and educational levels and have no prior experience with the test or its manufacturer. These factors shall be well defined in the inclusion and exclusion criteria.
(ii ) All sources of bias must be predefined and accounted for in the study results with regard to both responders and non-responders.
(iii ) The testing must follow a format where users have limited time to complete the studies (such as an onsite survey format and a one-time visit with a cap on the maximum amount of time that a participant has to complete the tests).
(iv ) Users must be randomly assigned to study arms. Test reports in the user comprehension study given to users must define the target condition being tested and related symptoms, explain the intended use and limitations of the test, explain the relevant ethnicities in regard to the variant tested, explain genetic health risks and relevance to the user's ethnicity, and assess participants' ability to understand the following comprehension concepts: The test's limitations, purpose, appropriate action, test results, and other factors that may have an impact on the test results.
(v ) Study participants must be untrained, be naive to the test subject of the study, and be provided the labeling prior to the start of the user comprehension study.
(vi ) The user comprehension study must meet the predefined primary endpoint criteria, including a minimum of a 90 percent or greater overall comprehension rate (i.e., selection of the correct answer) for each comprehension concept. Other acceptance criteria may be acceptable depending on the concept being tested. Meeting or exceeding this overall comprehension rate demonstrates that the materials presented to the user are adequate for over-the-counter use.
(vii ) The analysis of the user comprehension results must include results regarding reports that are provided for each gene/variant/ethnicity tested, statistical methods used to analyze all data sets, and completion rate, non-responder rate, and reasons for nonresponse/data exclusion. A summary table of comprehension rates regarding comprehension concepts (e.g., purpose of test, test results, test limitations, ethnicity relevance for the test results, etc.) for each study report must be included.
(4) The intended use of the device must not include the following indications for use:
(i) Prenatal testing;
(ii) Determining predisposition for cancer where the result of the test may lead to prophylactic screening, confirmatory procedures, or treatments that may incur morbidity or mortality to the patient;
(iii) Assessing the presence of genetic variants that impact the metabolism, exposure, response, risk of adverse events, dosing, or mechanisms of prescription or over-the-counter medications; or
(iv) Assessing the presence of deterministic autosomal dominant variants.
[82 FR 51561, Nov. 7, 2017, as amended at 83 FR 25914, June 5, 2018]
|
|
|
Sec. 866.5960 Human leukocyte antigen typing companion diagnostic test.
|
|
(a) Identification. A human leukocyte antigen (HLA) typing companion diagnostic (CDx) test is a prescription genotyping or phenotyping in vitro diagnostic product intended for use as an aid in identifying patients who have specific HLA allele(s) or express specific HLA antigen(s) and may benefit from treatment with a corresponding therapeutic product or are likely to be at increased risk for serious adverse reactions as a result of treatment with a corresponding therapeutic product.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) The intended use of the device must specify the target HLA allele(s) or antigen(s), the patient population(s), and the corresponding therapeutic product(s).
(2) Design verification and validation must include:
(i) Detailed documentation of an analytical accuracy study that uses well-characterized samples including clinical samples from intended use population(s) focusing on the target allele(s) needed for patient selection;
(ii) Detailed documentation of precision studies (repeatability, reproducibility) that evaluate possible sources of variation that may affect test results;
(iii) Detailed documentation of a study determining range of input sample concentrations that meet performance specifications;
(iv) Detailed description of the ambiguity resolution method, if applicable;
(v) For a sequencing-based assay, documentation of coverage and predefined coverage threshold of target genomic regions, pertinent variant types, and sequence contexts;
(vi) For multiplex assays, documentation of a risk assessment and design specifications that are in place to prevent incorrect reactivity assignment;
(vii) Description of a plan on how to ensure the performance of the device does not change when new HLA alleles are identified, and/or when reactivity assignments are changed; and
(viii) Detailed description of device software including standalone software, or software and bioinformatics analysis pipeline, if applicable, incorporated in the instruments, and documentation of software including the level of concern and associated risks, software requirement specifications, software design specifications (e.g., algorithms, alarms and device limitations), hazard analysis, traceability matrix, verification and validation testing, unresolved anomalies, hardware requirements, and effective cybersecurity management.
(3) Clinical validity data (which may include summary reports from clinical trials, comparison studies using clinical samples, or through an alternative approach determined to be appropriate by FDA), demonstrating the following, as applicable:
(i) Which patients identified by the HLA CDx test are most likely to benefit from the corresponding therapeutic product; and
(ii) Which patients identified by the HLA CDx test are likely to be at increased risk for serious adverse reactions as a result of treatment with the corresponding therapeutic product.
(4) If the HLA test used in the clinical trials is different from the HLA CDx test in the premarket notification submission, the submission must include results of a bridging study, or an alternative approach determined to be appropriate by FDA.
[87 FR 79252, Dec. 27, 2022]
|
|
|
Subpart G - Tumor Associated Antigen immunological Test Systems
|
|
Sec. 866.6010 Tumor-associated antigen immunological test system.
|
|
(a) Identification. A tumor-associated antigen immunological test system is a device that consists of reagents used to qualitatively or quantitatively measure, by immunochemical techniques, tumor-associated antigens in serum, plasma, urine, or other body fluids. This device is intended as an aid in monitoring patients for disease progress or response to therapy or for the detection of recurrent or residual disease.
(b) Classification. Class II (special controls). Tumor markers must comply with the following special controls: (1) A guidance document entitled "Guidance Document for the Submission of Tumor Associated Antigen Premarket Notifications (510(k)s) to FDA," and (2) voluntary assay performance standards issued by the National Committee on Clinical Laboratory Standards.
[62 FR 66005, Dec. 17, 1997]
|
|
|
Sec. 866.6020 Immunomagnetic circulating cancer cell selection and enumeration system.
|
|
(a) Identification. An immunomagnetic circulating cancer cell selection and enumeration system is a device that consists of biological probes, fluorochromes, and other reagents; preservation and preparation devices; and a semiautomated analytical instrument to select and count circulating cancer cells in a prepared sample of whole blood. This device is intended for adjunctive use in monitoring or predicting cancer disease progression, response to therapy, and for the detection of recurrent disease.
(b) Classification. Class II (special controls). The special control for this device is FDA's guidance document entitled "Class II Special Controls Guidance Document: Immunomagnetic Circulating Cancer Cell Selection and Enumeration System." See § 866.1(e) for availability of this guidance document.
[69 FR 26038, May 11, 2004]
|
|
|
Sec. 866.6030 AFP-L3% immunological test system.
|
|
(a) Identification. An AFP-L3% immunological test system is an in vitro device that consists of reagents and an automated instrument used to quantitatively measure, by immunochemical techniques, AFP and AFP-L3 subfraction in human serum. The device is intended for in vitro diagnostic use as an aid in the risk assessment of patients with chronic liver disease for development of hepatocellular carcinoma, in conjunction with other laboratory findings, imaging studies, and clinical assessment.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: AFP-L3% Immunological Test Systems." See § 866.1(e) for the availability of this guidance document.
[70 FR 57749, Oct. 4, 2005]
|
|
|
Sec. 866.6040 Gene expression profiling test system for breast cancer prognosis.
|
|
(a) Identification. A gene expression profiling test system for breast cancer prognosis is a device that measures the ribonucleic acid (RNA) expression level of multiple genes and combines this information to yield a signature (pattern or classifier or index) to aid in prognosis of previously diagnosed breast cancer.
(b) Classification. Class II (special controls). The special control is FDA's guidance document entitled "Class II Special Controls Guidance Document: Gene Expression Profiling Test System for Breast Cancer Prognosis." See § 866.1(e) for the availability of this guidance document.
[72 FR 26291, May 9, 2007]
|
|
|
Sec. 866.6050 Ovarian adnexal mass assessment score test system.
|
|
(a) Identification. An ovarian/adnexal mass assessment test system is a device that measures one or more proteins in serum or plasma. It yields a single result for the likelihood that an adnexal pelvic mass in a woman, for whom surgery is planned, is malignant. The test is for adjunctive use, in the context of a negative primary clinical and radiological evaluation, to augment the identification of patients whose gynecologic surgery requires oncology expertise and resources.
(b) Classification. Class II (special controls). The special control for this device is FDA's guidance document entitled "Class II Special Controls Guidance Document: Ovarian Adnexal Mass Assessment Score Test System." For the availability of this guidance document, see § 866.1(e).
(c) Black box warning. Under section 520(e) of the Federal Food, Drug, and Cosmetic Act these devices are subject to the following restriction: A warning statement must be placed in a black box and must appear in all advertising, labeling, and promotional material for these devices. That warning statement must read:
 [76 FR 16294, Mar. 23, 2011, as amended at 76 FR 82131, Dec. 30, 2011]
|
|
|
Sec. 866.6060 BCR-ABL quantitation test.
|
|
(a) Identification. A BCR-ABL quantitation test is identified as a reverse transcription-quantitative polymerase chain reaction (RT-qPCR) test for the quantitation of BCR-ABL1 expressed on the International Scale (IS) and control transcripts in total RNA from whole blood of diagnosed t(9;22) positive chronic myeloid leukemia (CML) patients during monitoring of treatment with tyrosine kinase inhibitors. This test is not intended for the diagnosis of CML.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include the following information:
(i) The indication for use must indicate the variant(s) for which the assay was designed and validated, for example BCR-ABL e13a2 and/or e14a2.
(ii) A detailed description of all components in the test, including the following:
(A) A detailed description of the test components, all required reagents, instrumentation and equipment, including illustrations or photographs of non-standard equipment or methods;
(B) Detailed documentation of the device software including, but not limited to, standalone software applications and hardware-based devices that incorporate software;
(C) Methodology and protocols for control procedures for the assay to allow reporting on the International Scale;
(D) A description of the result outputs, analytical sensitivity of the assay, and the range of values that will be reported; and
(E) A description of appropriate internal and external controls that are recommended or provided. The description must identify those control elements that are incorporated into the testing procedure.
(iii) Information that demonstrates the performance characteristics of the test, including:
(A) For indications for use based on a threshold established in a predicate device of this generic type, device performance data from either a method comparison study to the predicate device or through a clinical study demonstrating clinical validity using well-characterized prospectively or retrospectively obtained clinical specimens, as appropriate, representative of the intended use population;
(B) For indications for use based on a threshold not established in a predicate device of this generic type, device performance data from a clinical study demonstrating clinical validity using well-characterized prospectively or retrospectively obtained clinical specimens, as appropriate, representative of the intended use population;
(C) Device reproducibility data generated, using a minimum of three sites, of which at least two sites must be external sites, with two operators at each site. Each site must conduct a minimum of three runs per operator over non-consecutive days evaluating a minimum of five different BCR-ABL concentrations that span and are well distributed over the measuring range and include MR3 (0.1 percent IS). Results shall be reported as the standard deviation and percentage coefficient of variation for each level tested. Prespecified acceptance criteria must be provided and followed;
(D) Device precision data using clinical samples to evaluate the within-lot, between-lot, within-run, between run, and total variation;
(E) Device linearity data using a dilution panel created from clinical samples;
(F) Device analytic sensitivity data, including limit of blank, limit of detection, and limit of quantification;
(G) Device specificity data, including interference and cross-contamination; and
(H) Device stability data, including real-time stability of samples under various storage times, temperatures, and freeze-thaw conditions.
(iv) Identification of risk mitigation elements used by your device, including a detailed description of all additional procedures, methods, and practices incorporated into the instructions for use that mitigate risks associated with testing using your device.
(2) Your 21 CFR 809.10 compliant labeling must include the following:
(i) The intended use in your 21 CFR 809.10(a)(2) and (b)(2) complaint labeling must include an indication for use statement that reads "This test is not intended for the diagnosis of CML"; and
(ii) A detailed description of the performance studies conducted to comply with paragraph (b)(1)(iii) of this section and a summary of the results.
(3) Your device output must include results on the International Scale (IS) and your assay must include multipoint calibration controls traceable to a relevant international reference panel (e.g., the World Health Organization International Genetic Reference Panel for quantitation of BCR-ABL mRNA).
[82 FR 50532, Nov. 1, 2017]
|
|
|
Sec. 866.6080 Next generation sequencing based tumor profiling test.
|
|
(a) Identification. A next generation sequencing (NGS) based tumor profiling test is a qualitative in vitro diagnostic test intended for NGS analysis of tissue specimens from malignant solid neoplasms to detect somatic mutations in a broad panel of targeted genes to aid in the management of previously diagnosed cancer patients by qualified health care professionals.
(b) Classification. Class II (special controls). The special controls for this device are:
(1) Premarket notification submissions must include the following information:
(i) A detailed description of all somatic mutations that are intended to be detected by the test and that are adequately supported in accordance with paragraph (b)(1)(v) of this section and reported in the test results in accordance with paragraph (b)(2)(iv) of this section, including:
(A) A listing of mutations that are cancer mutations with evidence of clinical significance.
(B) As appropriate, a listing of mutations that are cancer mutations with potential clinical significance.
(ii) The indications for use must specify the following:
(A) The test is indicated for previously diagnosed cancer patients.
(B) The intended specimen type(s) and matrix (e.g., formalin-fixed, paraffin-embedded tumor tissue).
(C) The mutation types (e.g., single nucleotide variant, insertion, deletion, copy number variation or gene rearrangement) for which validation data has been provided.
(D) The name of the testing facility or facilities, as applicable.
(iii) A detailed device description including the following:
(A) A description of the test in terms of genomic coverage, as follows:
(1 ) Tabulated summary of all mutations reported, grouped according to gene and target region within each gene, along with the specific cDNA and amino acid positions for each mutation.
(2 ) A description of any within-gene targeted regions that cannot be reported and the data behind such conclusion.
(B) Specifications for specimen requirements including any specimen collection devices and preservatives, specimen volume, minimum tumor content, specimen handling, DNA extraction, and criteria for DNA quality and quantity metrics that are prerequisite to performing the assay.
(C) A detailed description of all test components, reagents, instrumentation, and software required. Detailed documentation of the device software including but not limited to, software applications and hardware-based devices that incorporate software.
(D) A detailed description of the methodology and protocols for each step of the test, including description of the quality metrics, thresholds, and filters at each step of the test that are implemented for final result reporting and a description of the metrics for run-failures, specimen-failures, invalids, as applicable.
(E) A list of links provided by the device to the user or accessed by the device for internal or external information (e.g., decision rules or databases) supporting clinical significance of test results for the panel or its elements in accordance with paragraphs (b)(1)(v) and (b)(2)(vi) of this section.
(F) A description of internal and external controls that are recommended or provided and control procedures. The description must identify those control elements that are incorporated into the testing procedure.
(iv) Information demonstrating analytical validity of the device according to analytical performance characteristics, evaluated either specifically for each gene/mutation or, when clinically and practically justified, using a representative approach based on other mutations of the same type, including:
(A) Data that adequately supports the intended specimen type (e.g., formalin-fixed, paraffin-embedded tumor tissue), specimen handling protocol, and nucleic acid purification for specific tumor types or for a pan-tumor claim.
(B) A summary of the empirical evidence obtained to demonstrate how the analytical quality metrics and thresholds were optimized.
(C) Device precision data using clinical samples to adequately evaluate intra-run, inter-run, and total variability. The samples must cover all mutation types tested (both positive and negative samples) and include samples near the limit of detection of the device. Precision must be assessed by agreement within replicates on the assay final result for each representative mutation, as applicable, and also supported by sequencing quality metrics for targeted regions across the panel.
(D) Description of the protocols and/or data adequately demonstrating the interchangeability of reagent lots and multiplexing barcodes.
(E) A description of the nucleic acid assay input concentration range and the evidence to adequately support the range.
(F) A description of the data adequately supporting the limit of detection of the device.
(G) A description of the data to adequately support device accuracy using clinical specimens representing the intended specimen type and range of tumor types, as applicable.
(1 ) Clinical specimens tested to support device accuracy must adequately represent the list of cancer mutations with evidence of clinical significance to be detected by the device.
(2 ) For mutations that are designated as cancer mutations with evidence of clinical significance and that are based on evidence established in the intended specimen type (e.g., tumor tissues) but for a different analyte type (e.g., protein, RNA) and/or a measurement (e.g., incorporating a score or copy number) and/or with an alternative technology (e.g., IHC, RT-qPCR, FISH), evidence of accuracy must include clinically adequate concordance between results for the mutation and the medically established biomarker test (e.g., evidence generated from an appropriately sized method comparison study using clinical specimens from the target population).
(3 ) For qualitative DNA mutations not described in paragraph (b)(1)(iv)(G)(2 ) of this section, accuracy studies must include both mutation-positive and wild-type results.
(H) Adequate device stability information.
(v) Information that adequately supports the clinical significance of the panel must include:
(A) Criteria established on what types and levels of evidence will clinically validate a mutation as a cancer mutation with evidence of clinical significance versus a cancer mutation with potential clinical significance.
(B) For representative mutations of those designated as cancer mutations with evidence of clinical significance, a description of the clinical evidence associated with such mutations, such as clinical evidence presented in professional guidelines, as appropriate, with method comparison performance data as described in paragraph (b)(1)(iv)(G) of this section.
(C) For all other mutations designated as cancer mutations with potential clinical significance, a description of the rationale for reporting.
(2) The 21 CFR 809.10 compliant labeling and any product information and test report generated, must include the following, as applicable:
(i) The intended use statement must specify the following:
(A) The test is indicated for previously diagnosed cancer patients.
(B) The intended specimen type(s) and matrix (e.g., formalin-fixed, paraffin-embedded tumor tissue).
(C) The mutation types (e.g., single nucleotide variant, insertion, deletion, copy number variation or gene rearrangement) for which validation data has been provided.
(D) The name of the testing facility or facilities, as applicable.
(ii) A description of the device and summary of the results of the performance studies performed in accordance with paragraphs (b)(1)(iii), (b)(1)(iv), and (b)(1)(v) of this section.
(iii) A description of applicable test limitations, including, for device specific mutations validated with method comparison data to a medically established test in the same intended specimen type, appropriate description of the level of evidence and/or the differences between next generation sequencing results and results from the medically established test (e.g., as described in professional guidelines).
(iv) A listing of all somatic mutations that are intended to be detected by the device and that are reported in the test results under the following two categories or equivalent designations, as appropriate: "cancer mutations panel with evidence of clinical significance" or "cancer mutations panel with potential clinical significance."
(v) For mutations reported under the category of "cancer mutations panel with potential clinical significance," a limiting statement that states "For the mutations listed in [cancer mutations panel with potential clinical significance or equivalent designation], the clinical significance has not been demonstrated [with adequate clinical evidence (e.g., by professional guidelines) in accordance with paragraph (b)(1)(v) of this section] or with this test."
(vi) For mutations under the category of "cancer mutations panel with evidence of clinical significance," or equivalent designation, link(s) for physicians to access internal or external information concerning decision rules or conclusions about the level of evidence for clinical significance that is associated with the marker in accordance with paragraph (b)(1)(v) of this section.
[83 FR 28995, June 22, 2018]
|
|
|
Authority: 21 U.S.C. 351, 360, 360c, 360e, 360j, 360l, 371.
Source: 47 FR 50823, Nov. 9, 1982, unless otherwise noted.
|
|